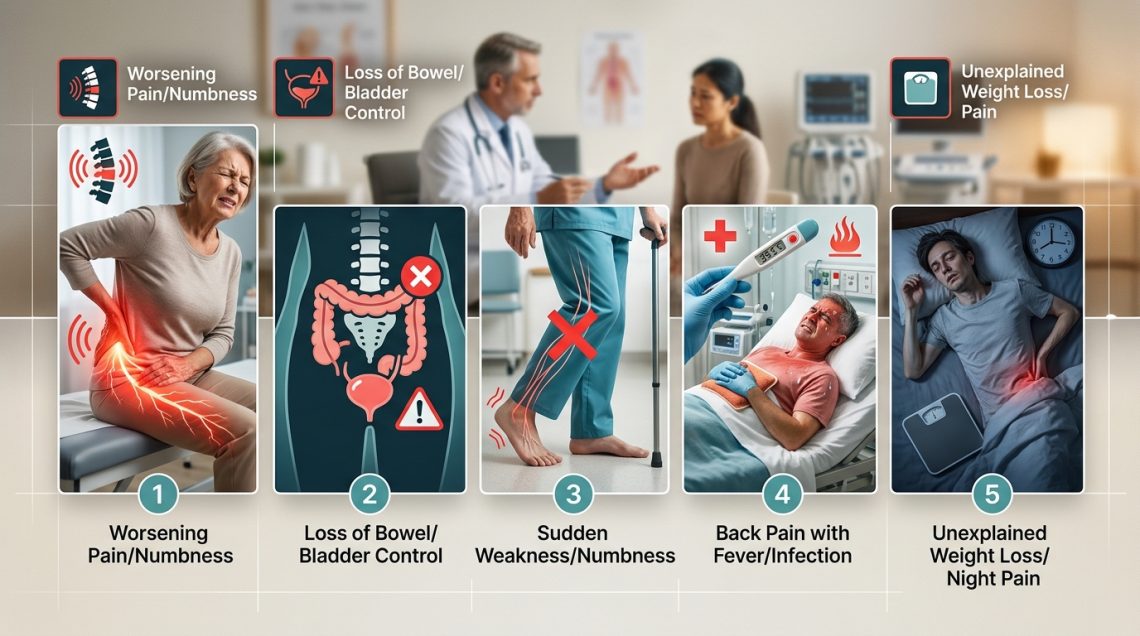
Most back pain goes away on its own within a few weeks. But some symptoms signal something more serious happening inside your body. Knowing the difference between ordinary back pain and warning signs that need immediate medical attention can literally save your life or prevent permanent damage.
Back pain red flags include loss of bowel or bladder control, numbness in the groin area, unexplained weight loss, fever with back pain, severe nighttime pain, weakness in your legs, and pain after significant trauma. These symptoms can indicate serious conditions like spinal cord compression, infections, or fractures that require immediate medical evaluation to prevent permanent damage or life-threatening complications.
Understanding What Makes Back Pain Dangerous
Your spine protects your spinal cord, the highway of nerves connecting your brain to the rest of your body. When something threatens this system, your body sends urgent signals.
These warning signs differ from typical muscle strain or disc issues that improve with rest. Red flags indicate potential damage to nerves, bones, or organs that won’t heal without medical intervention.
Most people experience back pain at some point. About 80% of adults deal with it during their lifetime. The vast majority recover without serious intervention.
But certain symptoms mean you need to act fast.
The Five Most Critical Warning Signs
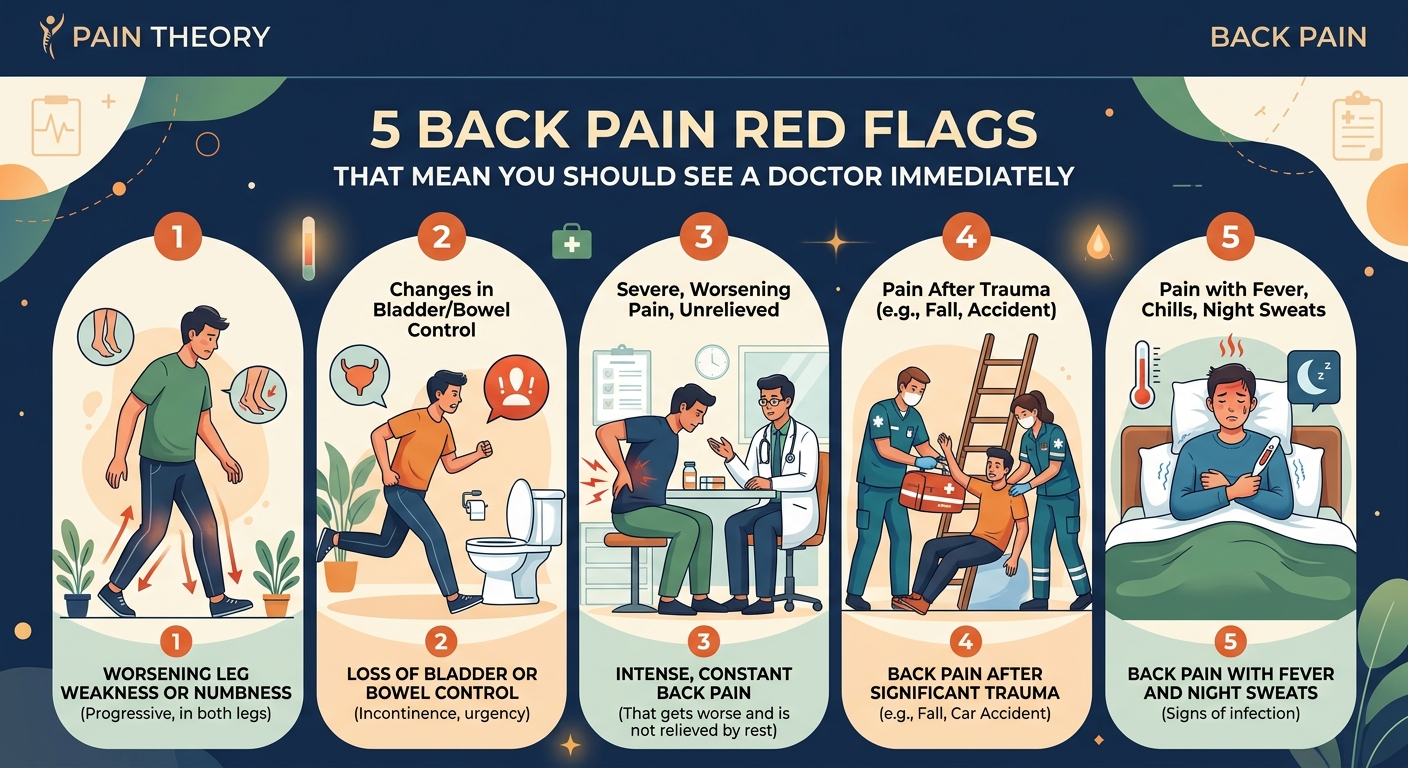
Loss of Bladder or Bowel Control
This is the most urgent red flag. If you suddenly can’t control when you urinate or have a bowel movement, you need emergency care immediately.
This symptom suggests cauda equina syndrome, a condition where nerves at the base of your spinal cord get compressed. Without treatment within 24 to 48 hours, you can suffer permanent nerve damage.
You might also notice:
- Numbness in your inner thighs or groin area (called saddle anesthesia)
- Inability to feel when you need to go to the bathroom
- Difficulty starting urination
- Loss of sexual function
Don’t wait to see if this improves. Call 911 or get to an emergency room.
Numbness or Tingling in Your Groin or Inner Thighs
Even without bladder issues, numbness in the saddle area (the region that would touch a bicycle seat) signals potential nerve compression.
This pattern of numbness is different from leg tingling that follows a sciatica pattern down one leg. Groin numbness affects both sides and indicates pressure on multiple nerve roots at once.
Medical professionals take this symptom very seriously because it often precedes complete loss of bowel and bladder function.
Severe Leg Weakness
Some leg discomfort with back pain is common. But if you notice progressive weakness where you can’t stand on your toes, lift your foot, or climb stairs, that’s different.
Progressive means getting worse over hours or days, not improving with rest.
This can indicate:
- Nerve root compression from a herniated disc
- Spinal stenosis causing cord compression
- Tumor pressing on nerves
- Infection affecting the spine
Test yourself by trying to stand on your toes, then on your heels. If you can’t do both, or if one leg is significantly weaker than the other, seek medical attention.
Fever Combined with Back Pain
Back pain plus fever suggests infection. Spinal infections like epidural abscesses or discitis need immediate treatment with antibiotics or surgery.
You’re at higher risk if you:
- Recently had surgery on your spine
- Use intravenous drugs
- Have a weakened immune system
- Recently had any infection elsewhere in your body
The infection can spread to your spinal cord and cause permanent paralysis if left untreated. Understanding your nervous system’s role in pain signals helps you recognize when something more serious is happening.
Unexplained Weight Loss with Back Pain
Losing weight without trying, combined with back pain, can indicate cancer. This includes cancer that started in the spine or cancer that spread there from another location.
Other concerning symptoms include:
- Pain that gets worse at night when lying down
- Pain that doesn’t improve with rest
- History of cancer
- Age over 50 with new back pain
- Night sweats
Additional Red Flags That Need Attention
Pain After Significant Trauma
If your back pain started after a fall, car accident, or other injury, you might have a fracture. This is especially true for:
- Adults over 50 (bones become more fragile)
- People taking steroids long-term
- Anyone with osteoporosis
- Those who experienced high-impact trauma
Even minor falls can cause fractures in people with weakened bones.
Nighttime Pain That Wakes You Up
Most mechanical back pain (from muscles, discs, or joints) improves when you rest. Pain that gets worse at night or wakes you from sleep can signal:
- Infection
- Tumor
- Inflammatory conditions like ankylosing spondylitis
If you find yourself experiencing worse pain at night, pay attention to other symptoms accompanying it.
Pain That Spreads to Both Legs
Sciatica typically affects one leg. Pain radiating down both legs, especially with numbness or weakness, suggests central spinal canal narrowing.
This bilateral pattern indicates more serious compression than single-sided symptoms.
When to See a Doctor Within 24 Hours
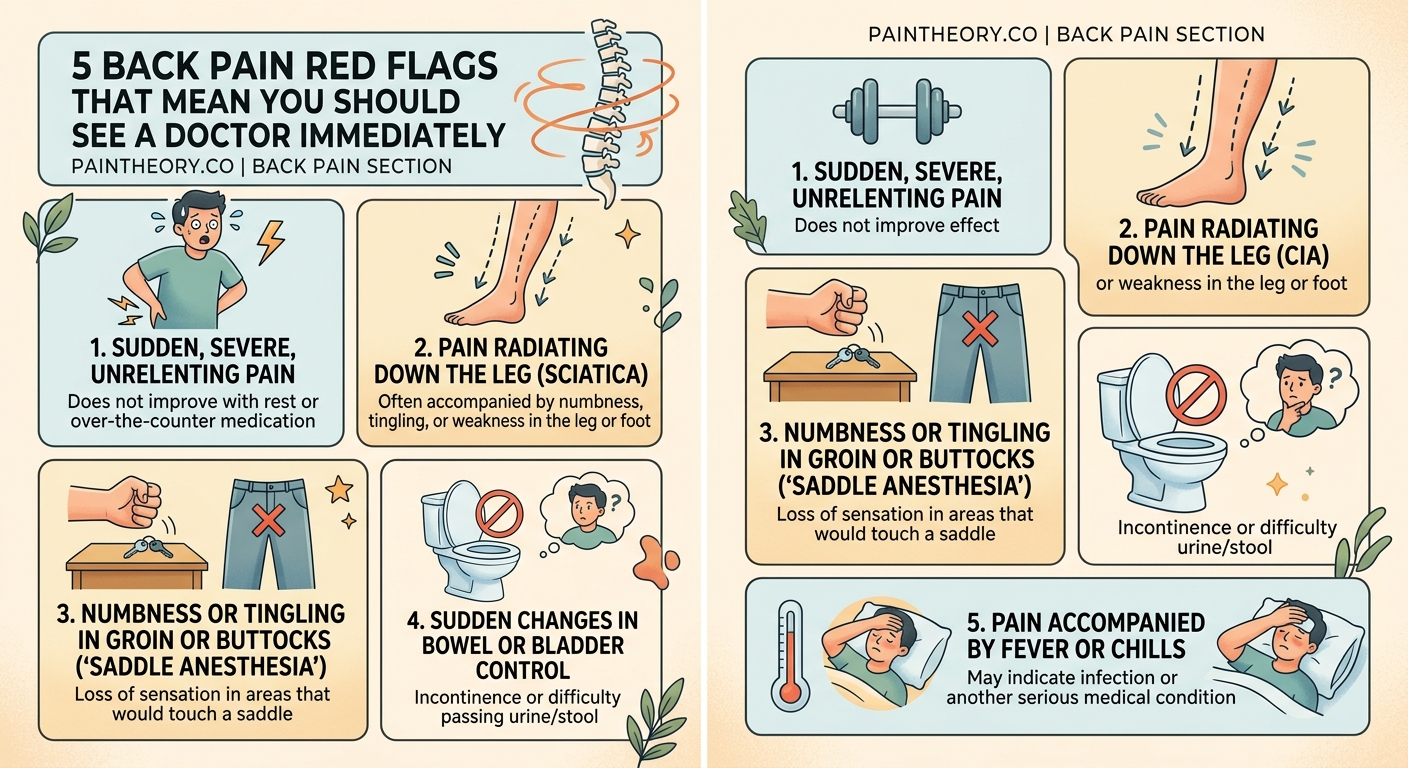
| Symptom | Why It Matters | Urgency Level |
|---|---|---|
| Bladder/bowel loss | Cauda equina syndrome | Emergency (call 911) |
| Groin numbness | Nerve compression | Emergency (same day) |
| Progressive leg weakness | Nerve damage risk | Urgent (within 24 hours) |
| Fever with back pain | Possible infection | Urgent (within 24 hours) |
| Pain after trauma | Potential fracture | Urgent (same day) |
| Unexplained weight loss | Possible tumor | Soon (within few days) |
How Doctors Evaluate Red Flag Symptoms
Your doctor will start with questions about:
- When the pain started and what you were doing
- Whether symptoms are getting better or worse
- What makes the pain better or worse
- Any other medical conditions you have
- Medications you’re taking
They’ll perform a physical exam checking:
- Reflexes in your legs
- Strength in different muscle groups
- Sensation in your legs and groin
- Ability to walk on toes and heels
- Straight leg raise test
Based on findings, they may order:
- X-rays to check for fractures or alignment issues
- MRI to see soft tissues, discs, and nerves
- CT scan for detailed bone images
- Blood tests to check for infection or inflammation
If you have any red flag symptoms, don’t try to tough it out. Early treatment prevents permanent damage and improves outcomes significantly. The difference between seeking care today versus waiting a week can determine whether you recover fully or face lifelong disability.
Common Mistakes People Make
Many people delay seeking care because they:
- Hope the pain will go away on its own
- Don’t want to bother their doctor
- Fear bad news
- Can’t afford medical bills
- Don’t recognize the seriousness of their symptoms
This delay can be catastrophic with red flag symptoms. Conditions like cauda equina syndrome have a narrow window for effective treatment.
Others rush to the emergency room for normal back pain that doesn’t have red flags. This costs more and ties up emergency resources.
Learning to distinguish between the two helps you make better decisions.
What About Chronic Back Pain?
If you’ve had back pain for months or years without red flags, you’re dealing with chronic pain rather than an emergency. Chronic pain involves different mechanisms in your nervous system.
Chronic pain still deserves treatment, but it doesn’t require emergency care unless new red flag symptoms develop.
Watch for changes in your pattern:
- Sudden increase in pain intensity
- New numbness or weakness
- Development of any red flag symptoms
Even longstanding back pain can develop complications that need urgent attention.
Special Considerations for Different Groups
Older Adults
People over 50 face higher risks of:
- Compression fractures from osteoporosis
- Cancer (primary or metastatic)
- Spinal stenosis
- Infections
New back pain after age 50, especially without obvious cause, warrants medical evaluation even without other red flags.
People with Compromised Immune Systems
If you have HIV, take immune-suppressing medications, or have diabetes, you’re more vulnerable to spinal infections.
Lower your threshold for seeking care. Fever with back pain needs same-day evaluation.
Pregnant Women
Back pain is common during pregnancy. But sudden severe pain, especially in the third trimester, can indicate:
- Preterm labor
- Placental abruption
- Kidney infection
Contact your obstetrician if you experience severe back pain with fever, bleeding, or contractions.
Making the Decision to Seek Care
Use this simple decision tree:
- Do you have loss of bladder or bowel control? Go to emergency room now.
- Do you have groin numbness or progressive leg weakness? Go to emergency room today.
- Do you have fever with back pain? See a doctor within 24 hours.
- Do you have pain after significant trauma? See a doctor today.
- Do you have unexplained weight loss or severe nighttime pain? Schedule appointment within a few days.
- Do you have ordinary back pain improving with rest? Try home care, see doctor if not better in a few weeks.
When in doubt, err on the side of caution. A doctor visit that turns out to be unnecessary is better than missing a serious condition.
Treatment Options for Red Flag Conditions
Treatment depends on the underlying cause:
- Cauda equina syndrome: Emergency surgery to decompress nerves
- Spinal infection: IV antibiotics, sometimes surgery
- Fracture: Bracing, pain management, sometimes vertebroplasty
- Tumor: Depends on type; may include surgery, radiation, chemotherapy
- Severe disc herniation: Medications, injections, or surgery
Early treatment dramatically improves outcomes for all these conditions.
Protecting Yourself Going Forward
After addressing immediate red flags, focus on spine health:
- Maintain healthy weight to reduce spine stress
- Exercise regularly to strengthen core muscles
- Practice good posture at work and home
- Lift heavy objects properly
- Don’t smoke (it impairs disc healing)
- Manage chronic conditions like diabetes
These habits won’t prevent all back problems, but they reduce your risk of serious complications.
Trusting Your Instincts About Your Body
You know your body better than anyone else. If something feels seriously wrong, trust that instinct.
Medical professionals would rather evaluate you and find nothing serious than have you wait at home while a treatable condition becomes permanent.
Don’t let embarrassment about bowel or bladder symptoms delay care. Doctors see these issues regularly and understand the urgency.
Don’t minimize your symptoms because you’re busy or don’t want to worry family members. Your health comes first.
Getting the Care You Need Right Now
Back pain red flags represent your body’s emergency broadcast system. These symptoms exist to protect you from permanent harm.
Most back pain is not an emergency. But when red flags appear, acting fast makes all the difference. The nervous system doesn’t wait, and neither should you. Trust the warning signs, seek appropriate care, and give yourself the best chance for complete recovery.