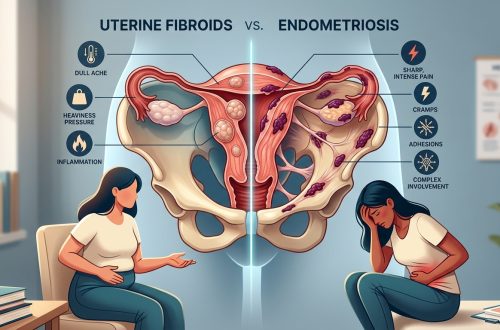
Your doctor just mentioned the word “hysterectomy,” and suddenly your mind is racing. You’re wondering if removing your uterus is really the only option for these painful fibroids, or if there’s another path forward. The decision feels huge because it is. But here’s what matters most: you have more choices than you might think, and understanding them clearly will help you make the right call for your body and your life.
A hysterectomy permanently removes fibroids by removing the uterus, but it’s not the only solution. Less invasive options like myomectomy, [uterine artery embolization](https://www.ncbi.nlm.nih.gov/books/NBK279545/), and medication can effectively manage symptoms for many women. The right choice depends on your symptom severity, fertility goals, fibroid characteristics, and overall health. Understanding all your options helps you make an informed decision that aligns with your life goals.
Understanding what a hysterectomy actually involves
A hysterectomy means surgical removal of your uterus. Sometimes the cervix comes out too (total hysterectomy), and sometimes it stays (partial hysterectomy). Your ovaries may or may not be removed, depending on your situation.
Three main surgical approaches exist:
- Abdominal hysterectomy: The surgeon makes an incision in your lower abdomen. Recovery takes 6 to 8 weeks.
- Vaginal hysterectomy: The uterus is removed through the vagina with no external incisions. Recovery is typically faster.
- Laparoscopic or robotic hysterectomy: Small incisions allow the surgeon to use specialized instruments. Recovery usually takes 2 to 4 weeks.
The approach your doctor recommends depends on your fibroid size, location, and overall pelvic anatomy.
After a hysterectomy, you’ll never have periods again. You cannot get pregnant. If your ovaries remain, you won’t go into surgical menopause. If they’re removed, hormone replacement therapy may become part of your care plan.
When hysterectomy becomes the recommended option
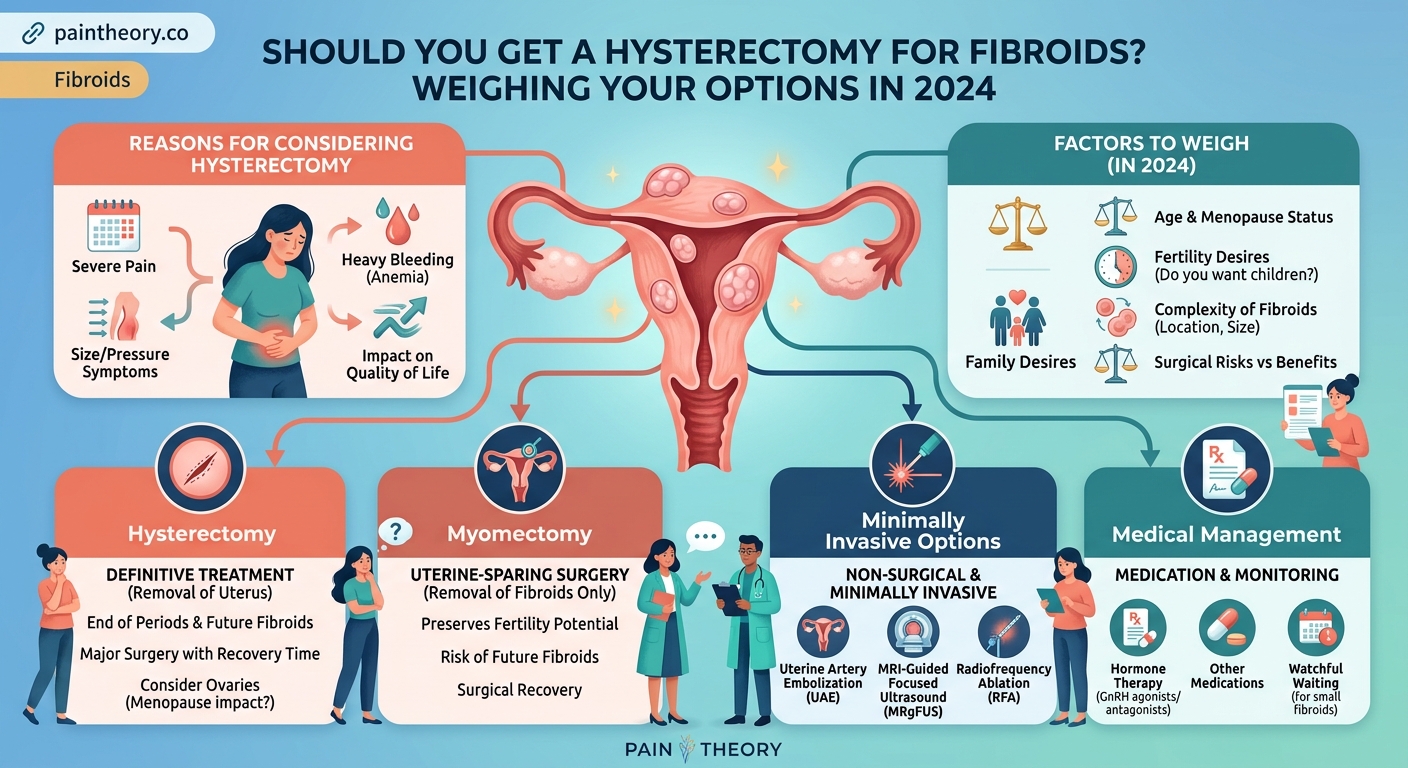
Doctors typically suggest hysterectomy for fibroids when other treatments haven’t worked or when your symptoms severely impact your quality of life.
Common scenarios include:
- Severe, uncontrolled bleeding that causes anemia despite medication or less invasive procedures
- Chronic pelvic pain that doesn’t respond to other treatments
- Large or multiple fibroids that cause pressure on nearby organs like your bladder or bowel
- Completed childbearing with no desire for future pregnancy
- Failed previous fibroid treatments like myomectomy or embolization
Your doctor might also recommend it if imaging shows suspicious features that need definitive diagnosis, though this is less common.
The key factor is whether you want to preserve your uterus for future pregnancy. If you’re done having children and your symptoms are severe, hysterectomy offers a permanent solution.
Comparing hysterectomy to other fibroid treatments
Before committing to uterus removal, understanding your alternatives matters. Here’s how different treatments stack up:
| Treatment | Preserves Uterus | Fibroid Recurrence | Recovery Time | Best For |
|---|---|---|---|---|
| Hysterectomy | No | None (permanent) | 2-8 weeks | Completed childbearing, severe symptoms |
| Myomectomy | Yes | 20-30% within 5 years | 2-6 weeks | Desire future pregnancy |
| Uterine Artery Embolization | Yes | Possible | 1-2 weeks | No future pregnancy desired |
| MRI-guided Focused Ultrasound | Yes | Possible | 1-2 days | Small to medium fibroids |
| Hormonal Medications | Yes | Returns when stopped | N/A | Temporary relief, mild symptoms |
Each option has trade-offs. Myomectomy removes individual fibroids while keeping your uterus intact, making pregnancy possible. However, fibroids can grow back, potentially requiring another surgery down the line.
Uterine artery embolization blocks blood flow to fibroids, causing them to shrink. It’s less invasive than surgery but may affect fertility and doesn’t work for all fibroid types.
Medications like GnRH agonists can shrink fibroids temporarily but cause menopausal symptoms and aren’t long-term solutions. They’re often used to reduce fibroid size before surgery.
Does heat or cold work better for fibroid pain relief while you’re weighing treatment options? Many women find symptom management techniques helpful during the decision-making process.
What to expect during recovery from hysterectomy

Recovery varies based on your surgical approach, but knowing the timeline helps you plan.
First week: You’ll have pain, fatigue, and possibly some vaginal bleeding or discharge. Most women need prescription pain medication. Walking short distances helps prevent blood clots.
Weeks 2-4: Energy gradually returns. You can usually drive once you’ve stopped taking narcotic pain medication and can brake comfortably. Light activities are fine, but no heavy lifting over 10-20 pounds.
Weeks 4-8: For abdominal hysterectomy, this is when you’ll regain most normal activities. Laparoscopic patients often feel better sooner. Sexual activity can typically resume after 6 weeks or when your doctor clears you.
Long-term: Some women report feeling relief almost immediately once fibroid symptoms disappear. Others need time to adjust emotionally to the loss of their uterus.
Complications are uncommon but can include infection, bleeding, injury to nearby organs, or blood clots. Choosing an experienced surgeon reduces these risks significantly.
Making the decision that’s right for your situation
This choice isn’t just medical. It’s personal, emotional, and tied to your vision for your future.
Ask yourself these questions:
- Do I want to have children or more children in the future?
- How severely are my symptoms affecting my daily life, work, and relationships?
- Have I tried other treatments, and did they help?
- Am I comfortable with permanent loss of menstruation and fertility?
- What does my overall health picture look like?
Can fibroids cause weight gain and other symptoms might influence your decision timeline. Some women tolerate mild symptoms for years, while others find even moderate symptoms unbearable.
“The best treatment is the one that aligns with your goals and values. If preserving fertility matters to you, that changes everything. If you’re done with periods and want permanent relief, hysterectomy might be exactly right.” — Dr. Sarah Chen, gynecologic surgeon
Getting a second opinion is always reasonable. Different doctors may have different perspectives based on their training and experience.
Financial and practical considerations you shouldn’t ignore
Surgery costs money, takes time, and requires support during recovery.
Insurance typically covers medically necessary hysterectomy for fibroids, but you’ll want to verify:
- Your deductible and out-of-pocket maximum
- Whether your surgeon is in-network
- Pre-authorization requirements
- Coverage for different surgical approaches
Recovery means time off work. Plan for at least 2 weeks minimum, possibly 6-8 weeks for abdominal surgery. Short-term disability may cover part of your lost wages if you have that benefit.
You’ll need help at home, especially the first week. Someone should drive you home from surgery, and having support for household tasks, childcare, and meal preparation makes recovery much easier.
If chronic pain has been disrupting your sleep, you might find how to sleep better when chronic pain keeps you awake helpful both before and after your procedure.
Emotional and psychological aspects of losing your uterus
Even when hysterectomy is the right medical choice, feelings about it can be complicated.
Some women feel relief. No more heavy periods, no more pain, no more worrying about fibroid growth. The surgery represents freedom from symptoms that have controlled their lives.
Others grieve. Your uterus connects to identity, femininity, and childbearing potential. Losing it can feel like losing part of yourself, even when you’re logically certain it’s the right choice.
Both reactions are completely valid. Many women experience a mix of emotions that shift over time.
Talking with a therapist, joining a support group, or connecting with women who’ve been through the same decision can help. Your partner or close family members might also benefit from understanding what you’re experiencing.
Research shows that most women report improved quality of life after hysterectomy for fibroids, particularly when symptoms were severe. Regret is uncommon when the decision was well-informed and aligned with personal values.
Alternatives worth trying before making a final decision
If you’re not facing an emergency situation, trying conservative approaches first makes sense.
Hormonal birth control pills or IUDs can reduce bleeding and pain for some women. They won’t shrink fibroids significantly but may make symptoms manageable.
GnRH agonists create a temporary menopause state that shrinks fibroids. Side effects include hot flashes and bone density loss, so they’re used short-term, often before surgery to make the procedure easier.
Tranexamic acid is a non-hormonal medication that reduces heavy menstrual bleeding by about 40%. It doesn’t affect fibroids themselves but can improve your quality of life.
For women who want to keep their uterus but don’t plan future pregnancies, endometrial ablation destroys the uterine lining to reduce bleeding. It doesn’t remove fibroids but can help with symptom management.
Understanding when should you consider surgery for chronic pain relief applies here too. Surgery becomes appropriate when conservative treatments fail and symptoms significantly impair your life.
Questions to ask your doctor before scheduling surgery
Come to your appointment prepared. These questions will help you gather the information you need:
- Based on my specific fibroids, what are all my treatment options?
- Why do you recommend hysterectomy over other approaches?
- Which surgical approach would you use for me, and why?
- What are your complication rates for this procedure?
- How many of these surgeries do you perform each year?
- Will my ovaries be removed, and what are the reasons for that decision?
- What will my recovery realistically look like?
- What symptoms should prompt me to call you after surgery?
- Are there any medical reasons I should have surgery sooner rather than later?
- What happens if I choose to wait?
Don’t leave the office until you understand the answers. If something isn’t clear, ask again. This is your body and your choice.
If your fibroids are causing lower back pain that gets worse at night, mention this specifically. It might influence the urgency of treatment.
Living well after hysterectomy
Life after surgery can be remarkably good, especially when fibroid symptoms were severely impacting your daily activities.
Most women report:
- Complete elimination of heavy menstrual bleeding
- Significant reduction or complete resolution of pelvic pain
- Improved energy levels once anemia resolves
- Better sleep without pain interruptions
- More freedom to participate in activities without worrying about bleeding
Physical activity can gradually resume. Start with walking and light movement, then progress to more intense exercise as your body heals. Your core muscles will need time to recover strength, especially after abdominal surgery.
Sexual function typically returns to normal or improves once pain resolves. Some women worry that removing the uterus will change sensation or desire, but research shows most women experience no negative impact on sexual satisfaction.
Hormone levels remain stable if your ovaries weren’t removed. You won’t experience menopause until your natural time. If your ovaries were removed, hormone replacement therapy can manage menopausal symptoms effectively.
Regular follow-up care continues even after hysterectomy. You’ll still need routine gynecologic exams, pelvic exams, and if your cervix remains, Pap smears.
Finding confidence in your choice
You’re facing a significant decision, and feeling uncertain is natural. The fact that you’re researching thoroughly shows you’re taking this seriously and advocating for yourself.
Trust that you know your body better than anyone else. You understand how much your symptoms affect your daily life, your relationships, and your happiness. Medical advice provides crucial information, but you’re the expert on what you can and cannot live with.
Whether you choose hysterectomy or another path, make your decision based on complete information, alignment with your values, and confidence in your medical team. There’s no universal right answer, only the right answer for you at this point in your life.
Give yourself permission to take the time you need to decide, unless your doctor indicates urgency for medical reasons. This choice will affect you for years to come, and making it thoughtfully matters more than making it hastily.