Your knee throbs after a run. Your joints ache on cold mornings. That nagging lower back pain flares up without warning. Behind every one of these sensations lies a complex conversation happening inside your body between inflammation and pain.
These two processes aren’t just related. They’re deeply intertwined in ways that determine whether you experience temporary discomfort or months of persistent suffering.
Inflammation triggers pain through chemical messengers called cytokines and prostaglandins that sensitize nerve endings. This protective response becomes problematic when inflammation persists, creating chronic pain cycles. Understanding this biological connection helps explain why anti-inflammatory approaches often reduce pain intensity and why some discomfort lingers long after initial injury healing completes.
What Actually Happens When Inflammation Starts
Inflammation begins the moment your body detects tissue damage or a potential threat.
Your immune system springs into action immediately. White blood cells rush to the affected area. Blood vessels widen to allow more immune cells through. Fluid accumulates in tissues, causing swelling.
This process releases dozens of chemical messengers into your tissues. Each one has a specific job in the healing response.
The main players include:
- Prostaglandins that increase blood flow and make nerve endings more sensitive
- Bradykinin that directly activates pain receptors
- Cytokines like interleukin-1 and tumor necrosis factor that coordinate immune responses
- Histamine that causes blood vessels to leak fluid into tissues
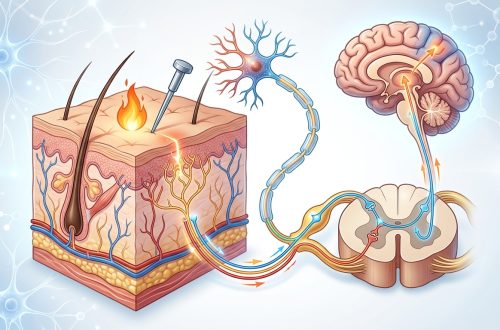
- Substance P that amplifies pain signals traveling to your brain
These chemicals don’t just coordinate healing. They also lower the threshold at which what are pain receptors and how do they actually work fire signals to your nervous system.
The Chemical Messengers Behind Your Discomfort
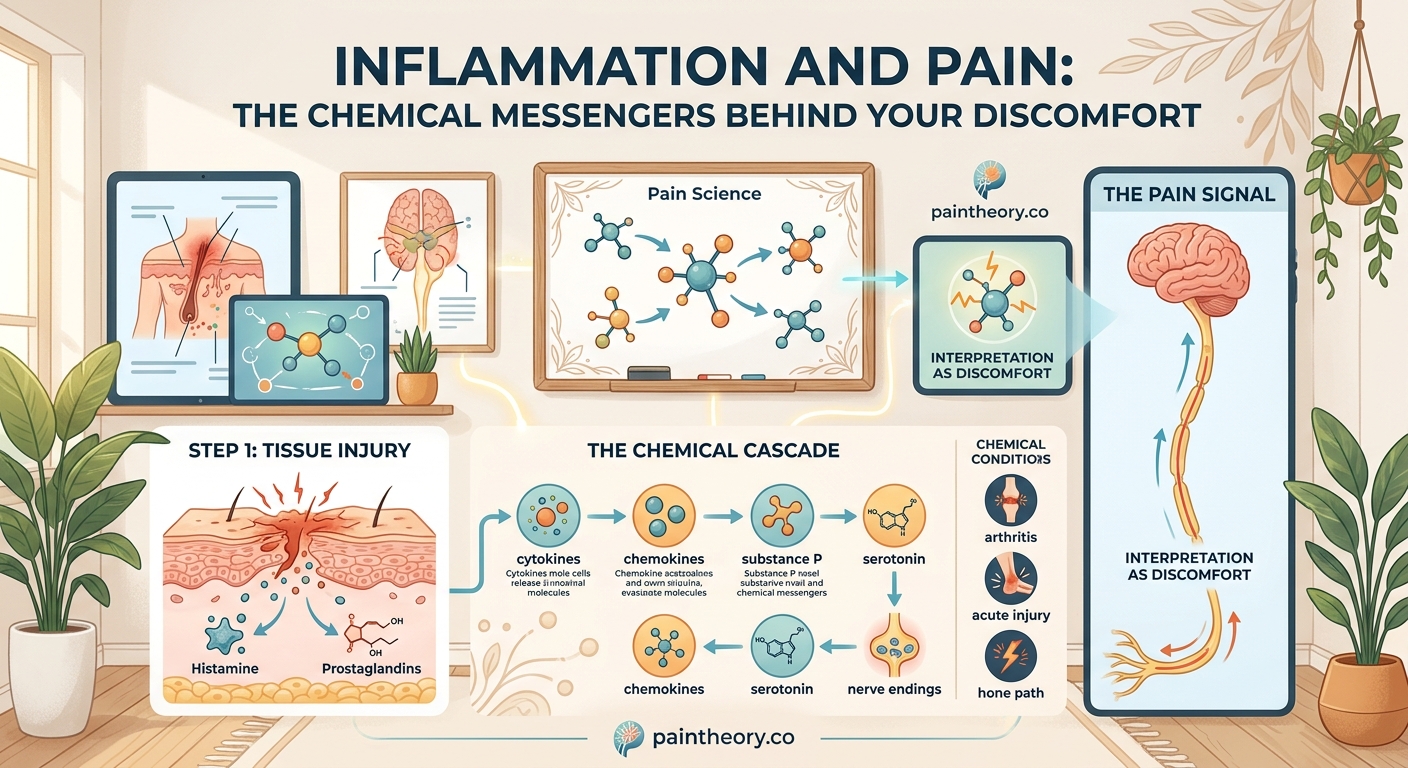
Prostaglandins deserve special attention because they’re central to both inflammation and pain.
Your body produces them at injury sites using an enzyme called cyclooxygenase (COX). Two versions exist: COX-1 and COX-2.
COX-2 enzymes ramp up dramatically during inflammation. They create prostaglandins that make nerve endings hyperresponsive. A stimulus that normally wouldn’t register as painful suddenly feels intense.
This explains why NSAIDs like ibuprofen work. They block COX enzymes, reducing prostaglandin production and thereby decreasing both inflammation and pain sensitivity.
Cytokines work differently but equally powerfully.
These protein molecules act like alarm signals between immune cells. When tissues get damaged, cytokines flood the area to recruit more immune defenders.
But cytokines also directly sensitize pain pathways. They can make neurons fire more readily and amplify signals traveling up your spinal cord to your brain.
“Inflammatory cytokines don’t just cause pain at the injury site. They can sensitize the entire pain processing system, from peripheral nerves all the way up to brain regions that interpret pain intensity and emotional suffering.” — Dr. Linda Watkins, neuroscience researcher
How Acute Inflammation Becomes Chronic Pain
Normal inflammation follows a predictable pattern.
- Injury or infection triggers the inflammatory response
- Chemical messengers flood the area and sensitize nerves
- Immune cells clear damaged tissue and pathogens
- Anti-inflammatory signals shut down the response
- Tissues heal and pain resolves
This process typically completes within days or weeks.
Chronic pain develops when this shutdown fails to happen. Inflammation persists at low levels for months or years. Your nervous system remains in a heightened state of alert.
Several factors can prevent proper resolution:
- Ongoing tissue damage that continuously triggers new inflammatory responses
- Autoimmune conditions where your immune system attacks healthy tissue
- Failed healing processes that leave inflammation smoldering
- Nervous system changes that maintain pain signals even after inflammation decreases
The longer inflammation persists, the more your nervous system adapts. Pain pathways become hypersensitive. Your brain rewires itself to expect and amplify pain signals.
This creates a frustrating cycle where inflammation maintains pain, and chronic pain can actually promote ongoing inflammation. Understanding why does pain become chronic helps break this pattern.
Conditions Where Inflammation Drives Pain
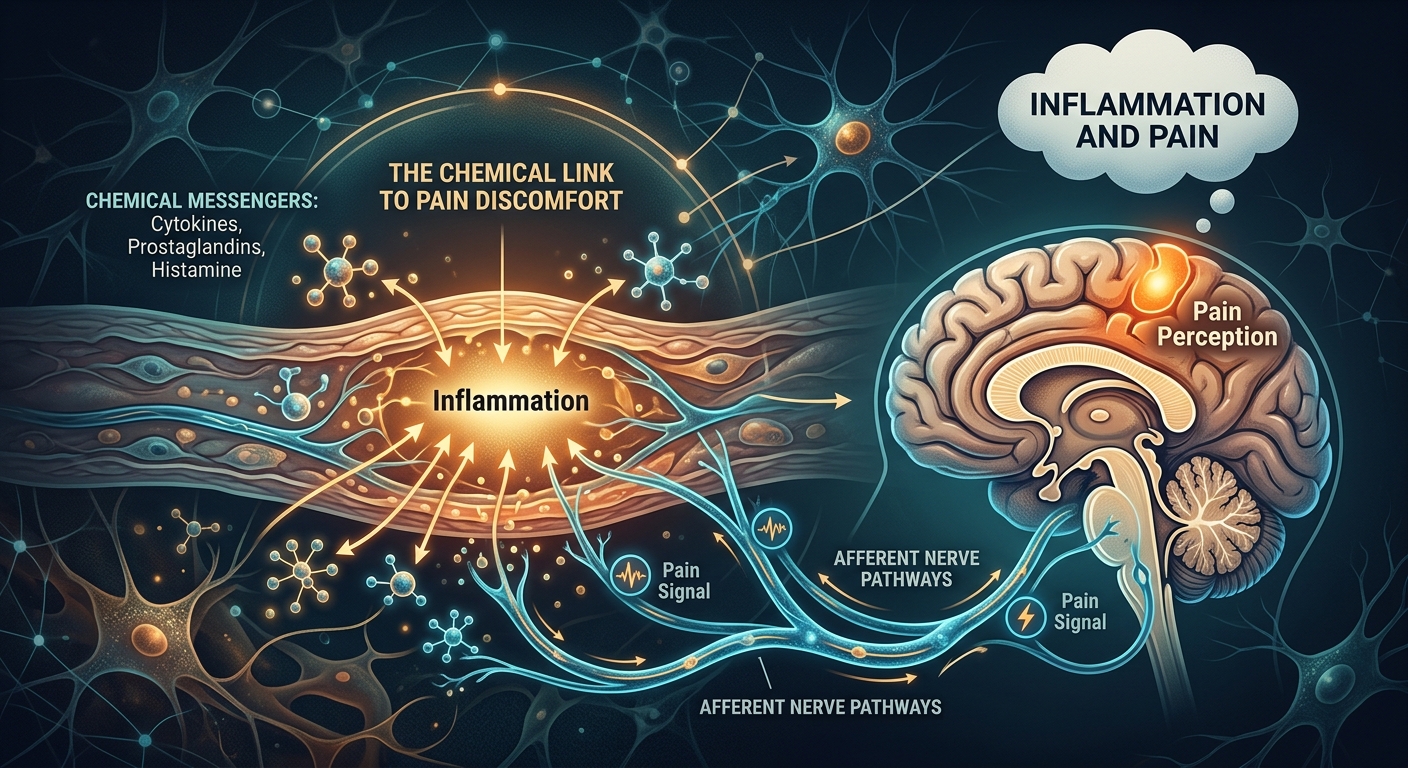
Many chronic pain conditions have inflammation at their core.
Arthritis represents the most obvious example. In osteoarthritis, joint damage triggers inflammatory responses that cause swelling and pain. Rheumatoid arthritis involves immune system attacks on joint tissue, creating persistent inflammation.
Back pain often involves inflammatory processes too. Disc injuries release inflammatory chemicals that irritate nearby nerve roots. This explains why your lower back pain gets worse at night and what to do about it when inflammatory fluid accumulates during rest.
Fibromyalgia presents a more complex picture. Researchers increasingly recognize that low-grade neuroinflammation in the brain and spinal cord contributes to widespread pain sensitivity.
For women, several reproductive conditions involve significant inflammation and pain connections:
Endometriosis creates inflammatory lesions throughout the pelvic cavity. These lesions release cytokines that sensitize pelvic nerves and explain why does endometriosis pain feel worse during your period.
Uterine fibroids can trigger inflammatory responses in surrounding tissues. This contributes to pelvic pain and pressure symptoms.
Even conditions you might not associate with inflammation often involve these processes. Nerve damage from diabetes causes inflammatory changes in nerve tissue. Migraines involve neuroinflammation in brain blood vessels and surrounding tissues.
Measuring Inflammation in Your Body
Doctors use several methods to assess inflammation levels.
Blood tests can measure inflammatory markers:
| Test | What It Measures | Normal Range |
|---|---|---|
| C-reactive protein (CRP) | General inflammation marker | Less than 3.0 mg/L |
| Erythrocyte sedimentation rate (ESR) | How fast red blood cells settle | 0-22 mm/hr for men, 0-29 mm/hr for women |
| Interleukin-6 | Specific inflammatory cytokine | Less than 5 pg/mL |
| Tumor necrosis factor-alpha | Inflammatory signaling protein | Less than 8.1 pg/mL |
These tests help identify systemic inflammation but don’t always correlate perfectly with pain intensity.
You might have elevated inflammatory markers without severe pain. Conversely, you might experience significant pain with normal blood test results.
Local inflammation at specific injury sites doesn’t always show up in blood work. A inflamed knee joint or irritated nerve root might cause substantial pain without raising systemic markers.
Imaging studies like MRI can sometimes visualize inflammatory changes in tissues. These show fluid accumulation, tissue swelling, or inflammatory lesions.
Breaking the Inflammation-Pain Cycle
Addressing inflammation often reduces pain, but the approach matters.
Anti-inflammatory medications work through different mechanisms:
NSAIDs block prostaglandin production and reduce both inflammation and pain sensitivity. They work well for acute injuries and inflammatory conditions like arthritis.
Corticosteroids suppress multiple inflammatory pathways simultaneously. Doctors use them for severe inflammation but limit long-term use due to side effects.
Newer biologics target specific cytokines. These medications help conditions like rheumatoid arthritis where particular inflammatory molecules drive disease.
Lifestyle approaches also powerfully influence inflammation levels.
Diet affects inflammatory processes throughout your body. Foods high in omega-3 fatty acids, antioxidants, and polyphenols can reduce inflammatory marker levels. Processed foods, excess sugar, and certain fats promote inflammation.
Regular movement paradoxically reduces inflammation despite initially triggering mild inflammatory responses. Exercise trains your body to resolve inflammation more efficiently.
Sleep quality directly impacts inflammatory regulation. Poor sleep increases inflammatory cytokine production and lowers pain thresholds. Learning how to sleep better when chronic pain keeps you awake becomes essential.
Stress management matters because psychological stress activates inflammatory pathways. Chronic stress keeps your immune system in overdrive, promoting ongoing inflammation.
Physical therapy and the 15-minute daily stretching routine for chronic pain management can reduce localized inflammation through improved circulation and tissue mobility.
When Inflammation Needs Medical Attention
Not all inflammation-related pain requires aggressive treatment.
Mild inflammatory responses after exercise or minor injuries typically resolve on their own. Rest, ice, and over-the-counter anti-inflammatory medications usually suffice.
Certain warning signs indicate you need professional evaluation:
- Pain that progressively worsens despite home treatment
- Severe swelling, redness, or warmth suggesting infection
- Fever accompanying localized pain and inflammation
- Pain that prevents normal daily activities for more than a few days
- Symptoms suggesting serious underlying conditions
These 5 back pain red flags that mean you should see a doctor immediately apply to inflammatory pain throughout your body.
Healthcare providers can offer targeted treatments that home approaches can’t match.
How nerve blocks and injections target pain at its source by delivering anti-inflammatory medications directly to affected tissues. This provides relief while minimizing systemic side effects.
Physical therapy addresses mechanical factors that perpetuate inflammation. Therapists identify movement patterns or postural issues that continuously irritate tissues.
Comparing pain medications helps you understand which options best match your specific inflammatory condition.
For persistent cases, when should you consider surgery for chronic pain relief becomes relevant if inflammation stems from structural problems that conservative treatment can’t resolve.
Common Mistakes That Worsen Inflammation
People often unknowingly perpetuate inflammatory cycles.
Pushing through pain during flare-ups causes additional tissue damage. This triggers new inflammatory responses on top of existing inflammation.
Inconsistent anti-inflammatory medication use prevents adequate suppression of inflammatory processes. Taking NSAIDs only when pain becomes severe allows inflammation to build between doses.
Ignoring dietary triggers lets food-related inflammation continue unchecked. Some people have sensitivities to specific foods that promote inflammatory responses.
Sedentary behavior during painful episodes seems protective but actually slows inflammation resolution. Complete rest beyond the initial injury phase delays healing.
Inadequate sleep creates a vicious cycle where inflammation disrupts sleep, and poor sleep worsens inflammation.
| Helpful Approach | Common Mistake |
|---|---|
| Consistent low-dose anti-inflammatory use during flares | Taking medication only when pain peaks |
| Gentle movement within pain tolerance | Complete rest for extended periods |
| Anti-inflammatory diet maintained long-term | Dietary changes only during flare-ups |
| Stress reduction practices done regularly | Addressing stress only when overwhelmed |
| Ice for acute inflammation, heat for chronic stiffness | Using heat on acute inflammatory flares |
The Brain’s Role in Processing Inflammatory Pain
Your brain doesn’t passively receive pain signals from inflamed tissues.
It actively interprets, modulates, and sometimes amplifies these signals based on context, past experience, and emotional state.
Inflammatory chemicals sensitize peripheral nerves, but 5 surprising ways your brain creates and amplifies pain sensations show how central processing determines your actual pain experience.
This explains why two people with identical inflammatory conditions report vastly different pain levels.
Psychological factors influence inflammatory processes themselves. Anxiety and depression can increase inflammatory cytokine production. Stress activates inflammatory pathways throughout your body.
The good news is that brain-based interventions can reduce pain even when inflammation persists. Cognitive behavioral therapy, mindfulness practices, and pain neuroscience education all help by changing how your nervous system processes inflammatory signals.
Hormones and Inflammation in Women’s Pain
Women experience unique inflammatory pain patterns related to hormonal fluctuations.
Estrogen influences immune function and inflammatory responses. The estrogen-pain connection explains why many inflammatory pain conditions worsen during certain menstrual cycle phases.
Conditions like endometriosis, fibroids, and ovarian cysts involve complex interactions between hormones and inflammation.
Endometriosis lesions produce inflammatory cytokines that sensitize pelvic nerves. Hormonal changes during menstruation increase inflammatory activity in these lesions.
Fibroids can create localized inflammatory responses in uterine tissue. This contributes to pain beyond simple mechanical pressure effects.
Managing ovarian cyst pain without surgery often involves addressing inflammatory components alongside hormonal factors.
Understanding these connections helps women and their healthcare providers develop more effective treatment strategies.
Living Well Despite Inflammation
Managing chronic inflammatory pain requires a comprehensive approach.
No single intervention addresses all aspects of the inflammation and pain connection. Successful management combines multiple strategies tailored to your specific condition.
Start by identifying and addressing controllable inflammatory triggers. Track your symptoms alongside diet, activity, sleep, and stress to identify patterns.
Work with healthcare providers who understand the complexity of inflammatory pain. Effective treatment often requires coordination between primary care doctors, specialists, physical therapists, and sometimes pain psychologists.
Set realistic expectations. Reducing inflammation and pain to manageable levels represents success for many chronic conditions. Complete elimination isn’t always possible or necessary for good quality of life.
The working woman’s guide to managing chronic pain at your desk job offers practical strategies for maintaining function despite ongoing symptoms.
Remember that inflammation serves protective purposes. The goal isn’t to eliminate all inflammatory responses but to prevent excessive or prolonged inflammation that creates chronic pain.
Your Body’s Healing Conversation
The inflammation and pain connection represents your body’s attempt to protect and heal itself.
Chemical messengers coordinate complex responses designed to clear threats and repair damage. Pain serves as a warning system, encouraging you to rest injured areas while healing occurs.
Problems arise when this normally helpful process becomes excessive or fails to shut down properly. Understanding the biological mechanisms behind your pain empowers you to work with your body’s systems rather than against them.
Small changes in how you eat, move, sleep, and manage stress can significantly influence inflammatory processes. Medical treatments work best when combined with these foundational approaches.
Your pain has biological explanations rooted in measurable chemical and cellular processes. This knowledge transforms pain from a mysterious enemy into an understandable challenge you can address with targeted strategies.