Your back has been aching for months. You’ve tried stretches, heat pads, and over-the-counter pain relievers. But what if the missing piece of your recovery plan is sitting on your dinner plate?
Inflammation is a major driver of chronic back pain. When your body stays in an inflamed state, it keeps pain signals firing even after an injury should have healed. The good news is that certain foods can either fuel that inflammation or help calm it down.
An anti-inflammatory diet for back pain focuses on whole foods rich in [omega-3 fatty acids](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3257651/), antioxidants, and fiber while eliminating processed foods, refined sugars, and trans fats. Research shows that dietary changes can reduce inflammatory markers in the body within weeks, potentially decreasing pain intensity and improving mobility for people with chronic back conditions.
Understanding the Inflammation and Back Pain Connection
Inflammation is your body’s natural response to injury or stress. When you hurt your back, inflammatory chemicals rush to the area to start healing.
That’s helpful in the short term.
But chronic inflammation is different. It keeps your pain receptors sensitized long after the initial injury. This creates a cycle where inflammation triggers pain, and pain triggers more inflammation.
Diet plays a bigger role in this cycle than most people realize. Certain foods contain compounds that either promote or reduce inflammatory markers in your bloodstream. These markers include cytokines, prostaglandins, and C-reactive protein.
Studies on people with chronic pain conditions show that those who eat more anti-inflammatory foods report lower pain levels over time. The effect isn’t instant like taking a pill, but it builds as your body’s chemistry shifts.
Why does pain become chronic in the first place? Your nervous system can get stuck in a heightened state of alert, and inflammation is one of the triggers that keeps it there.
Foods That Fight Inflammation and Support Back Health

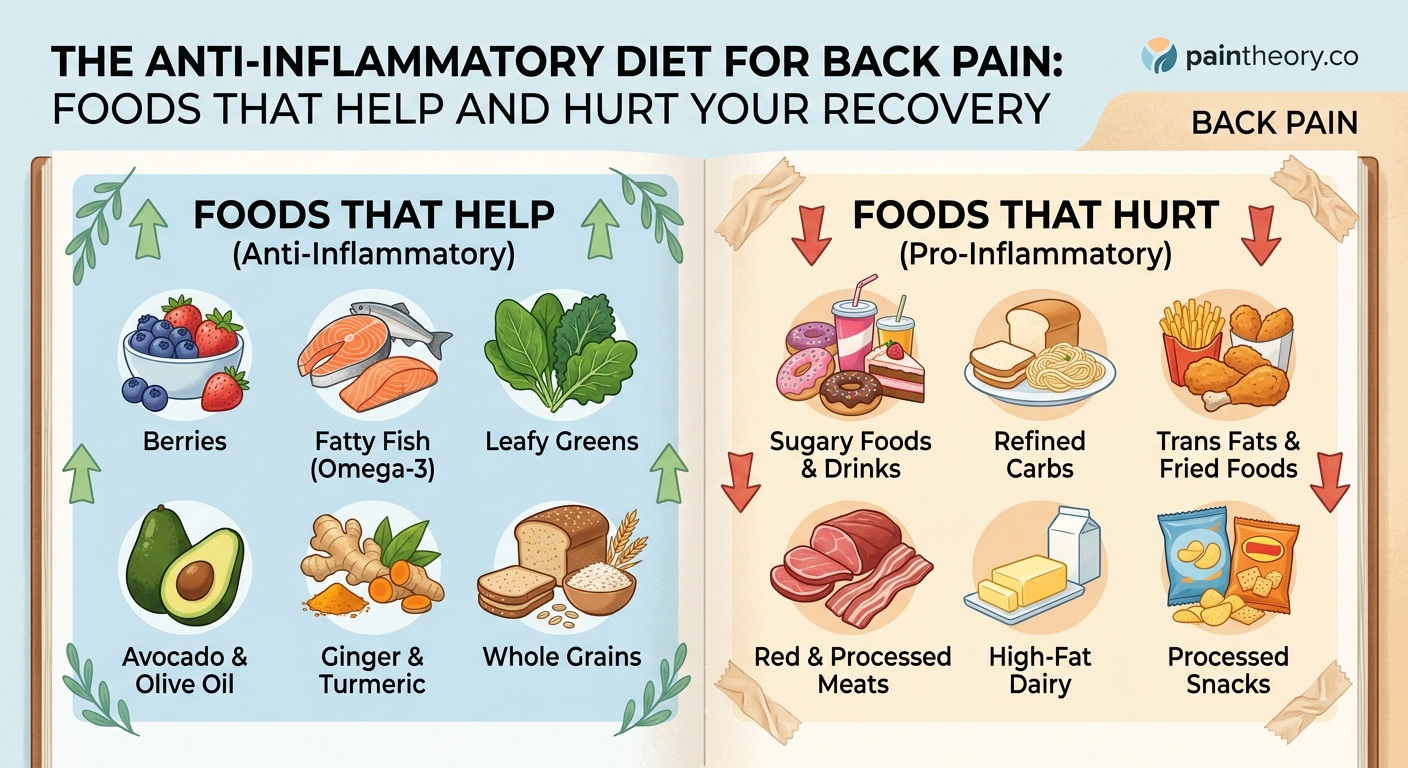
The most powerful anti-inflammatory foods share common traits. They’re typically whole, unprocessed, and packed with nutrients that calm your immune system.
Fatty fish tops the list. Salmon, mackerel, sardines, and herring contain omega-3 fatty acids called EPA and DHA. These compounds directly reduce the production of inflammatory chemicals. Aim for at least two servings per week.
Leafy greens like spinach, kale, and collard greens deliver antioxidants and vitamin K. Vitamin K helps regulate inflammatory responses in your body. Try adding a handful to smoothies or sautéing them with garlic.
Berries are inflammation-fighting superstars. Blueberries, strawberries, and blackberries contain anthocyanins, which are compounds that reduce oxidative stress. Frozen berries work just as well as fresh ones.
Nuts and seeds provide healthy fats, fiber, and minerals. Walnuts are especially high in omega-3s. Almonds offer vitamin E, another anti-inflammatory nutrient. A small handful makes a perfect snack.
Olive oil contains oleocanthal, a compound that works similarly to ibuprofen in reducing inflammation. Use extra virgin olive oil for salads and low-heat cooking.
Here are more foods to include regularly:
- Turmeric (contains curcumin, a potent anti-inflammatory)
- Ginger (reduces prostaglandins that cause pain)
- Green tea (rich in polyphenols)
- Tomatoes (high in lycopene)
- Cherries (especially tart cherries for pain relief)
- Broccoli and other cruciferous vegetables
- Avocados (healthy fats and antioxidants)
- Dark chocolate (70% cacao or higher)
Foods That Worsen Inflammation and Back Pain
Just as important as knowing what to eat is understanding what to avoid. Some foods actively promote inflammation in your body.
Refined carbohydrates spike your blood sugar and trigger inflammatory responses. White bread, pastries, and most breakfast cereals fall into this category. They also lack the fiber that helps control inflammation.
Sugar is one of the worst offenders. It increases inflammatory markers and can worsen pain sensitivity. This includes sodas, candy, and many packaged foods with hidden sugars.
Trans fats are found in many fried foods, margarine, and processed baked goods. They raise inflammatory markers and lower the anti-inflammatory compounds in your blood.
Processed meats like hot dogs, sausages, and deli meats contain advanced glycation end products (AGEs) that promote inflammation. They’re also high in saturated fats that can worsen pain conditions.
Vegetable oils high in omega-6 fatty acids can throw off your body’s inflammatory balance. Corn oil, soybean oil, and sunflower oil are common culprits when consumed in excess.
Alcohol in large amounts increases inflammation and can interfere with sleep, which is crucial for managing chronic pain. If you drink, keep it moderate.
The table below shows common food swaps that can reduce inflammation:
| Instead of This | Choose This | Why It Helps |
|---|---|---|
| White bread | Whole grain or sourdough | Lower glycemic impact, more fiber |
| Vegetable oil | Olive oil or avocado oil | Better omega-3 to omega-6 ratio |
| Sugary cereal | Oatmeal with berries | Stable blood sugar, antioxidants |
| Processed lunch meat | Grilled chicken or chickpeas | Less AGEs, more protein |
| Soda | Green tea or water with lemon | Antioxidants instead of sugar |
| Chips | Nuts or carrot sticks | Healthy fats and nutrients |
Building Your Anti-Inflammatory Meal Plan

Creating sustainable eating habits matters more than perfect meals. Start with small changes that fit your lifestyle.
Follow these steps to build your plan:
-
Assess your current diet. Keep a food journal for three days. Notice how many inflammatory foods you’re eating versus anti-inflammatory ones.
-
Make one swap per week. Don’t overhaul everything at once. Replace your morning bagel with oatmeal topped with walnuts and berries. Next week, swap your afternoon chips for a handful of almonds.
-
Plan your protein sources. Include fatty fish twice a week. On other days, choose chicken, turkey, legumes, or tofu. Avoid processed meats.
-
Fill half your plate with vegetables. This simple rule ensures you get plenty of anti-inflammatory compounds. Mix colors for different nutrients.
-
Prep ingredients on weekends. Wash greens, chop vegetables, and cook grains in advance. This makes healthy choices easier during busy weekdays.
-
Stay hydrated. Water helps flush inflammatory compounds from your body. Aim for eight glasses daily, more if you’re active.
A sample day might look like this:
- Breakfast: Greek yogurt with blueberries, walnuts, and a drizzle of honey
- Lunch: Large salad with mixed greens, grilled salmon, cherry tomatoes, cucumber, and olive oil dressing
- Snack: Apple slices with almond butter
- Dinner: Baked chicken breast with roasted broccoli and quinoa
- Evening: Turmeric tea or tart cherry juice
The Role of Supplements in an Anti-Inflammatory Approach
Whole foods should be your foundation, but some supplements can support your efforts when diet alone isn’t enough.
Omega-3 supplements can help if you don’t eat fish regularly. Look for high-quality fish oil or algae-based options with at least 1000mg of combined EPA and DHA. Take them with meals to improve absorption.
Turmeric or curcumin supplements provide higher doses than you’d get from cooking. Pair them with black pepper, which increases absorption by up to 2000%. Standard doses range from 500 to 2000mg daily.
Vitamin D deficiency is common in people with chronic pain. Low levels are associated with increased inflammation. Have your doctor check your levels before supplementing.
Magnesium helps with muscle relaxation and pain management. Many people don’t get enough from food alone. Magnesium glycinate is well-absorbed and less likely to cause digestive issues.
“Food can be the most powerful form of medicine or the slowest form of poison. When patients combine an anti-inflammatory diet with other pain management strategies, we often see improvements that medications alone couldn’t achieve.” – Dr. Sarah Mitchell, Pain Management Specialist
Always talk to your healthcare provider before starting new supplements, especially if you take medications. Some supplements can interact with blood thinners, diabetes medications, and other drugs.
Common Mistakes When Starting an Anti-Inflammatory Diet
Even with good intentions, people often stumble in predictable ways. Avoid these pitfalls to stay on track.
Going too extreme too fast. Cutting out every “bad” food overnight usually backfires. You’ll feel deprived and likely give up within weeks. Gradual changes stick better.
Focusing only on what to avoid. If you only think about restrictions, you’ll feel miserable. Instead, get excited about new foods to try. Experiment with recipes that feature anti-inflammatory ingredients.
Ignoring portion sizes. Even healthy foods can cause problems in excess. Nuts are nutritious but calorie-dense. Olive oil is beneficial but still adds up. Pay attention to serving sizes.
Expecting instant results. This isn’t a pain pill. Dietary changes typically take several weeks to show effects on inflammation markers. Some people notice improvements sooner, but give it at least a month.
Not addressing other lifestyle factors. Diet alone won’t fix chronic back pain if you’re not sleeping, barely moving, or living with constant stress. Sleep quality affects inflammation levels significantly.
Falling for “superfoods” marketing. No single food will cure your pain. A varied diet rich in many anti-inflammatory foods works better than loading up on one trendy ingredient.
Forgetting to stay consistent. Eating well for a few days then returning to old habits won’t produce lasting changes. Think of this as a permanent shift, not a temporary diet.
Combining Diet with Other Back Pain Strategies
Food is powerful, but it works best as part of a comprehensive approach to managing back pain.
Movement matters. Gentle stretching helps maintain flexibility and reduces stiffness. It also improves circulation, which helps deliver anti-inflammatory nutrients to your tissues.
Stress management is crucial. Chronic stress elevates cortisol, which promotes inflammation throughout your body. Meditation, deep breathing, or even short walks can help lower stress hormones.
Sleep quality directly impacts inflammation. When you don’t sleep well, inflammatory markers rise. Create a consistent bedtime routine and make your bedroom conducive to rest.
Body mechanics at work make a difference. If you sit at a desk all day, proper posture and regular breaks prevent additional strain on your back.
Know when to seek help. If your back pain is severe, getting worse, or accompanied by other symptoms, don’t rely on diet alone. Certain warning signs require immediate medical attention.
Some people benefit from working with healthcare providers who understand both nutrition and pain management. They can help you create a personalized plan that addresses your specific situation.
Tracking Your Progress and Adjusting Your Approach
Measuring your results helps you stay motivated and identify what works for your body.
Keep a pain and food journal. Rate your pain level each day on a scale of 1 to 10. Note what you ate and any other relevant factors like sleep quality or stress levels. After a few weeks, patterns often emerge.
Track your mobility. Can you bend further than before? Do you move more easily in the morning? These functional improvements matter as much as pain scores.
Monitor inflammation markers if possible. Some people work with their doctors to check C-reactive protein or other inflammatory markers through blood tests. This provides objective data on how your diet is affecting inflammation.
Pay attention to other health changes. Many people notice better energy, improved digestion, or clearer thinking when they reduce inflammatory foods. These are positive signs that your body is responding.
Be patient but persistent. If you don’t see improvements after six to eight weeks of consistent effort, consider whether you need to adjust your approach. Maybe you’re still eating hidden sources of inflammation, or perhaps you need to address other factors contributing to your pain.
Making It Sustainable for the Long Term
The anti-inflammatory diet for back pain isn’t a temporary fix. It’s a way of eating that supports your overall health for years to come.
Find versions of your favorite foods that fit the plan. Love pizza? Make it with whole grain crust, lots of vegetables, and moderate cheese. Craving something sweet? Dark chocolate, fruit, or yogurt with honey can satisfy without spiking inflammation.
Build a support system. Tell family and friends about your goals. When they understand why you’re making changes, they’re more likely to support you. Some people find success joining online communities focused on anti-inflammatory eating.
Plan for special occasions. You don’t need to be perfect at every meal. If you eat well most of the time, occasional treats won’t derail your progress. Enjoy birthday cake or holiday meals without guilt, then return to your regular eating pattern.
Keep learning. Nutrition science evolves, and you’ll discover new foods and recipes that work for you. Stay curious about how different foods affect your body.
Celebrate small wins. Did you go a week without soda? Make that. Notice less stiffness in the morning? That’s progress. Acknowledging improvements keeps you motivated.
Your Plate, Your Power
Food choices might seem small in the moment, but they add up to significant changes in how your body handles inflammation and pain. Every meal is an opportunity to support your recovery or work against it.
The anti-inflammatory diet for back pain isn’t about perfection or deprivation. It’s about gradually shifting toward foods that help your body heal while reducing those that keep inflammation high. Start with one change this week. Add another next week. Before long, these choices become habits that serve your health for life.
Your back pain didn’t develop overnight, and it won’t disappear that way either. But with consistent effort, the right foods can become powerful allies in your journey toward less pain and better movement.