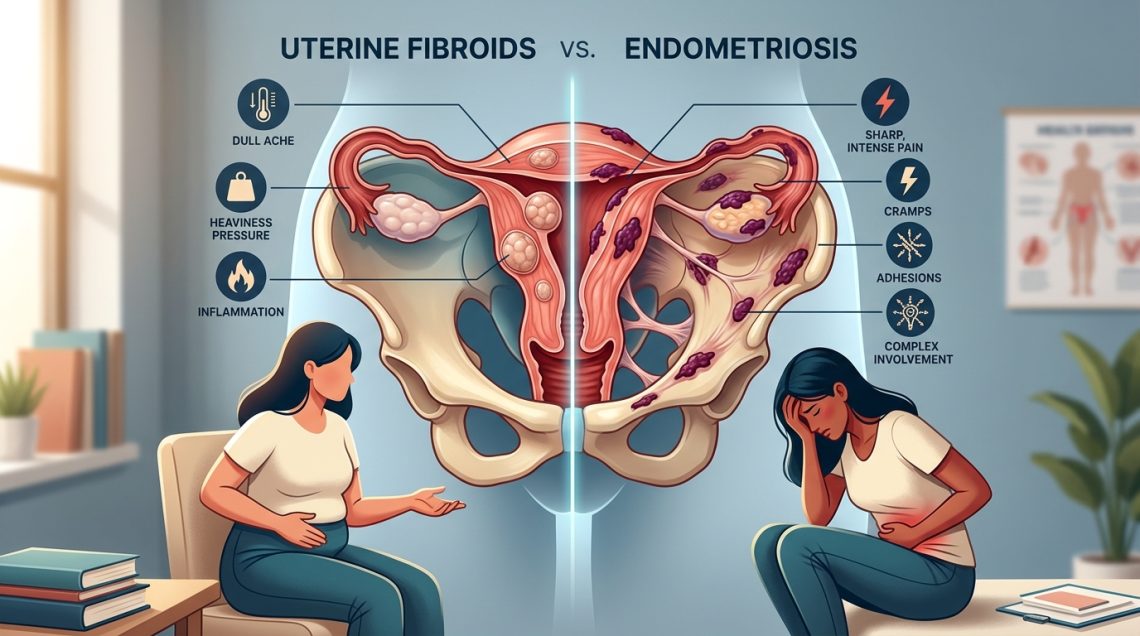
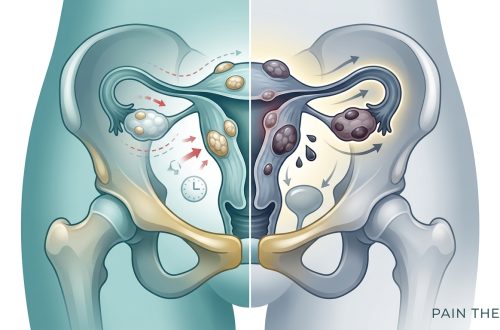
You’ve been dealing with pelvic pain for months. Your periods are getting heavier. You’re exhausted all the time, and you’re wondering if what you’re experiencing is fibroids or endometriosis. These two conditions share enough symptoms to confuse even the most informed women, but they’re fundamentally different problems that require different treatments. Getting the right diagnosis matters because the wrong treatment plan won’t help and might even delay relief.
Fibroids are benign tumors growing in or on the uterus, while endometriosis involves uterine lining tissue growing outside the uterus. Fibroids typically cause heavy bleeding and pelvic pressure, whereas endometriosis creates cyclical pain that worsens during periods. Diagnosis requires imaging for fibroids and often laparoscopy for endometriosis. Treatment ranges from medication to surgery, depending on severity, symptoms, and whether you want to preserve fertility.
What fibroids and endometriosis actually are
Fibroids are muscular tumors that grow in the wall of your uterus. They’re almost always benign, meaning they won’t become cancer. They can range from the size of a pea to larger than a grapefruit. Some women have one fibroid, while others develop multiple growths.
Endometriosis is a completely different problem. The tissue that normally lines the inside of your uterus starts growing in places it shouldn’t, like your ovaries, fallopian tubes, or the outer surface of your uterus. During your menstrual cycle, this misplaced tissue behaves like normal uterine lining. It thickens, breaks down, and bleeds. But because it has nowhere to go, it causes inflammation, scarring, and adhesions.
The confusion happens because both conditions affect your reproductive organs and can cause pain. But the mechanisms are entirely different.
How the symptoms differ between the two
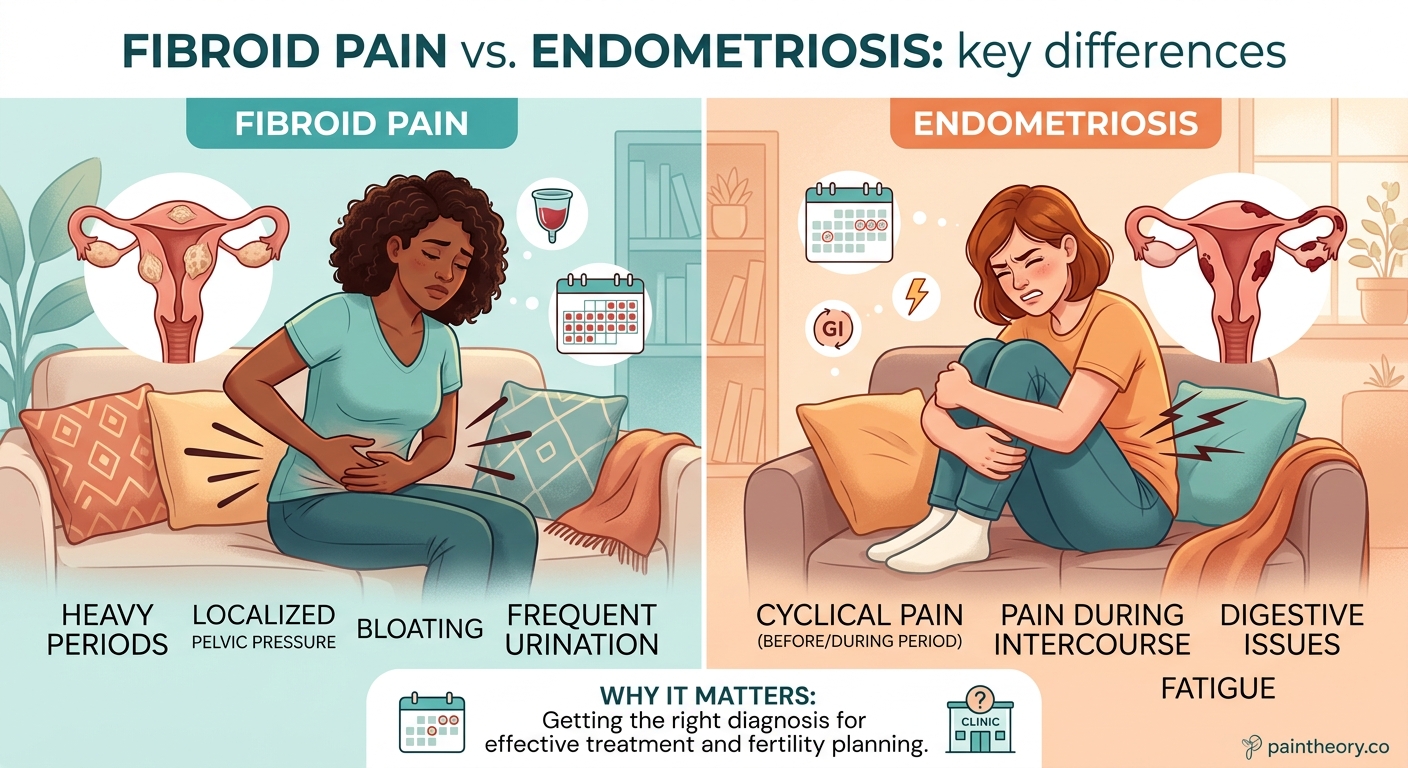
Both conditions can cause pelvic pain, but the quality and timing of that pain often differ.
Fibroid symptoms typically include:
- Heavy menstrual bleeding that soaks through pads or tampons every hour
- Periods lasting longer than seven days
- Pelvic pressure or fullness, especially as fibroids grow larger
- Frequent urination when fibroids press against your bladder
- Constipation or bloating when fibroids press on your bowels
- Lower back pain from larger fibroids
- Pain during sex, particularly with certain positions
Endometriosis symptoms usually involve:
- Severe menstrual cramps that worsen over time
- Chronic pelvic pain that follows your cycle
- Pain during or after sex, often deep penetration
- Pain with bowel movements or urination during periods
- Excessive bleeding or spotting between periods
- Fatigue that intensifies around your period
- Digestive issues like diarrhea, constipation, or nausea during menstruation
- Difficulty getting pregnant
One key difference: endometriosis pain typically follows a cyclical pattern tied to your menstrual cycle. The pain often starts a few days before your period and continues through it. Why does endometriosis pain feel worse during your period has to do with hormonal fluctuations that trigger inflammation in the misplaced tissue.
Fibroid pain tends to be more constant and related to the physical presence of the growths. As they get larger, they create more pressure. The pain doesn’t necessarily sync with your cycle the same way endometriosis does.
Getting the right diagnosis
Your doctor will use different approaches to diagnose each condition.
For fibroids
- A pelvic exam can detect larger fibroids when your doctor feels an irregularly shaped uterus.
- An ultrasound (either abdominal or transvaginal) shows fibroids clearly and measures their size and location.
- An MRI provides detailed images if surgery is being considered or if the ultrasound results are unclear.
- A hysteroscopy allows your doctor to look inside your uterus with a thin, lighted tube to see fibroids growing into the uterine cavity.
For endometriosis
- A pelvic exam might reveal tender areas or cysts, but many women with endometriosis have normal exams.
- An ultrasound can sometimes detect endometriomas (ovarian cysts caused by endometriosis) but often misses smaller patches of tissue.
- An MRI can identify larger areas of endometriosis but isn’t sensitive enough to catch everything.
- A laparoscopy is the gold standard. Your surgeon makes a small incision and uses a camera to look directly at your pelvic organs, identifying and often removing endometrial tissue during the same procedure.
The frustrating reality is that endometriosis takes an average of seven to ten years to diagnose. Many women are told their pain is normal or psychological before getting proper testing.
If you’re experiencing symptoms but haven’t received clear answers, 7 early warning signs of fibroids most women ignore until it’s too late might help you identify patterns worth discussing with your doctor.
Treatment approaches for each condition

The right treatment depends on your symptoms, the severity of your condition, your age, and whether you want to have children.
| Treatment Type | Fibroids | Endometriosis |
|---|---|---|
| Pain medication | NSAIDs for mild pain | NSAIDs for pain, sometimes stronger options needed |
| Hormonal therapy | Birth control pills, IUDs to reduce bleeding | Birth control pills, progestins, GnRH agonists to suppress tissue growth |
| Minimally invasive procedures | Uterine artery embolization, MRI-guided focused ultrasound | Laparoscopic excision or ablation of tissue |
| Surgery | Myomectomy (fibroid removal) or hysterectomy | Laparoscopy to remove tissue, hysterectomy in severe cases |
| Natural approaches | Diet changes, supplements (limited evidence) | Anti-inflammatory diet, physical therapy, acupuncture |
Medication options
For fibroids, hormonal birth control can reduce heavy bleeding but won’t shrink the tumors. GnRH agonists can temporarily shrink fibroids by creating a menopause-like state, but they’re not a long-term solution due to side effects.
For endometriosis, hormonal treatments aim to suppress your menstrual cycle, reducing the hormonal stimulation that makes endometrial tissue grow and bleed. Options include continuous birth control pills, progestin-only pills, hormonal IUDs, and GnRH agonists.
Comparing pain medications: what works best for your condition can help you understand which over-the-counter and prescription options might provide relief while you work on a longer-term treatment plan.
Surgical solutions
For fibroids, a myomectomy removes the tumors while preserving your uterus. This is often the preferred option if you want to maintain fertility. A hysterectomy removes your uterus entirely and is a permanent solution.
For endometriosis, laparoscopic surgery removes or destroys the misplaced tissue. Excision surgery, where tissue is cut out, tends to provide longer-lasting relief than ablation, where tissue is burned away. In severe cases where other treatments have failed, a hysterectomy with removal of the ovaries might be recommended.
“The goal of endometriosis surgery isn’t just to reduce pain temporarily. We’re trying to remove all visible disease and restore normal anatomy so patients can have the best possible quality of life and fertility outcomes.” – Dr. Sarah Chen, Reproductive Endocrinologist
Managing symptoms at home
While medical treatment addresses the underlying condition, symptom management improves daily quality of life.
For fibroid pain, does heat or cold work better for fibroid pain relief can make a real difference during flare-ups. Many women find heating pads helpful for cramps and pressure.
For endometriosis, the 15-minute daily stretching routine for chronic pain management can reduce muscle tension that compounds pelvic pain.
Both conditions benefit from:
- Regular, gentle exercise to reduce inflammation
- Stress management techniques
- Adequate sleep (though how to sleep better when chronic pain keeps you awake might require specific strategies)
- Anti-inflammatory foods like leafy greens, fatty fish, and berries
Can you have both conditions at once?
Yes, and it’s more common than you might think. Studies suggest that 20 to 50 percent of women with endometriosis also have fibroids. Having both conditions can complicate diagnosis because symptoms overlap significantly.
If you have both, your treatment plan needs to address each condition. Your doctor might recommend hormonal therapy to manage endometriosis while monitoring fibroids with regular ultrasounds. In some cases, surgery can address both issues simultaneously.
The fertility factor
Both conditions can affect your ability to get pregnant, but in different ways.
Fibroids might interfere with conception if they:
- Distort the shape of your uterine cavity
- Block fallopian tubes
- Prevent a fertilized egg from implanting
- Increase the risk of miscarriage
Location matters more than size. A small fibroid growing into the uterine cavity causes more fertility problems than a large one on the outer wall of your uterus.
Endometriosis affects fertility through:
- Inflammation that damages eggs or sperm
- Scarring that blocks fallopian tubes
- Adhesions that prevent the ovary from releasing eggs properly
- Changes in the uterine environment that prevent implantation
About 30 to 50 percent of women with endometriosis experience infertility. But many women with endometriosis do conceive, especially with treatment.
If you’re trying to get pregnant and have either condition, working with a reproductive endocrinologist can help you understand your specific situation and options.
When to see a specialist
You should seek medical attention if you experience:
- Pelvic pain that interferes with daily activities or work
- Periods so heavy you’re changing pads or tampons every hour
- Bleeding that lasts longer than seven days
- Severe cramping that doesn’t respond to over-the-counter pain medication
- Pain during sex that’s getting worse
- Difficulty getting pregnant after a year of trying (or six months if you’re over 35)
Your primary care doctor can start the evaluation, but you might need a gynecologist or reproductive endocrinologist for specialized care. If surgery is recommended, when should you consider surgery for chronic pain relief can help you weigh the decision.
Don’t accept “periods are just painful” as an answer. Severe pain isn’t normal, and you deserve proper evaluation and treatment.
Understanding the hormonal connection
Both fibroids and endometriosis are estrogen-dependent conditions. They tend to grow or worsen when estrogen levels are high and often improve during pregnancy or after menopause when estrogen drops.
This hormonal sensitivity explains why:
- Both conditions are most common during reproductive years
- Symptoms often improve during pregnancy
- Hormonal treatments can help manage both conditions
- Both conditions typically improve after menopause
The estrogen-pain connection: how hormones amplify chronic pain in women helps explain why hormonal fluctuations throughout your cycle affect symptom severity.
Understanding this connection can help you track patterns in your symptoms and time treatments for maximum effectiveness.
Living with chronic pelvic pain
Whether you have fibroids, endometriosis, or both, chronic pelvic pain affects every aspect of your life. It impacts your work, relationships, mental health, and daily activities.
The working woman’s guide to managing chronic pain at your desk job offers practical strategies for managing symptoms while maintaining your career.
Building a support system matters. This might include:
- A healthcare team that listens and takes your pain seriously
- Friends or family who understand when you need to cancel plans
- Online or in-person support groups with other women managing similar conditions
- A therapist who specializes in chronic pain
Why does pain become chronic? Understanding your nervous system’s role can help you understand why pelvic pain sometimes persists even after treatment and what you can do about it.
What happens without treatment
Both conditions can worsen over time if left untreated, though the specific risks differ.
Untreated fibroids might:
- Continue growing, causing more severe symptoms
- Lead to anemia from heavy bleeding
- Cause complications during pregnancy
- Rarely, degenerate and cause severe pain
What happens if you leave fibroids untreated? Long-term risks every woman should know provides detailed information about potential complications.
Untreated endometriosis might:
- Progress to more severe stages
- Cause extensive scarring and adhesions
- Lead to chronic pain that’s harder to treat
- Reduce fertility over time
- Affect organs beyond the reproductive system
Early treatment generally leads to better outcomes for both conditions.
Getting clarity on your diagnosis
If you’re still unsure whether your symptoms point to fibroids, endometriosis, or something else entirely, keeping a detailed symptom diary helps. Track:
- When pain occurs (dates, times, relation to your cycle)
- Pain intensity on a scale of 1 to 10
- Pain quality (sharp, dull, cramping, pressure)
- What makes it better or worse
- Bleeding patterns (heaviness, duration, clots)
- Other symptoms like fatigue, digestive issues, or urinary problems
Bring this information to your doctor. Specific details help them determine which tests to order and which treatments might work best.
Some women benefit from seeking a second opinion, especially if initial treatments aren’t helping or if their concerns are being dismissed. Trust your instincts about your body.
Making informed treatment decisions
Once you have a diagnosis, you’ll face decisions about treatment. Consider:
- How much your symptoms affect your quality of life
- Whether you want to preserve fertility
- Your age and how close you are to menopause
- Previous treatments you’ve tried
- Your personal preferences about medication versus surgery
- Potential side effects and risks of each option
How to shrink fibroids naturally: evidence-based strategies that actually work might appeal if you want to try conservative approaches first.
There’s rarely one “right” answer. The best treatment is the one that addresses your specific symptoms, fits your life circumstances, and aligns with your values and goals.
Moving forward with confidence
Understanding the difference between fibroids and endometriosis gives you power. You can ask better questions, recognize when symptoms change, and make informed decisions about your care.
You’re not overreacting to your pain. You’re not being dramatic. These are real medical conditions that deserve proper diagnosis and treatment. The path to relief starts with accurate information and a healthcare provider who takes your concerns seriously. Keep advocating for yourself until you get the answers and treatment you need. Your quality of life matters, and effective options exist for managing both conditions.