Your shoulders feel like concrete blocks. Your lower back aches every time you sit down. You’ve tried stretching, bought a new chair, and even changed your mattress. But the pain keeps coming back, especially during your busiest weeks at work or when family tension runs high. If this sounds familiar, you’re not imagining things. Stress doesn’t just live in your head. It creates real, measurable changes in your body that can absolutely cause back pain.
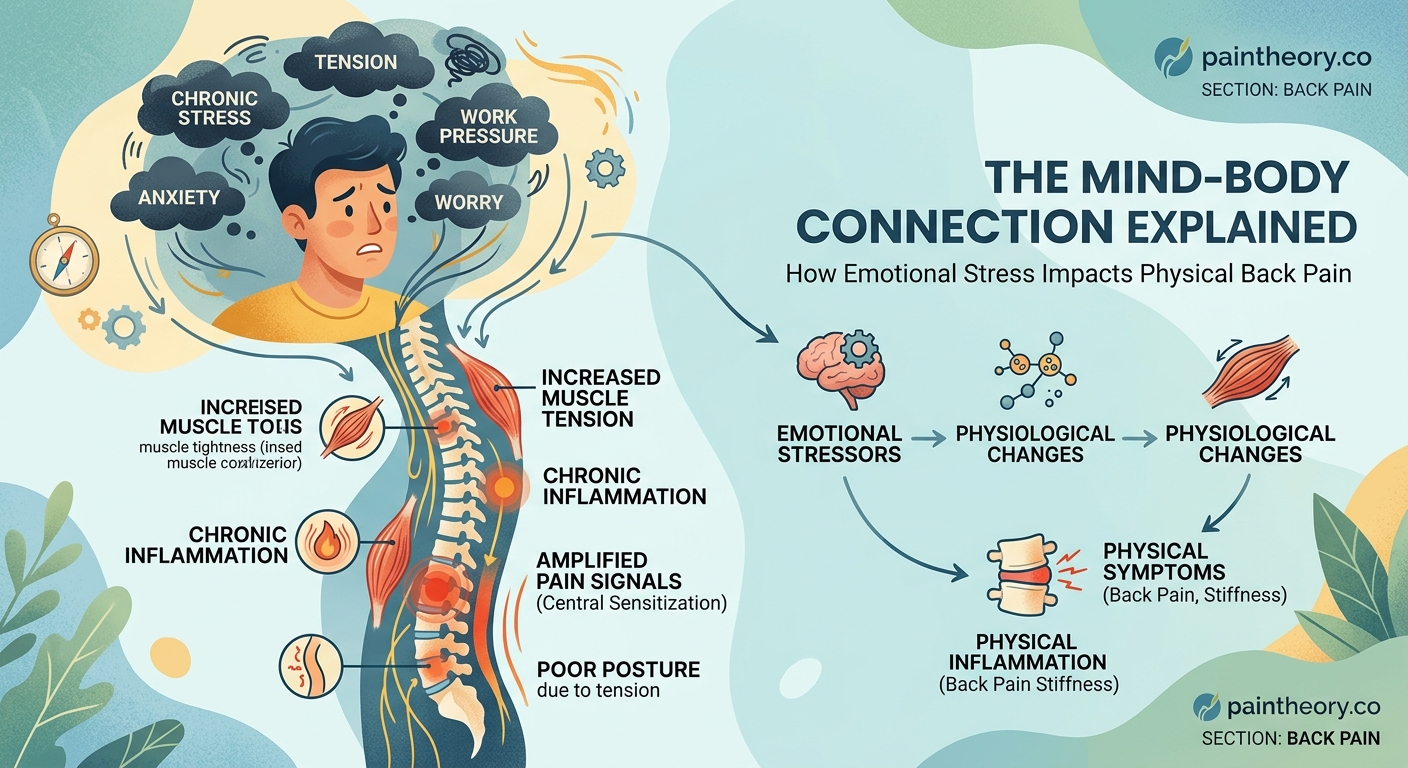
Stress triggers a cascade of physical responses that directly cause back pain through muscle tension, inflammation, altered posture, and nervous system sensitization. The connection between emotional stress and physical back pain is backed by decades of research showing how cortisol, muscle guarding, and pain perception changes create a very real cycle. Understanding these mechanisms helps you address both the mental and physical components for lasting relief.
How Stress Physically Changes Your Back Muscles
When your brain perceives a threat, whether it’s a looming deadline or an argument with your partner, it activates your sympathetic nervous system. This ancient survival mechanism floods your body with stress hormones like cortisol and adrenaline.
Your muscles respond immediately. They contract and brace for action.
This works perfectly if you’re facing a genuine physical danger. The problem starts when the threat is psychological and never goes away. Your muscles stay partially contracted for hours, days, or even weeks.
The trapezius muscles in your upper back and shoulders are particularly vulnerable. They tighten first and stay tight longest. Your lower back muscles, especially the erector spinae group along your spine, do the same thing.
This constant low-level contraction creates several problems:
- Reduced blood flow to muscle tissue
- Buildup of metabolic waste products like lactic acid
- Decreased oxygen delivery to muscle cells
- Formation of trigger points (those painful knots you can feel)
- Compression of small nerves between muscle fibers
The result is genuine tissue irritation and pain. Not imagined pain. Not “all in your head” pain. Real structural changes that hurt.
The Cortisol Connection to Back Pain

Cortisol does more than just prepare you for fight or flight. When levels stay elevated for extended periods, this hormone actually changes how your body processes pain signals.
Research shows that chronic stress and elevated cortisol increase systemic inflammation throughout your body. This inflammatory state makes nerve endings more sensitive to pain signals. Your pain threshold effectively drops.
Here’s what happens at the tissue level:
- Cortisol triggers the release of pro-inflammatory cytokines
- These molecules increase tissue sensitivity and swelling
- Your immune system stays in a heightened state of alert
- Normal sensations that wouldn’t usually register as painful now do
- The pain signals get amplified as they travel to your brain
This explains why the same movement that felt fine last month now makes you wince. Your tissues haven’t necessarily changed that much. Your nervous system’s interpretation of those signals has shifted.
People experiencing chronic stress often notice their back pain gets worse at night when cortisol levels naturally fluctuate and the day’s accumulated tension reaches its peak.
Stress-Related Posture Changes That Hurt Your Back
Watch someone during a stressful phone call. Their shoulders creep up toward their ears. Their head juts forward. Their spine rounds.
These postural shifts happen automatically and unconsciously. But they create significant mechanical stress on your back structures.
Forward head posture is particularly damaging. For every inch your head moves forward from neutral alignment, it adds approximately 10 pounds of extra force on your neck and upper back muscles. During a stressful day at your computer, you might maintain this position for hours without realizing it.
Your lower back suffers too. Stress often causes people to:
- Clench their abdominal muscles
- Tilt their pelvis forward or backward
- Lock their knees when standing
- Shift weight unevenly between feet
- Hold their breath or breathe shallowly
Each of these compensations forces your back muscles to work harder to maintain balance. Over time, some muscles become overworked and painful while others weaken from disuse.
The Breath-Pain Connection You Might Be Missing
Stress changes how you breathe. Most people shift from deep belly breathing to shallow chest breathing when anxious or overwhelmed.
This matters more than you might think.
Shallow breathing keeps your accessory breathing muscles (in your neck, shoulders, and upper back) constantly engaged. These muscles aren’t designed for continuous use. They’re meant for occasional help during exercise or emergencies.
When you use them all day, every day, they become overworked and painful. The scalene muscles in your neck, the upper trapezius, and the levator scapulae all develop trigger points and chronic tension.
Shallow breathing also reduces oxygen delivery to all your tissues, including your back muscles. Less oxygen means slower recovery, more metabolic waste buildup, and increased pain sensitivity.
“The diaphragm is your body’s primary breathing muscle, but stress essentially hijacks this system. When patients learn to restore proper diaphragmatic breathing, we often see a 30-40% reduction in reported back pain within just two weeks.” (Dr. Sarah Chen, Physical Medicine and Rehabilitation)
Why Stress Makes Existing Back Problems Worse
If you already have a back condition like a herniated disc, arthritis, or old injury, stress acts as an amplifier.
The pain doesn’t exist only in the damaged tissue. Pain is an experience created by your brain based on multiple inputs. When you’re stressed, your brain becomes more likely to interpret ambiguous signals as dangerous.
This is part of a process called central sensitization. Your nervous system essentially turns up the volume on pain signals. Movements or positions that caused mild discomfort before now trigger intense pain.
Understanding why pain becomes chronic helps explain why managing stress is just as important as treating the structural problem.
Practical Ways to Break the Stress-Pain Cycle
Knowing that stress causes back pain is useful. But you need concrete strategies to interrupt this cycle.
Here’s a systematic approach that addresses both the mental and physical components:
-
Establish a daily breathing practice. Set three alarms on your phone. When they go off, stop and take five slow belly breaths. Inhale for four counts, exhale for six counts. This activates your parasympathetic nervous system and releases muscle tension.
-
Schedule movement breaks every 30 minutes. Stand up, roll your shoulders back, do three gentle spinal twists each direction. Movement prevents the sustained muscle contraction that builds throughout the day.
-
Create a stress release routine before bed. Spend 10 minutes doing gentle stretches, progressive muscle relaxation, or foam rolling. This signals your nervous system that the day’s demands are over.
-
Track your pain patterns alongside your stress levels. Use a simple notebook or app to record both. You’ll likely see clear correlations that help you identify your specific triggers.
-
Address sleep quality aggressively. Poor sleep increases both stress hormones and pain sensitivity. If pain disrupts your sleep, read about how to sleep better when chronic pain keeps you awake.
Common Mistakes That Keep You Stuck
Many people unknowingly sabotage their recovery by making these errors:
| Mistake | Why It Hurts | Better Approach |
|---|---|---|
| Ignoring pain until it’s severe | Allows nervous system sensitization to deepen | Address tension and stress daily, even when pain is mild |
| Only treating the physical symptoms | Misses the stress component driving muscle tension | Combine physical therapy with stress management techniques |
| Pushing through pain during exercise | Reinforces pain pathways and increases inflammation | Respect pain signals and modify activities appropriately |
| Relying only on medication | Doesn’t address underlying muscle tension or stress response | Use medication as one tool among many |
| Waiting for stress to naturally decrease | Chronic stress rarely resolves without active intervention | Build regular stress-reduction practices into your routine |
The biggest mistake is treating stress and back pain as separate problems. They’re interconnected parts of the same cycle.
When Professional Help Makes Sense
Some situations require more than self-care strategies. Consider seeking professional support if:
- Your pain persists beyond three months despite home management
- Pain intensity increases over time rather than improving
- You develop new neurological symptoms like numbness, tingling, or weakness
- Pain significantly disrupts your work, relationships, or daily activities
- You notice increasing anxiety or depression alongside physical symptoms
A comprehensive treatment team might include a physical therapist who understands pain science, a psychologist trained in cognitive behavioral therapy for pain, and a physician who can rule out serious structural problems.
For some people with persistent pain, interventional procedures might be appropriate. Learn more about when to consider surgery for chronic pain relief, though most stress-related back pain responds well to conservative treatment.
The Science Behind Mind-Body Treatments
Multiple research studies confirm that addressing the psychological component of back pain produces measurable physical improvements.
A 2019 study in the Journal of the American Medical Association found that cognitive behavioral therapy reduced back pain intensity by an average of 30% and improved function scores by 40%. These benefits lasted for at least 12 months after treatment ended.
Mindfulness-based stress reduction programs show similar results. Participants report less pain, use fewer pain medications, and demonstrate actual changes in brain imaging studies. The parts of the brain that process pain signals become less reactive.
These aren’t placebo effects. They’re real neurological changes that alter how your nervous system processes and responds to pain signals.
Building Your Personal Stress-Pain Prevention Plan
Everyone’s stress triggers and pain patterns are unique. Your prevention plan needs to match your specific situation.
Start by identifying your high-risk periods:
- Certain times of day (morning rush, evening after work)
- Specific situations (meetings, family gatherings, financial tasks)
- Seasonal patterns (tax season, holidays, back-to-school time)
- Life transitions (job changes, moves, relationship shifts)
Once you know when you’re most vulnerable, you can build targeted interventions into those times.
For example, if your back pain flares during busy work periods, you might:
- Block 10-minute movement breaks in your calendar
- Use a standing desk for afternoon hours
- Practice breathing exercises before stressful meetings
- Schedule a massage or physical therapy appointment during peak stress weeks
Prevention is always easier than treatment. Small daily practices compound over weeks and months to create significant change.
Your Body Is Listening to Your Mind
The connection between stress and back pain isn’t weakness or failure. It’s basic human biology.
Your nervous system evolved to protect you from danger. When it perceives threat, whether physical or psychological, it creates tension and heightened sensitivity. This response served our ancestors well when dangers were brief and physical.
Modern life presents a different challenge. The threats are constant, psychological, and rarely resolved through physical action. Your body maintains its protective response indefinitely, creating chronic muscle tension and pain.
Understanding this connection gives you power. You can’t always control the stressors in your life, but you can change how your body responds to them. Every breathing exercise, every movement break, every moment of mindfulness sends a signal to your nervous system that it’s safe to relax.
Your back pain is real. The solution just might involve calming your mind as much as treating your muscles.