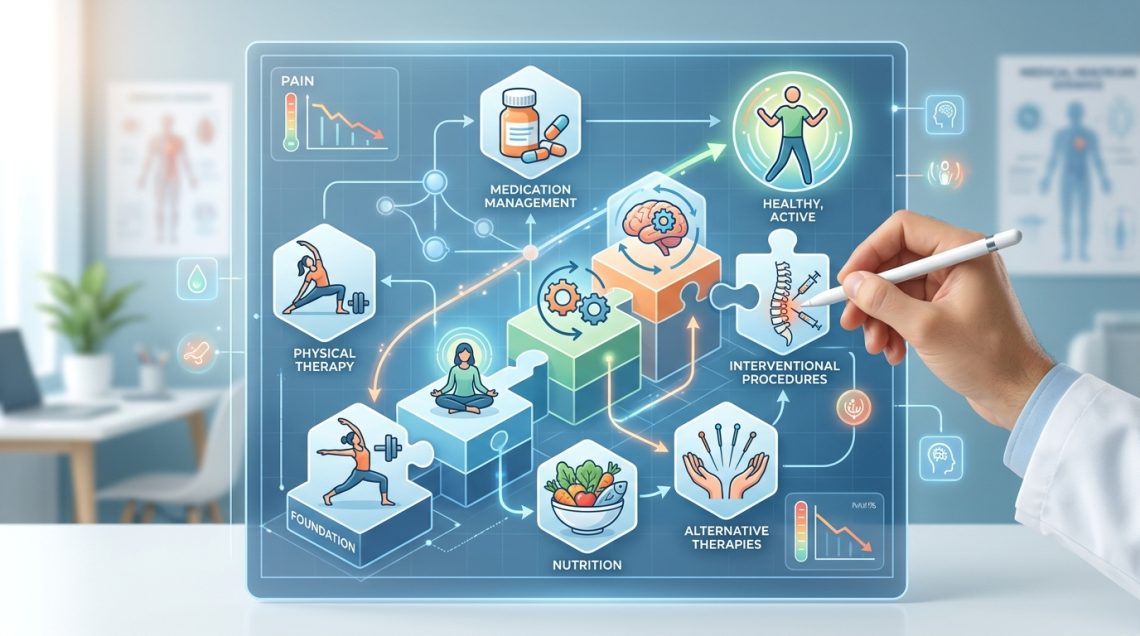
Living with chronic pain feels like carrying an invisible weight that nobody else can see. You’ve probably tried medication after medication, only to find that pills alone don’t give you the relief you need. That’s where a multimodal pain management plan comes in, combining different treatment approaches to target your pain from multiple angles at once.
A multimodal pain management plan combines multiple treatment strategies including medications, physical therapy, psychological support, and lifestyle modifications to address chronic pain more effectively than any single approach. This comprehensive method targets pain through different biological pathways, reducing reliance on opioids while improving function and quality of life. Success requires coordination between healthcare providers and active patient participation in treatment decisions.
What Makes Multimodal Pain Management Different
Traditional pain treatment often relies heavily on a single approach, usually medication. You take a pill, hope it works, and increase the dose when it stops helping.
Multimodal pain management works differently.
Instead of putting all your eggs in one basket, this approach combines several evidence-based treatments that work through different mechanisms. One therapy might reduce inflammation while another retrains your nervous system’s pain response. Together, they create a stronger effect than any single treatment could achieve alone.
Think of it like fixing a leaky roof. You wouldn’t just throw a tarp over the hole and call it done. You’d repair the shingles, check the underlayment, seal the flashing, and maybe improve the gutters too. Each fix addresses a different part of the problem.
Your pain works the same way. It involves physical damage, nerve sensitization, inflammation, muscle tension, stress responses, and learned patterns. Addressing just one piece leaves the others untouched.
Core Components of an Effective Plan
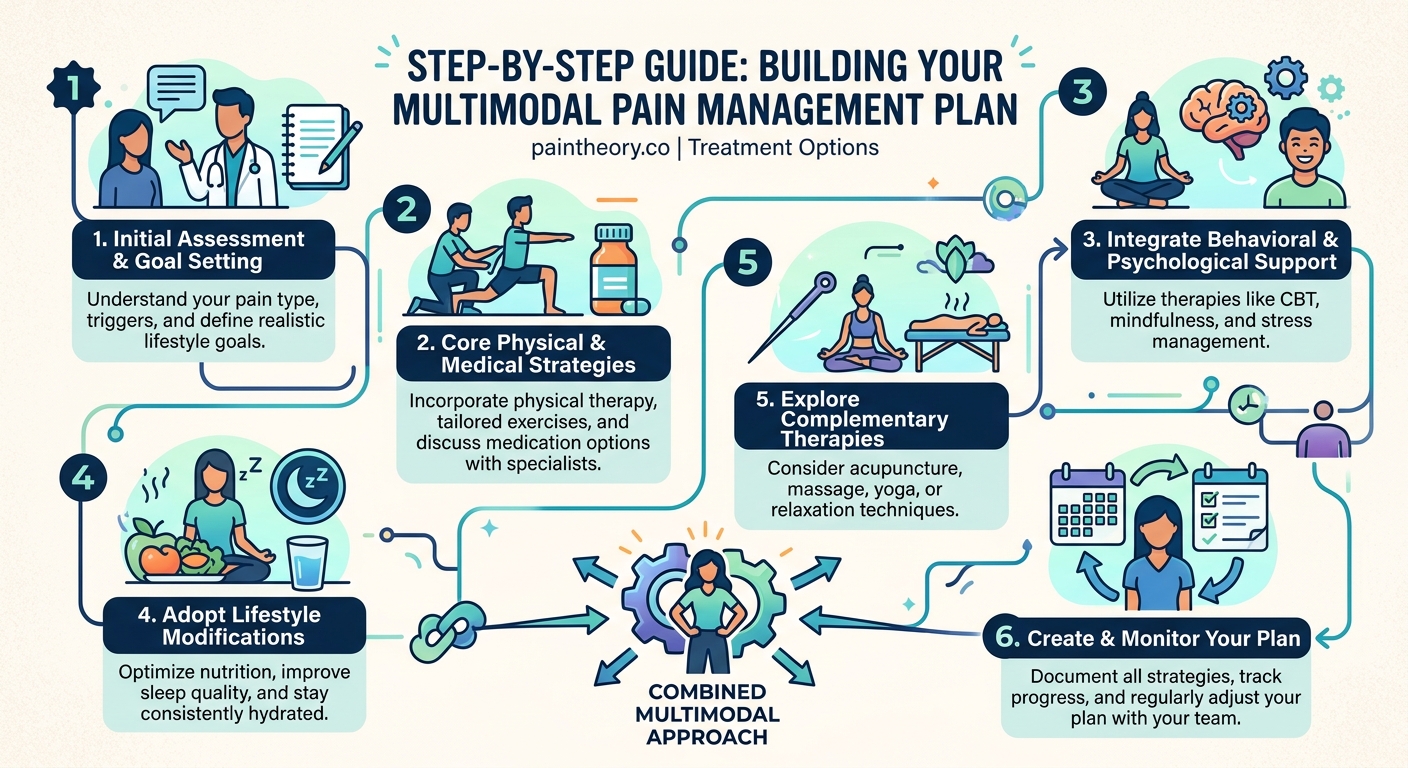
Building your multimodal pain management plan means selecting treatments from different categories that complement each other. Here are the main pillars:
Pharmacological treatments include medications that work through different pathways. You might combine a non-opioid pain reliever with a medication that calms overactive nerves, rather than relying on a single drug at high doses.
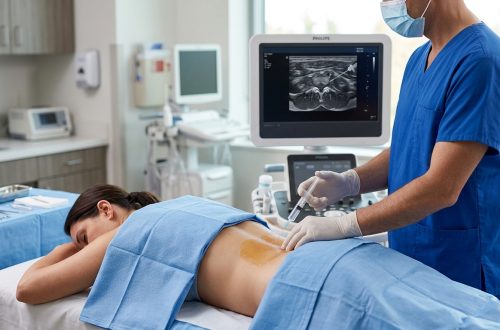
Physical interventions encompass everything from physical therapy and exercise to targeted nerve blocks and injections that deliver relief directly to pain sources.
Psychological approaches address how your brain processes and responds to pain signals. Cognitive behavioral therapy, mindfulness, and biofeedback can actually change your pain experience at a neurological level.
Lifestyle modifications include sleep optimization, nutrition changes like following an anti-inflammatory diet, and stress management techniques.
Complementary therapies such as acupuncture, massage, and heat or cold therapy provide additional relief mechanisms that support your primary treatments.
Step-by-Step Guide to Building Your Plan
Creating an effective multimodal pain management plan takes intentional planning and collaboration with your healthcare team. Here’s how to approach it:
-
Document your current pain experience thoroughly. Keep a detailed pain diary for at least two weeks, noting pain levels, triggers, what helps, what makes it worse, and how pain affects your daily activities. This baseline data helps you and your providers identify patterns and measure progress.
-
Assemble your care team. Depending on your condition, this might include your primary care physician, a pain specialist, physical therapist, psychologist, and other specialists. Make sure they can communicate with each other about your treatment.
-
Set realistic, specific goals. Rather than “reduce pain,” aim for measurable outcomes like “sleep through the night four times per week” or “walk for 20 minutes without increased pain.” These concrete targets help you track whether your plan is working.
-
Select treatments from multiple categories. Work with your providers to choose at least three different types of interventions. For example, you might combine medication management, weekly physical therapy, and daily mindfulness practice.
-
Create an implementation schedule. Some treatments work immediately while others take weeks or months. Plan when you’ll start each intervention and how long you’ll try it before evaluating effectiveness.
-
Establish checkpoints for assessment. Schedule regular reviews with your care team, typically every 4-8 weeks initially, to evaluate what’s working and what needs adjustment.
-
Build in flexibility for modifications. Your plan should evolve based on your response. What works initially might need adjustment as your condition changes or as you reach new functional levels.
Common Treatment Combinations That Work
Different pain conditions respond better to specific treatment combinations. Here’s what research and clinical experience show works well:
| Pain Condition | Effective Combination | Why It Works |
|---|---|---|
| Chronic back pain | Physical therapy + NSAIDs + cognitive behavioral therapy | Addresses muscle weakness, inflammation, and pain catastrophizing simultaneously |
| Fibromyalgia | Low-dose antidepressants + gentle exercise + sleep hygiene | Targets central sensitization, improves conditioning, and breaks the pain-insomnia cycle |
| Post-surgical pain | Scheduled acetaminophen + nerve blocks + early mobilization | Prevents pain from becoming chronic while promoting healing |
| Arthritis pain | Anti-inflammatory medication + joint protection techniques + aquatic therapy | Reduces inflammation while maintaining joint function without excess stress |
| Neuropathic pain | Anticonvulsants + physical therapy + topical treatments | Calms overactive nerves through systemic and local mechanisms |
The specific combination that works best for you depends on your individual pain mechanisms, overall health, preferences, and treatment goals.
Medication Strategies Within Multimodal Plans
Medications remain an important component, but the multimodal approach uses them more strategically.
Instead of relying on a single medication at high doses, you might use smaller doses of several medications that work through different mechanisms. This often provides better pain relief with fewer side effects.
For example, combining acetaminophen with a topical anti-inflammatory and a medication that targets nerve pain might control your symptoms better than a high dose of opioids alone.
Comparing pain medications helps you understand which options target your specific pain type most effectively.
“The goal isn’t to eliminate all pain, which is often unrealistic. The goal is to reduce pain enough that you can participate in the physical therapy, exercise, and other activities that will improve your long-term function.” – Pain management specialists consistently emphasize this practical perspective.
Physical and Functional Rehabilitation
Movement might be the last thing you want to do when you’re hurting, but appropriate physical activity is one of the most powerful pain treatments available.
Physical therapy does more than strengthen muscles. It retrains movement patterns, reduces fear of movement, improves flexibility, and can actually change how your nervous system processes pain signals.
The 15-minute daily stretching routine offers a practical starting point if you’re new to movement-based pain management.
Your physical rehabilitation should start where you are, not where you think you should be. If walking to the mailbox is your current limit, that’s your starting point. Gradual, consistent progress beats sporadic intense effort every time.
Psychological and Behavioral Interventions
Your brain plays a massive role in how you experience pain. Understanding your nervous system’s role helps you appreciate why psychological interventions aren’t just “in your head” but actually change your physical pain experience.
Cognitive behavioral therapy for pain teaches you to recognize and modify thoughts and behaviors that amplify pain. You learn to challenge catastrophic thinking, pace activities effectively, and respond to pain flares constructively rather than reactively.
Mindfulness and meditation practices help you change your relationship with pain. Rather than fighting against every sensation, you learn to observe pain without adding layers of stress and emotional suffering on top of the physical experience.
Biofeedback training teaches you to control physiological responses you normally can’t feel, like muscle tension or skin temperature. This gives you tangible tools to reduce pain in real-time.
Stress management techniques provide additional strategies for reducing the emotional amplification of pain signals.
Lifestyle Modifications That Support Pain Relief
Small daily choices add up to significant impacts on chronic pain.
Sleep quality and pain exist in a vicious cycle. Pain disrupts sleep, and poor sleep lowers your pain threshold. Improving your sleep when chronic pain keeps you awake becomes a critical part of your overall pain management strategy.
Nutrition affects inflammation levels throughout your body. While food won’t cure chronic pain, an anti-inflammatory eating pattern can reduce the biological processes that sensitize pain pathways.
Activity pacing prevents the boom-and-bust cycle where you overdo it on good days and pay for it with increased pain afterward. Learning to spread activities evenly and take breaks before pain escalates helps maintain more consistent function.
Work modifications matter too. Managing chronic pain at your desk job requires specific strategies to prevent workplace activities from sabotaging your pain management efforts.
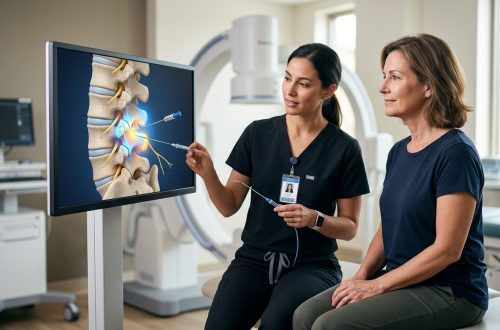
Interventional Procedures in Multimodal Care
Sometimes your plan needs more targeted interventions. These procedures deliver treatment directly to pain sources.
Nerve blocks temporarily interrupt pain signals, providing relief and sometimes resetting sensitized pain pathways. They work especially well when combined with physical therapy during the pain-free window they create.
Epidural steroid injections reduce inflammation around compressed nerves, buying time for other treatments to work and sometimes avoiding surgery.
Radiofrequency ablation uses heat to interrupt nerve signals from painful joints or other structures, providing relief that can last months or longer.
These procedures work best as part of a comprehensive plan, not as standalone solutions. The relief they provide creates opportunities to engage more fully with physical therapy, exercise, and other active treatments.
Tracking Progress and Adjusting Your Plan
Your multimodal pain management plan should evolve based on results, not remain static.
Track multiple outcomes, not just pain levels:
- Functional abilities (what you can do)
- Sleep quality and duration
- Mood and emotional wellbeing
- Medication usage and side effects
- Activity tolerance
- Quality of life measures
Some improvements show up quickly while others take months. Medication changes might provide relief within days, but the benefits of physical therapy or psychological interventions often build gradually over 8-12 weeks.
Don’t abandon treatments too quickly, but also don’t persist indefinitely with approaches that clearly aren’t helping. Your regular checkpoints with providers help you make these judgment calls based on objective data rather than daily fluctuations.
Common Mistakes to Avoid
Even well-designed multimodal plans can fail if you fall into these traps:
| Mistake | Why It Happens | How to Avoid It |
|---|---|---|
| Trying everything at once | Eagerness for relief | Start 1-2 new treatments at a time so you can identify what helps |
| Stopping treatments when pain improves | Assuming you’re “cured” | Maintain effective treatments and taper gradually under supervision |
| Expecting complete pain elimination | Unrealistic goals | Aim for meaningful functional improvement and pain reduction |
| Skipping “homework” between appointments | Passive treatment mindset | Remember that what you do daily matters more than weekly appointments |
| Not communicating between providers | Assuming they talk to each other | Take responsibility for ensuring your team knows what others are doing |
When to Consider Adjusting Your Approach
Your multimodal pain management plan needs revision when:
You’ve followed the plan consistently for the agreed-upon trial period (usually 8-12 weeks) without meaningful improvement. Some treatments need time, but there should be at least small positive changes within this timeframe.
Side effects from one component outweigh its benefits. Every treatment involves tradeoffs, but the balance should favor improvement.
Your pain pattern changes significantly. A new injury, disease progression, or shift in pain characteristics might require different treatment combinations.
You reach a plateau where progress stalls. This often means it’s time to add new challenges or interventions rather than continuing the same routine.
Life circumstances change in ways that affect your ability to follow the plan. A new job, move, or family situation might require adapting your approach to fit new realities.
Recognizing when to consider surgery becomes relevant if conservative multimodal approaches don’t provide adequate relief after thorough trials.
Putting Your Plan Into Action
The best multimodal pain management plan in the world doesn’t help if it stays on paper.
Start by choosing one or two changes you can implement this week. Maybe that means scheduling your first physical therapy appointment and starting a pain diary. Small, consistent steps build momentum better than trying to overhaul everything overnight.
Communicate openly with your healthcare team about what’s realistic for you. If daily exercises aren’t feasible with your work schedule, say so. If a medication causes side effects you can’t tolerate, speak up immediately. Your providers can’t adjust what they don’t know about.
Remember that managing chronic pain is a marathon, not a sprint. Some days will feel discouraging. You might have flares that make you question whether anything is working. That’s normal and doesn’t mean your plan is failing.
The combination of treatments that addresses your pain from multiple angles gives you the best chance of reclaiming function and improving your quality of life. Your pain might not disappear completely, but with persistence and the right multimodal approach, it can stop controlling your life.