Your lower back has been aching for days now. You’re only 18 weeks along, and you’re wondering if this is just part of pregnancy or something more serious. You’re not alone. Nearly 70% of pregnant women experience back pain at some point during their nine months, but knowing what’s normal and what requires medical attention can feel like guesswork.
Back pain during pregnancy typically results from weight gain, posture changes, and hormone-induced ligament loosening. Most discomfort is normal and manageable with proper positioning, targeted exercises, and supportive devices. However, sudden severe pain, fever, numbness, or pain accompanied by bleeding requires immediate medical evaluation to rule out serious complications like preterm labor or infection.
Why Pregnancy Changes Your Back
Your body undergoes dramatic shifts during pregnancy. Your center of gravity moves forward as your belly grows. Your spine curves more deeply to compensate.
The hormone relaxin loosens your ligaments and joints. This prepares your pelvis for delivery, but it also reduces stability throughout your spine and hips.
Your uterus expands from the size of a pear to a watermelon. This adds 25 to 35 pounds of weight, most of it concentrated in your abdomen.
Your abdominal muscles stretch and sometimes separate. This condition, called diastasis recti, removes crucial support from your lower back.
All these changes create the perfect storm for back discomfort. But not all back pain signals the same problem.
Types of Pregnancy Back Pain
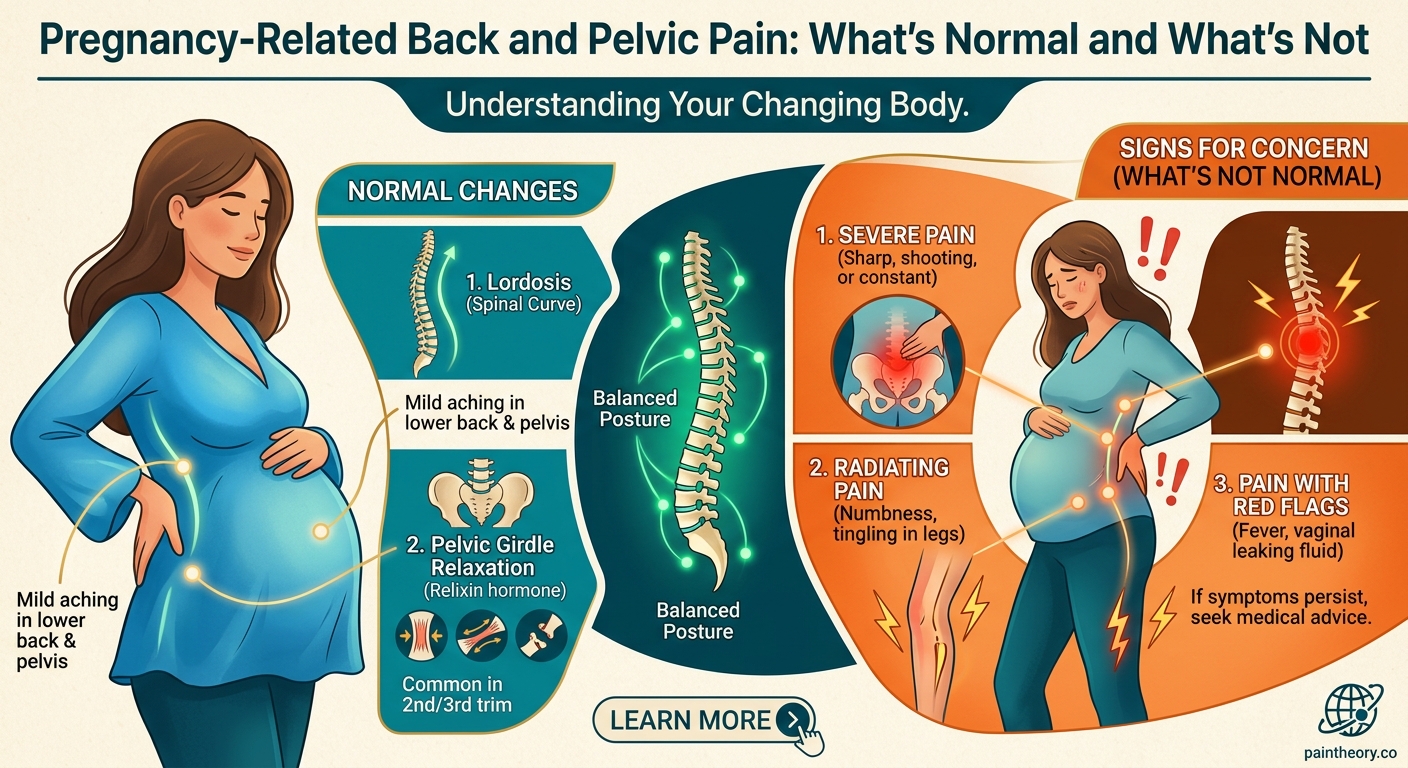
Understanding which type of pain you’re experiencing helps you find the right relief strategy.
Lumbar pain sits in your lower back, around your waistline. It feels similar to the back pain you might have experienced before pregnancy. Standing for long periods makes it worse. It often radiates down into your legs.
Posterior pelvic pain occurs lower than lumbar pain. You’ll feel it deep in your buttocks, sometimes on one or both sides. It can shoot down the back of your thigh. Walking, climbing stairs, or rolling over in bed triggers this pain.
Sacroiliac joint pain appears where your pelvis connects to your spine. It creates a sharp, stabbing sensation on one side of your lower back or buttocks. You might feel it when you stand up from sitting or when you put weight on one leg.
Round ligament pain creates sharp, brief pains on one or both sides of your abdomen or into your groin. It happens when the ligaments supporting your uterus stretch. This pain is sudden but short-lived.
What’s Normal at Each Stage
First Trimester
Back pain in early pregnancy often surprises women. Your belly isn’t showing yet, so why does your back hurt?
Hormonal changes start immediately. Relaxin begins loosening your ligaments within weeks of conception. Your body is preparing for changes that won’t be visible for months.
Breast enlargement adds weight to your upper body. This shifts your posture forward and strains your upper and middle back.
Fatigue makes you more prone to poor posture. You might slouch more when sitting or standing.
Second Trimester
This is when most women start experiencing noticeable back pain. Your belly expands rapidly between weeks 13 and 27.
Your center of gravity shifts forward. You naturally arch your back more to stay balanced. This increased curvature puts pressure on your lower spine.
Your growing uterus stretches your abdominal muscles. The weakened core support means your back muscles work harder to keep you upright.
Weight gain accelerates. Most women gain 1 to 2 pounds per week during this trimester.
Third Trimester
Back pain often intensifies as you approach delivery. The baby drops lower into your pelvis, changing pressure points.
Your relaxin levels peak. Your joints become increasingly unstable. Simple movements that felt fine earlier now cause discomfort.
Sleep becomes difficult. Finding a comfortable position gets harder, and poor sleep makes pain feel worse.
Braxton Hicks contractions can cause back pain. These practice contractions sometimes create a dull ache in your lower back.
Red Flags That Need Medical Attention

Most pregnancy back pain is uncomfortable but harmless. However, certain symptoms require immediate evaluation.
Call your doctor right away if you experience any of these warning signs:
- Severe pain that doesn’t improve with rest or position changes
- Fever above 100.4°F accompanied by back pain
- Numbness or tingling in your legs, feet, or groin
- Difficulty controlling your bladder or bowels
- Vaginal bleeding along with back pain
- Regular, rhythmic back pain before 37 weeks (possible preterm labor)
- Pain following a fall or injury
- Sudden onset of severe pain that takes your breath away
These symptoms might indicate serious conditions like kidney infection, preterm labor, placental abruption, or other complications that require immediate medical care.
“Any back pain accompanied by fever, bleeding, or contractions needs same-day evaluation. Trust your instincts. If something feels wrong, it probably is.” — Dr. Sarah Mitchell, Maternal-Fetal Medicine Specialist
Evidence-Based Relief Strategies
You don’t have to just endure back pain for nine months. These approaches have solid research backing their effectiveness.
Posture and Body Mechanics
How you move and position yourself throughout the day makes a significant difference.
When standing:
– Keep your feet shoulder-width apart
– Slightly bend your knees
– Pull your shoulders back
– Tuck your pelvis under to reduce the arch in your lower back
– Shift your weight between feet if standing for extended periods
When sitting:
– Choose chairs with good lumbar support
– Place a small pillow or rolled towel behind your lower back
– Keep your feet flat on the floor or on a footrest
– Avoid crossing your legs
– Stand and move every 30 minutes
When sleeping:
– Sleep on your left side (best for circulation)
– Place a pillow between your knees
– Put another pillow under your belly for support
– Use a pregnancy pillow that supports your entire body
– Avoid sleeping on your back after 20 weeks
Supportive Devices
The right support can dramatically reduce daily discomfort.
A maternity support belt wraps around your lower back and under your belly. It lifts some of the weight off your spine and pelvis. Wear it during activities that typically cause pain.
Supportive shoes matter more than you think. Avoid heels higher than two inches. Choose shoes with good arch support and cushioning.
A pregnancy pillow transforms sleep quality. Full-body pillows support your back, belly, and legs simultaneously.
Safe Exercises and Stretches
Movement might seem counterintuitive when you’re in pain, but gentle exercise often provides relief.
Pelvic tilts:
1. Get on your hands and knees
2. Keep your back in a neutral position
3. Slowly arch your back like a cat
4. Hold for five seconds
5. Return to neutral
6. Repeat 10 times
Hip flexor stretch:
1. Kneel on your right knee with your left foot flat in front
2. Keep your torso upright
3. Gently push your hips forward
4. Hold for 30 seconds
5. Switch sides
6. Repeat three times per side
Wall squats:
1. Stand with your back against a wall
2. Walk your feet out about two feet
3. Slowly slide down until your thighs are nearly parallel to the floor
4. Hold for 10 seconds
5. Slide back up
6. Repeat 10 times
Swimming and water aerobics provide excellent low-impact exercise. The water supports your weight and takes pressure off your joints and spine.
Walking strengthens your back and core muscles without jarring impact. Start with 10 minutes daily and gradually increase.
Prenatal yoga improves flexibility and teaches breathing techniques useful during labor. Look for certified prenatal instructors who understand pregnancy modifications.
Heat and Cold Therapy
Temperature therapy offers safe, drug-free pain relief.
Apply heat for muscle tension and stiffness. Use a heating pad on low for 15 to 20 minutes. Never fall asleep with a heating pad. Avoid electric blankets on high settings.
Apply cold for acute pain or inflammation. Wrap ice packs in a thin towel. Apply for 10 to 15 minutes at a time.
Alternate heat and cold for stubborn pain. Start with cold for 15 minutes, then switch to heat for 15 minutes.
Warm baths provide overall relaxation. Keep water temperature below 100°F to avoid raising your core temperature.
Professional Treatments
Some situations benefit from expert intervention.
Prenatal massage from a certified therapist trained in pregnancy techniques can relieve muscle tension. Avoid deep tissue massage during pregnancy.
Physical therapy teaches you specific exercises for your pain pattern. A therapist can identify muscle imbalances and create a personalized treatment plan.
Chiropractic care from a practitioner experienced with pregnant patients may help with alignment issues. Make sure they use pregnancy-appropriate techniques and tables.
Acupuncture shows promise for pregnancy-related back pain in several studies. Choose a licensed acupuncturist with prenatal experience.
Common Mistakes That Make Pain Worse
Avoiding these errors can prevent your back pain from escalating.
| Mistake | Why It’s Harmful | Better Alternative |
|---|---|---|
| Wearing high heels | Shifts your center of gravity forward, increasing lower back curve | Supportive flats or shoes with 1-2 inch heels |
| Sleeping on your back after 20 weeks | Reduces blood flow and increases back pressure | Side sleeping with pillow support |
| Lifting heavy objects | Strains already stressed back muscles | Ask for help or use proper lifting technique |
| Staying sedentary | Weakens supporting muscles | Gentle movement and approved exercises |
| Ignoring pain signals | Allows minor issues to become major problems | Rest when needed and modify activities |
| Gaining weight too rapidly | Adds excessive strain to spine | Follow recommended weight gain guidelines |
When Different Specialists Can Help
Your obstetrician should be your first stop for any concerning back pain. They can rule out pregnancy complications and refer you to specialists when needed.
A maternal-fetal medicine specialist handles high-risk pregnancies and complex pain issues. Your OB will refer you if your situation requires this level of care.
A physical therapist designs exercise programs specific to pregnancy. They can address muscle imbalances and teach you proper body mechanics.
An orthopedic specialist evaluates structural problems with your spine or joints. You might need this consultation if you had back problems before pregnancy.
A pain management specialist offers additional options when standard treatments aren’t enough. They understand safe interventions during pregnancy.
Pain Relief Options to Avoid
Pregnancy limits your pain relief choices. Many treatments safe outside pregnancy pose risks to your developing baby.
Avoid these medications unless specifically approved by your doctor:
– Ibuprofen and other NSAIDs after 20 weeks
– Aspirin in regular doses
– Muscle relaxants
– Most prescription pain medications
– Topical pain creams containing NSAIDs
Skip these physical treatments:
– Hot tubs and saunas (risk of overheating)
– Deep tissue massage
– Chiropractic techniques that involve lying on your stomach
– Electrical stimulation devices without medical approval
Planning Ahead for Postpartum
Your back pain might not end with delivery. Planning for the postpartum period helps you recover faster.
Labor and delivery put significant stress on your back and pelvis. You might experience new or worsened pain immediately after birth.
Breastfeeding positions can strain your neck, shoulders, and upper back. Set up proper support before your baby arrives.
Carrying your baby, car seats, and diaper bags adds new physical demands. Your ligaments remain loose for several months postpartum, making you vulnerable to injury.
Sleep deprivation amplifies pain perception. Everything hurts more when you’re exhausted.
Start planning your support system now. Line up help for household tasks, meal preparation, and childcare for older children.
Consider pelvic floor physical therapy postpartum. Many women benefit from professional guidance as their bodies recover.
Your Back Pain Roadmap
Understanding your back pain puts you in control. You know what’s normal, what’s concerning, and what actually helps.
Most pregnancy back pain responds well to simple interventions. Proper posture, supportive devices, gentle exercise, and rest usually provide significant relief.
Trust your body’s signals. If something feels wrong, get it checked. Your instincts about your own body are valuable information.
Remember that this discomfort is temporary. Your body is doing extraordinary work growing a new life. Taking care of your back now helps you stay active and comfortable throughout your pregnancy and sets you up for better recovery after delivery.
Start with one or two strategies that seem most manageable. Maybe that’s adding a pillow between your knees tonight or taking a 10-minute walk tomorrow. Small changes add up to significant relief over time.
Your pregnancy journey is unique. What works for your sister or best friend might not work for you. Be patient as you figure out your own best combination of relief strategies. You’re doing an amazing job, and you deserve to feel as comfortable as possible while you do it.