If you’ve noticed your pain flares up before your period, during pregnancy, or as you approach menopause, you’re not imagining things. Estrogen plays a powerful role in how your body experiences and processes pain. For millions of women living with chronic conditions, understanding this hormonal connection can be the missing piece in finally getting relief.
Estrogen directly influences pain sensitivity through its effects on nerve cells, inflammation, and neurotransmitters. Women experience more chronic pain conditions than men, partly due to hormonal fluctuations throughout menstrual cycles, pregnancy, and menopause. Understanding how estrogen amplifies pain helps you work with healthcare providers to develop targeted treatment strategies that address both hormonal imbalances and pain management simultaneously for better long-term relief.
What Makes Estrogen So Influential in Pain Processing
Estrogen doesn’t just regulate your reproductive system. It acts on pain receptors throughout your entire body.
Your nervous system has estrogen receptors in key areas that control pain signals. When estrogen levels change, these receptors respond differently to pain stimuli. High estrogen can sometimes reduce pain sensitivity, while low estrogen often increases it.
But the relationship isn’t that simple.
Estrogen also affects inflammation markers in your body. When levels drop suddenly, inflammatory compounds can surge. This is why many women notice joint pain, headaches, or body aches right before their period starts.
The hormone influences serotonin and endorphins too. These are your body’s natural pain relievers. When estrogen dips, so do these protective chemicals. You’re left more vulnerable to pain signals that your brain would normally dampen.
How Hormonal Fluctuations Trigger Pain Cycles
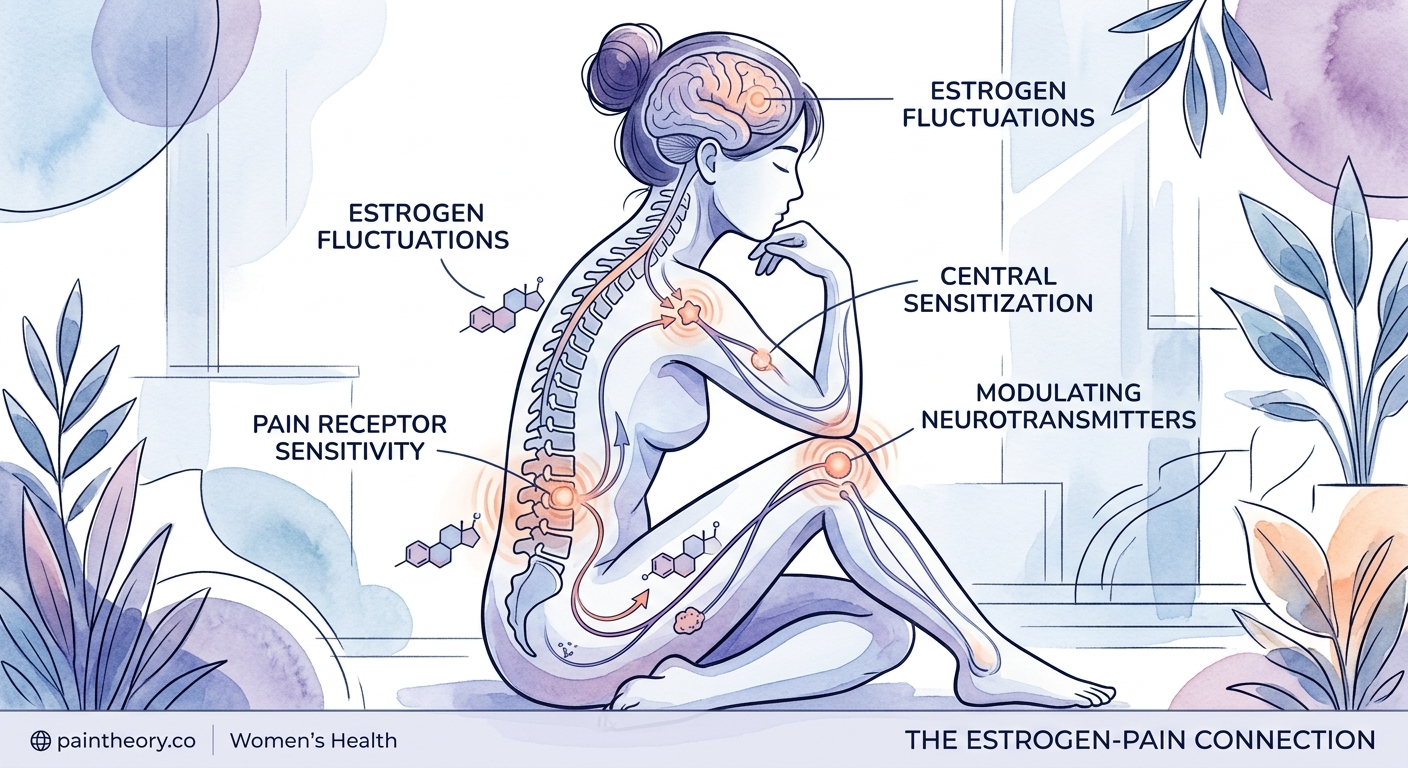
Your menstrual cycle creates a monthly roller coaster of hormone levels. Each phase brings different pain risks.
During the follicular phase (right after your period), estrogen rises steadily. Many women feel their best during this time. Pain conditions often improve.
Ovulation brings peak estrogen levels. Some women experience mittelschmerz, or ovulation pain, but chronic conditions may temporarily ease.
The luteal phase is where things get complicated. Estrogen drops, then rises slightly, then crashes right before menstruation. Progesterone also enters the picture. This hormonal chaos can trigger migraines, fibromyalgia flares, and arthritis pain.
Menstruation itself brings the lowest estrogen levels of your cycle. Pain sensitivity peaks. Conditions like endometriosis feel significantly worse during your period because of this hormonal low point combined with inflammatory prostaglandins.
Chronic Pain Conditions Most Affected by Estrogen
Migraines and Hormonal Headaches
Women experience migraines three times more often than men. The estrogen connection is undeniable.
Menstrual migraines typically strike in the two days before your period through the third day of bleeding. This timing matches the sharp estrogen drop perfectly.
Pregnancy often brings migraine relief during the second and third trimesters when estrogen stays consistently high. But postpartum, when estrogen plummets, migraines often return with a vengeance.
Perimenopause can be brutal for migraine sufferers. Erratic estrogen swings create unpredictable attack patterns.
Fibromyalgia
About 80 to 90 percent of fibromyalgia patients are women. Estrogen’s role in this widespread pain condition is significant.
Research shows that estrogen modulates pain pathways in the central nervous system. When levels are low or fluctuating wildly, the pain amplification characteristic of fibromyalgia intensifies.
Many women report that fibromyalgia symptoms worsen premenstrually and during perimenopause. Sleep disruption from hormonal changes compounds the problem, since poor sleep makes chronic pain worse.
Rheumatoid Arthritis and Joint Pain
Autoimmune arthritis affects women at much higher rates than men. Estrogen influences immune system function, which explains part of this disparity.
During pregnancy, when estrogen levels soar, many women with rheumatoid arthritis experience remission. Symptoms often return postpartum as hormones normalize.
Menopause frequently brings new onset or worsening arthritis. The permanent estrogen decline removes some protective effects on joints and increases inflammatory responses.
Temporomandibular Joint Disorder (TMJ)
Women aged 20 to 40 experience TMJ pain far more often than men. Estrogen receptors exist in the jaw joint itself.
Hormonal fluctuations affect the joint’s cartilage and the muscles surrounding it. Pain often worsens premenstrually and during times of hormonal transition.
The Perimenopause and Menopause Pain Connection
Perimenopause typically starts in your 40s, though it can begin earlier. This transition period brings the most erratic hormone fluctuations of your life.
Estrogen doesn’t just decline gradually. It swings wildly from very high to very low, sometimes within the same week. These unpredictable changes wreak havoc on pain conditions.
Women who never had chronic pain may suddenly develop it during perimenopause. Those with existing conditions often see dramatic worsening.
Common new pain complaints during this time include:
- Joint and muscle aches
- Headaches or new onset migraines
- Widespread body pain
- Lower back pain that intensifies at night
- Burning mouth syndrome
- Increased sensitivity to touch
After menopause, when estrogen settles at consistently low levels, some women find their pain stabilizes. Others continue struggling with conditions that developed during the transition.
How to Track Your Hormonal Pain Patterns
Understanding your personal pattern is the first step toward better management.
-
Start a detailed symptom diary. Record pain levels daily using a 0 to 10 scale. Note the type of pain, location, and intensity.
-
Track your menstrual cycle carefully. Mark the first day of your period and count cycle days. Note any spotting or irregular bleeding.
-
Document other symptoms. Include mood changes, sleep quality, energy levels, and digestive issues. These often correlate with hormonal shifts.
-
Continue for at least three months. Patterns become clear when you can compare multiple cycles side by side.
-
Bring your tracking data to appointments. This concrete information helps healthcare providers see connections you might miss and make better treatment recommendations.
Treatment Approaches That Address the Hormonal Component
Hormone Therapy Options
For some women, stabilizing estrogen levels reduces pain significantly.
Birth control pills provide steady hormone levels without the monthly crash. Continuous dosing (skipping placebo weeks) can prevent menstrual migraine triggers entirely.
Hormone replacement therapy during perimenopause and menopause may ease pain conditions for some women. However, HRT carries risks that you need to discuss thoroughly with your doctor.
Topical estrogen creams offer localized treatment with less systemic absorption. Some women find these helpful for joint pain or vulvodynia.
Medications That Work With Your Cycle
Timing medication to your hormonal fluctuations can improve effectiveness.
Preventive migraine medication taken only during the luteal phase may be sufficient for menstrual migraine sufferers. This reduces overall medication exposure.
Anti-inflammatory drugs started a few days before your period can prevent prostaglandin surges that worsen pain.
Some doctors recommend adjusting chronic pain medication doses based on cycle phase, increasing during high-risk times.
Lifestyle Modifications That Support Hormone Balance
What you do daily affects how your body handles hormonal fluctuations.
Regular exercise helps regulate hormones and reduces inflammation. Aim for 30 minutes of moderate activity most days. Even walking counts.
Sleep consistency matters tremendously. Irregular sleep disrupts hormone production and amplifies pain sensitivity. Stick to the same sleep and wake times, even on weekends.
Stress management directly impacts cortisol, which interacts with estrogen. High cortisol can worsen hormonal imbalances. Try meditation, yoga, or deep breathing exercises.
Nutrition choices influence inflammation and hormone metabolism. Focus on:
- Omega-3 fatty acids from fish or flaxseed
- Plenty of vegetables, especially cruciferous types
- Adequate protein at each meal
- Limited processed foods and added sugars
- Moderate caffeine and alcohol
Understanding When Pain Becomes Chronic
Hormonal fluctuations can trigger acute pain episodes. But why does pain sometimes become chronic and persistent?
Your nervous system can become sensitized over time. Repeated pain signals create changes in how your brain and spinal cord process information. This is called central sensitization and plays a major role in chronic pain.
Estrogen fluctuations can accelerate this sensitization process. Each hormonal pain flare reinforces the pain pathways in your nervous system.
Breaking this cycle requires addressing both the hormonal triggers and the nervous system changes. This is why comprehensive treatment works better than targeting just one aspect.
Common Mistakes Women Make Managing Hormonal Pain
| Mistake | Why It Backfires | Better Approach |
|---|---|---|
| Dismissing pain as “just hormones” | Delays proper diagnosis and treatment | Track patterns but seek medical evaluation |
| Taking pain medication only when severe | Allows inflammation to build up | Use preventive strategies during high-risk cycle phases |
| Stopping treatment when pain improves | Doesn’t address underlying hormonal dysfunction | Continue treatment through full cycles to assess effectiveness |
| Ignoring other health conditions | Conditions like fibroids or thyroid problems worsen hormonal pain | Get comprehensive evaluation for overlapping issues |
| Relying solely on medication | Misses opportunities for lifestyle improvements | Combine medication with exercise, sleep, and stress management |
What Your Doctor Should Evaluate
A thorough assessment of hormonal pain includes several components.
Your healthcare provider should take a detailed menstrual history. When did your periods start? Are they regular? How long do they last? How heavy is your flow?
Hormone testing can be helpful but timing matters. A single test rarely tells the whole story. Testing at different cycle phases or repeatedly over time gives better information.
Screening for conditions that affect both hormones and pain is important. Thyroid disorders, polycystic ovary syndrome, and uterine fibroids can all complicate the picture.
Your doctor should also assess for vitamin deficiencies. Low vitamin D, magnesium, and B vitamins can worsen both hormonal imbalances and pain sensitivity.
When to Consider Specialized Treatment
Some situations call for more intensive intervention.
If pain significantly interferes with work, relationships, or daily activities despite conservative treatment, specialized pain management may help. This might include nerve blocks, physical therapy, or surgical options in select cases.
If hormonal treatments aren’t working or cause unacceptable side effects, a reproductive endocrinologist can offer more sophisticated hormone management.
If you suspect multiple overlapping conditions, a multidisciplinary pain clinic provides coordinated care from various specialists.
“Women’s pain has been understudied and undertreated for too long. Understanding the estrogen connection validates what many women have known instinctively: their pain is real, it’s connected to their hormones, and it deserves comprehensive treatment.” – Dr. Andrea Bradford, Pain Psychology Researcher
Practical Pain Management Strategies for Different Life Stages
Reproductive Years (20s to 40s)
Focus on tracking and prevention. Your cycles are likely regular, making patterns easier to identify.
Consider hormonal birth control if you’re not trying to conceive. The steady hormone levels can dramatically reduce pain flares.
Build strong lifestyle habits now. Regular exercise, good sleep, and stress management create resilience against hormonal fluctuations.
Perimenopause (40s to early 50s)
This is often the most challenging time. Expect unpredictability.
Stay flexible with your treatment plan. What works one month may not work the next as hormone levels swing wildly.
Communicate frequently with your healthcare provider. Don’t wait for annual appointments if symptoms change significantly.
Consider short-term hormone therapy if pain becomes unmanageable. Even a year or two of treatment during the worst transition period can provide relief.
Postmenopause (after final period)
Pain may stabilize once hormones settle at consistently low levels. Some women feel better than they have in years.
Others need ongoing management as low estrogen continues affecting pain sensitivity.
Hormone replacement therapy remains an option if benefits outweigh risks for your individual situation.
Focus on maintaining bone health and muscle strength, as both affect pain levels long-term.
The Mind-Body Connection in Hormonal Pain
Chronic pain affects your emotional health. Hormonal fluctuations affect your mood. The combination can feel overwhelming.
Anxiety and depression are more common in women with chronic pain conditions. Estrogen influences neurotransmitters that regulate mood, so hormonal changes can worsen mental health symptoms.
This isn’t weakness. It’s biology.
Addressing the psychological aspects of pain improves outcomes. Cognitive behavioral therapy helps you develop coping strategies. Mindfulness practices reduce pain catastrophizing. Support groups provide validation and practical advice from others who understand.
Taking care of your mental health is part of treating hormonal pain, not separate from it.
Your Path Forward with Hormonal Pain
You now understand that estrogen and chronic pain in women are deeply connected. Your pain isn’t all in your head. It’s in your hormones, your nervous system, and your body’s complex response to both.
Start with tracking. Knowledge about your personal patterns empowers better conversations with healthcare providers. Bring data, not just descriptions.
Build your treatment team. You may need a primary care doctor, gynecologist, pain specialist, and mental health provider all working together. Coordinated care produces the best results.
Be patient with the process. Finding the right combination of treatments takes time. Hormonal pain management is rarely a single solution. It’s usually several strategies working together.
And remember that your pain is valid. It deserves attention, treatment, and respect. Keep advocating for yourself until you find providers who take your symptoms seriously and work with you toward relief.