If you’ve been told that painful periods are just something you need to push through, you’re not alone. Many women spend years believing their severe menstrual pain is normal, only to later discover they have endometriosis. But here’s what makes this condition particularly confusing: the pain doesn’t stay constant. It spikes dramatically during your period, leaving you wondering why those few days each month feel so unbearable.
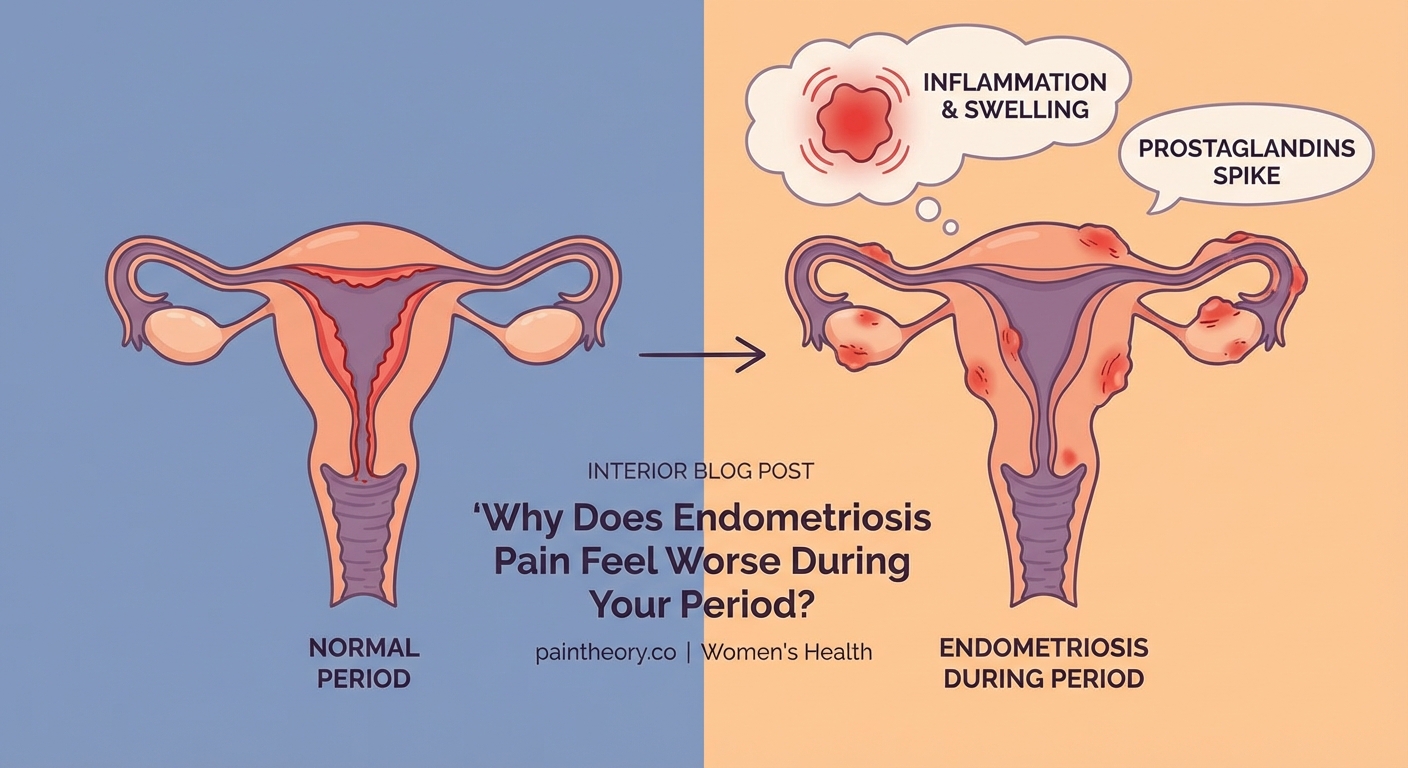
Endometriosis pain worsens during menstruation because hormonal changes trigger inflammation in misplaced [endometrial tissue](https://www.nichd.nih.gov/health/topics/endometri) throughout your body. As estrogen and progesterone levels fluctuate, this tissue swells, bleeds, and irritates surrounding organs. Unlike normal menstrual tissue that exits your body, endometriosis lesions have nowhere to go, creating pressure, inflammation, and severe pain that intensifies with each menstrual cycle.
Understanding What Endometriosis Actually Does
Endometriosis occurs when tissue similar to your uterine lining grows outside the uterus. This tissue can appear on your ovaries, fallopian tubes, bladder, intestines, and even as far as your diaphragm or lungs in rare cases.
Here’s the problem: this tissue behaves just like the lining inside your uterus. It responds to the same hormonal signals that control your menstrual cycle.
During a normal period, your uterine lining sheds and exits through your vagina. But endometriosis tissue has no exit route. When it tries to shed, it becomes trapped inside your body.
Think of it like a wound that reopens every month but never gets the chance to properly heal. Each cycle creates more irritation, more scar tissue, and more pain.
The Hormonal Trigger Behind Period Pain
Your menstrual cycle runs on hormones, primarily estrogen and progesterone. These chemical messengers rise and fall in predictable patterns throughout the month.
Estrogen builds up during the first half of your cycle, thickening the uterine lining in preparation for a potential pregnancy. Progesterone takes over after ovulation, maintaining that lining.
When pregnancy doesn’t occur, both hormones drop sharply. This sudden decline triggers menstruation.
For women with endometriosis, these hormonal shifts affect not just the uterus but every patch of endometrial tissue scattered throughout the body. As estrogen drops, all of that tissue tries to shed simultaneously.
The result? Inflammation erupts in multiple locations at once.
Why Inflammation Makes Everything Hurt More
When endometriosis tissue breaks down during your period, your immune system responds as it would to any internal injury. It sends inflammatory chemicals to the affected areas.
This inflammation causes:
- Swelling that puts pressure on nearby organs
- Release of pain-causing chemicals called prostaglandins
- Irritation of nerve endings in affected tissues
- Formation of adhesions that bind organs together
- Bleeding that has nowhere to drain
Prostaglandins deserve special attention. These compounds make your uterus contract during menstruation, but they also amplify pain signals throughout your nervous system. Women with endometriosis produce higher levels of prostaglandins than average, creating a feedback loop of increasing discomfort.
The Trapped Blood Problem
Normal menstrual blood flows out of your body. Endometriosis blood gets trapped.
When endometrial tissue on your ovaries bleeds, it forms cysts called endometriomas or “chocolate cysts” because of their dark, thick appearance. These cysts can grow to several centimeters and cause intense pain as they expand during each period.
Lesions on your bladder or intestines can bleed internally, causing inflammation that makes urination or bowel movements excruciating during menstruation.
The trapped blood irritates surrounding tissue, triggering your immune system to attack. White blood cells flood the area, causing even more swelling and pain.
Over time, your body tries to wall off these problem areas with scar tissue. But scar tissue is rigid and inflexible, creating new sources of pain as organs get pulled out of their normal positions.
How Your Body’s Pain Response Amplifies Symptoms
Chronic pain changes how your nervous system processes signals. This phenomenon, called central sensitization, means your brain becomes hypersensitive to pain.
After months or years of repeated inflammation, your nervous system starts interpreting normal sensations as painful ones. A gentle touch on your abdomen might feel like pressure. Mild bloating might register as severe cramping.
During your period, when actual tissue damage occurs, this heightened sensitivity makes everything feel exponentially worse.
Your body also develops “pain memory.” Areas that have been repeatedly injured become more reactive to future inflammation. This explains why endometriosis pain often gets progressively worse with each passing year if left untreated.
Recognizing When Period Pain Crosses the Line
Many women dismiss severe menstrual pain as normal because they’ve experienced it since their first period. But there’s a difference between typical menstrual cramps and endometriosis pain.
Normal period cramps:
- Respond well to over-the-counter pain medication
- Last one to three days
- Feel like a dull ache or pressure in your lower abdomen
- Don’t prevent you from attending work or school
- Improve with heat, rest, or light movement
Endometriosis pain:
- Requires prescription medication or doesn’t respond to medication at all
- Can start before your period and last throughout
- Feels sharp, stabbing, or burning
- Forces you to miss work, cancel plans, or stay in bed
- May worsen with movement or certain positions
If you regularly miss work or school because of period pain, that’s not normal. If you’ve been to the emergency room for menstrual cramps, that’s a red flag.
The Domino Effect on Other Body Systems
Endometriosis doesn’t just cause pelvic pain. Because lesions can grow anywhere, your symptoms during menstruation might include:
- Painful bowel movements or diarrhea if lesions affect your intestines
- Painful urination or blood in urine if lesions involve your bladder
- Shoulder pain if lesions grow on your diaphragm
- Leg pain if lesions compress nerves in your pelvis
- Nausea and vomiting from severe pain or intestinal involvement
- Fatigue from chronic inflammation and poor sleep
These symptoms cluster around your period because that’s when all the endometrial tissue throughout your body becomes most active.
A Timeline of What Happens During Your Cycle
Understanding the progression helps explain why certain days feel worse than others.
| Cycle Phase | Hormone Levels | What Happens to Endometriosis | Typical Pain Level |
|---|---|---|---|
| Days 1-5 (Menstruation) | Estrogen and progesterone drop | Tissue breaks down and bleeds | Severe to extreme |
| Days 6-14 (Follicular) | Estrogen rises | Tissue begins to rebuild | Mild to moderate |
| Day 14 (Ovulation) | Estrogen peaks, progesterone starts rising | Tissue continues thickening | Moderate (ovulation pain possible) |
| Days 15-28 (Luteal) | Progesterone dominates | Tissue becomes engorged with blood | Moderate, increasing toward period |
Many women report that pain starts two to three days before bleeding begins. This happens because inflammatory chemicals start releasing as hormone levels begin their pre-menstrual drop.
Why Some Months Feel Worse Than Others
If you’ve noticed that some periods are more painful than others, you’re not imagining it. Several factors influence pain severity:
-
Stress levels: Cortisol, your stress hormone, can amplify inflammation and lower your pain threshold.
-
Diet changes: Foods high in inflammatory compounds (processed foods, alcohol, red meat) can worsen symptoms.
-
Sleep quality: Poor sleep increases inflammatory markers and reduces your ability to cope with pain.
-
Physical activity: Both too much and too little exercise can affect symptoms differently.
-
Lesion growth: Endometriosis progresses over time, meaning more tissue equals more potential pain.
-
Adhesion formation: As scar tissue develops, it can create new sources of pain independent of your cycle.
The Role of Estrogen Dominance
Some women with endometriosis produce higher than normal estrogen levels or process estrogen inefficiently. This condition, called estrogen dominance, feeds endometriosis growth.
Estrogen tells endometrial tissue to grow and thicken. More estrogen means more tissue proliferation, which translates to more inflammation and pain during menstruation.
Factors that contribute to estrogen dominance include:
- Excess body fat (fat cells produce estrogen)
- Exposure to endocrine-disrupting chemicals in plastics and personal care products
- Liver dysfunction that impairs estrogen metabolism
- Low fiber intake (fiber helps eliminate excess estrogen)
- Chronic stress (affects hormone balance)
This creates a vicious cycle: estrogen feeds endometriosis, endometriosis causes inflammation, inflammation disrupts hormone balance, hormone imbalance produces more estrogen.
What Medical Research Tells Us
“Endometriosis is not just a gynecological condition. It’s a systemic inflammatory disease that affects multiple body systems. The cyclical nature of symptoms corresponds directly to hormonal fluctuations, but the underlying inflammation persists throughout the entire month, even when pain temporarily subsides.” (Dr. Iris Orbuch, endometriosis specialist)
Recent studies have revealed that women with endometriosis have different immune system profiles compared to women without the condition. Their bodies produce higher levels of inflammatory cytokines, particularly during menstruation.
Research also shows that endometriosis lesions contain their own nerve fibers. These nerves grow deeper into tissue with each menstrual cycle, explaining why pain often worsens over time even if lesion size stays the same.
Scientists have discovered that endometriosis tissue produces its own estrogen locally, independent of ovarian estrogen production. This means lesions can continue growing and causing problems even when overall estrogen levels are controlled.
Breaking the Pain Cycle
Understanding why your pain worsens during your period is the first step toward managing it effectively. Here are evidence-based approaches that target the root mechanisms:
-
Hormonal suppression: Birth control pills, hormonal IUDs, or medications that stop ovulation can prevent the monthly hormonal fluctuations that trigger symptoms.
-
Anti-inflammatory strategies: NSAIDs taken preventively (starting before your period begins) can reduce prostaglandin production and limit inflammation.
-
Dietary modifications: An anti-inflammatory diet rich in omega-3 fatty acids, vegetables, and whole grains may reduce overall inflammation levels.
-
Pelvic floor physical therapy: Chronic pain often causes pelvic floor muscle dysfunction, which creates additional pain during menstruation.
-
Surgical excision: Removing endometriosis lesions can significantly reduce pain, though symptoms may return if new lesions develop.
-
Stress management: Techniques like meditation, yoga, or counseling can modulate your nervous system’s pain response.
When to Seek Specialized Care
If over-the-counter pain medication doesn’t control your symptoms, or if you’re missing work or school regularly because of period pain, it’s time to see a specialist.
Look for a gynecologist who specializes in endometriosis, not just a general practitioner. Endometriosis requires specific expertise to diagnose and treat effectively.
Red flags that warrant immediate medical attention:
- Pain so severe you can’t stand up straight
- Fever along with pelvic pain
- Sudden, sharp pain that doesn’t ease (could indicate a ruptured cyst)
- Heavy bleeding that soaks through a pad or tampon every hour
- Difficulty breathing or chest pain during your period
Don’t let anyone tell you that debilitating period pain is normal or that you just need to tolerate it. Severe menstrual pain is always worth investigating.
Your Pain Has a Reason
Endometriosis pain worsens during your period because your body is literally fighting itself. Tissue that should only exist inside your uterus is scattered throughout your abdomen, responding to hormonal signals, breaking down, bleeding, and triggering inflammation with nowhere for that inflammation to go.
This isn’t in your head. It’s not something you need to just push through. Your pain is a signal that something specific is happening in your body, something that can be identified, understood, and treated. Armed with this knowledge, you can have more productive conversations with your healthcare providers and make informed decisions about your treatment options. You deserve to have periods that don’t control your life.