You’ve been told PCOS is just about irregular periods and ovarian cysts. But the aching joints, the persistent headaches, the lower back pain that won’t quit? Those aren’t in your head. They’re real, measurable consequences of a condition that affects your entire body, not just your reproductive system.
PCOS pain manifests throughout your body due to chronic inflammation, [insulin resistance](https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5866679/), and hormonal imbalances. Women with PCOS experience higher rates of joint pain, headaches, muscle aches, and nerve discomfort compared to those without the condition. Understanding these connections helps you advocate for proper treatment and find targeted relief strategies that address the root causes, not just symptoms.
What Makes PCOS Pain Different From Regular Discomfort
PCOS doesn’t follow the rules of typical reproductive conditions. While you might expect pelvic pain or cramping, the reality is far more complex.
The condition creates a perfect storm of inflammation throughout your body. Your cells become resistant to insulin, forcing your pancreas to pump out more of the hormone. This excess insulin triggers your ovaries to produce more androgens (male hormones), which throws your entire endocrine system off balance.
That imbalance doesn’t stay contained in your pelvis. It radiates outward, affecting tissues, joints, nerves, and muscles from your head to your feet.
Studies show women with PCOS report pain in locations that seem completely unrelated to their ovaries. The connection isn’t obvious until you understand how systemic inflammation works.
Where PCOS Pain Shows Up in Your Body
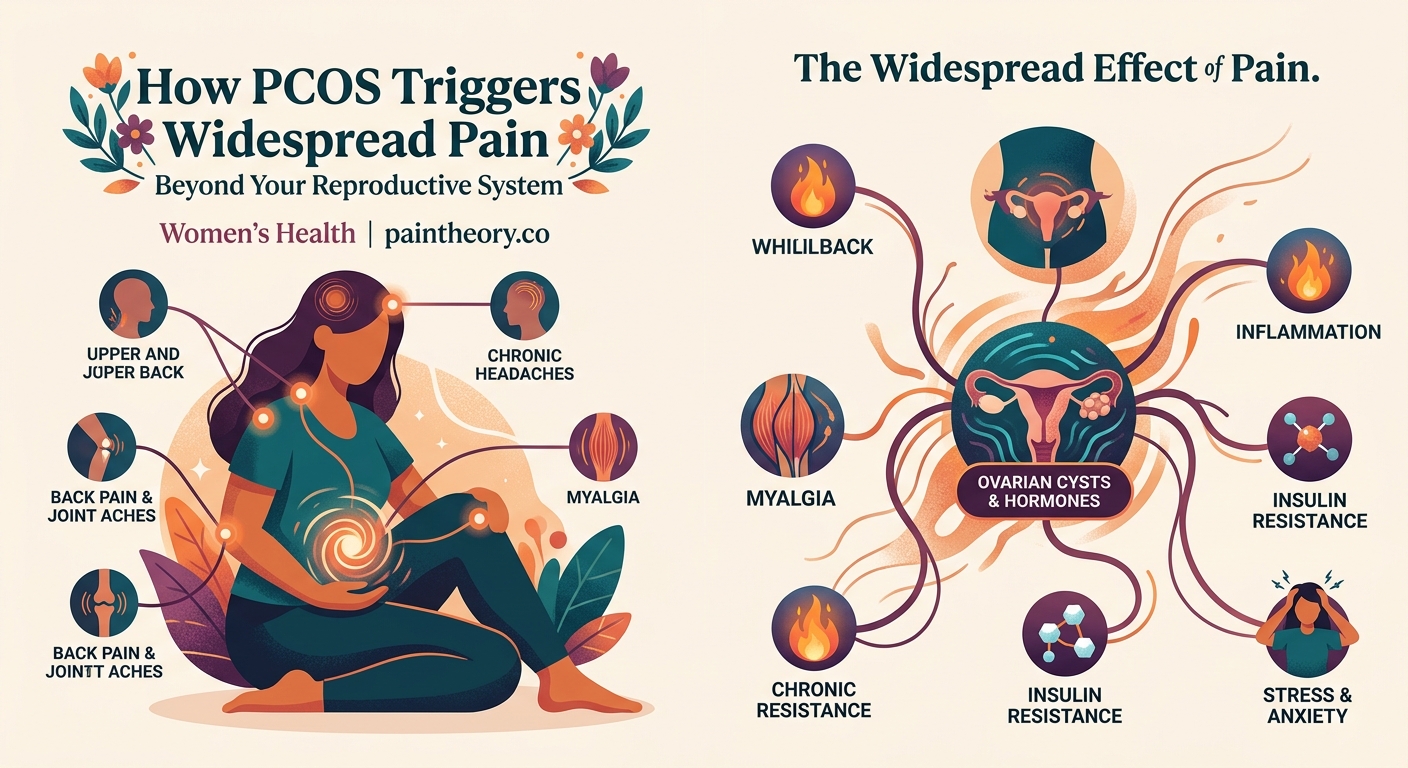
The pain locations might surprise you. Here’s where women with PCOS most commonly experience discomfort:
- Lower back and hip pain that worsens during menstruation
- Joint stiffness and achiness, particularly in hands and knees
- Tension headaches and migraines that coincide with hormonal fluctuations
- Muscle soreness without clear cause or recent exercise
- Nerve pain or tingling in extremities
- Abdominal bloating and digestive discomfort beyond typical cramping
- Chest wall pain that mimics cardiac issues but stems from inflammation
Each of these pain types connects back to the core metabolic and hormonal disruptions PCOS creates.
The Inflammation Connection You Need to Understand
Chronic low-grade inflammation is the thread connecting PCOS to widespread pain. Your body exists in a constant state of mild immune activation.
Think of inflammation as your immune system’s alarm bell. In acute situations, like a sprained ankle, inflammation helps healing. But with PCOS, that alarm never fully shuts off.
Researchers measure inflammation using markers like C-reactive protein (CRP). Women with PCOS consistently show elevated CRP levels compared to women without the condition. This persistent inflammation sensitizes pain receptors throughout your body, making you more susceptible to discomfort in multiple locations.
The inflammation and pain relationship in PCOS creates a feedback loop. Insulin resistance promotes inflammation. Inflammation worsens insulin resistance. The cycle continues, amplifying pain signals along the way.
How Insulin Resistance Amplifies Your Pain Sensitivity
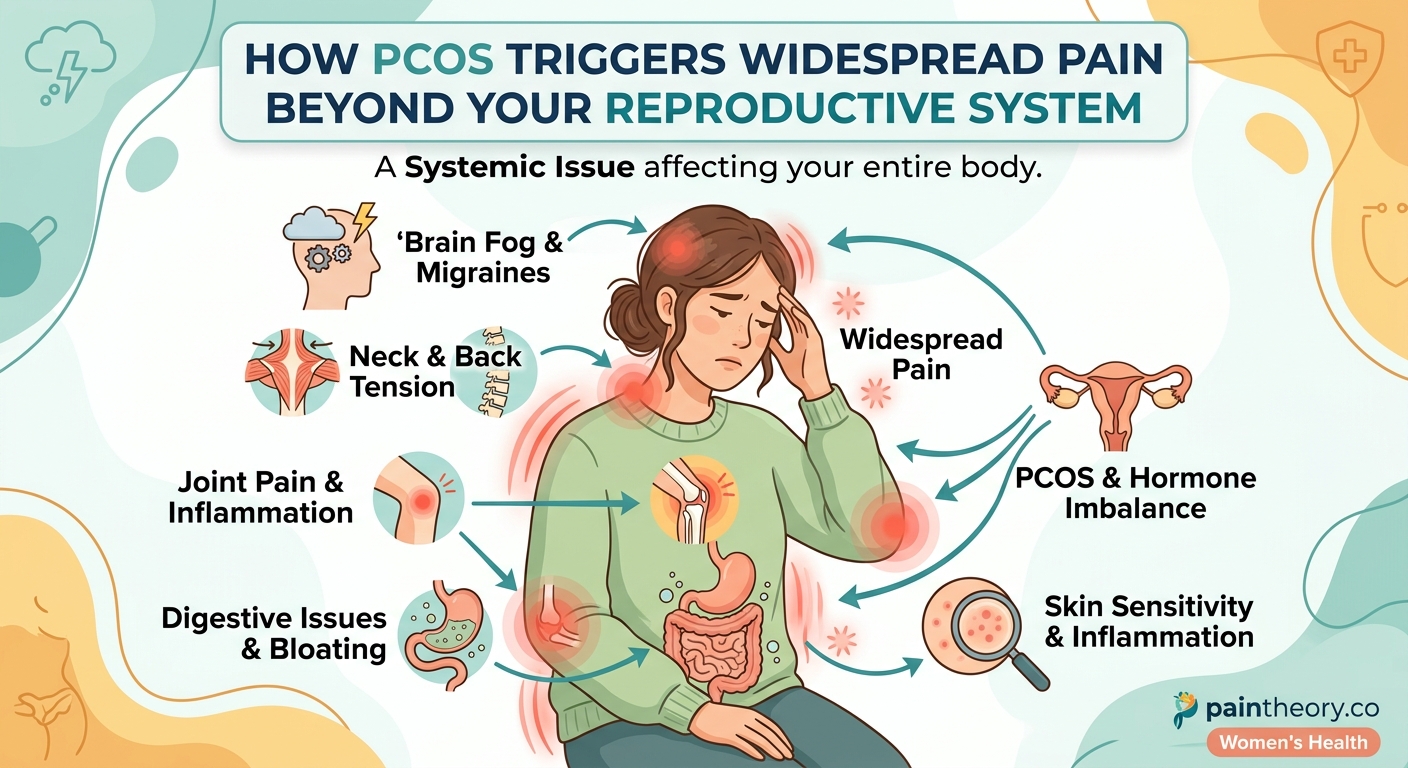
Insulin resistance does more than affect your blood sugar. It fundamentally changes how your nervous system processes pain signals.
When your cells resist insulin’s effects, glucose builds up in your bloodstream. This excess sugar damages small blood vessels and nerves through a process called glycation. Damaged nerves send faulty pain signals, creating discomfort even when no actual tissue injury exists.
Your pain threshold drops. Sensations that wouldn’t normally register as painful suddenly feel intense and overwhelming.
This explains why some women with PCOS develop conditions like fibromyalgia or chronic fatigue syndrome. The underlying metabolic dysfunction makes their nervous systems hyperreactive to stimuli.
Hormonal Fluctuations and Pain Intensity Patterns
The estrogen-pain connection plays a major role in how PCOS pain fluctuates throughout your cycle, assuming you have somewhat regular cycles.
Estrogen and progesterone don’t just control reproduction. They modulate pain perception in your brain and spinal cord. When these hormones swing wildly or remain chronically imbalanced, your pain experience changes accordingly.
Many women with PCOS notice their pain worsens during specific times:
- The week before an expected period (if cycles occur)
- During ovulation attempts, when follicles develop but don’t release eggs
- After consuming high-sugar or high-carbohydrate meals that spike insulin
These patterns aren’t coincidental. They reflect the direct influence hormones have on your pain processing systems.
Common PCOS Pain Conditions and Their Triggers
| Pain Condition | Primary Trigger | How PCOS Contributes |
|---|---|---|
| Migraine headaches | Estrogen fluctuations | Irregular cycles create unpredictable hormone swings |
| Joint pain | Systemic inflammation | Elevated inflammatory markers damage cartilage |
| Muscle aches | Insulin resistance | Poor glucose metabolism impairs muscle recovery |
| Nerve pain | Advanced glycation | High blood sugar damages peripheral nerves |
| Pelvic pain | Ovarian enlargement | Multiple cysts stretch ovarian capsule |
| Back pain | Weight distribution | Abdominal weight gain stresses lumbar spine |
Understanding these connections helps you identify which interventions might provide the most relief for your specific pain pattern.
Why Your Doctor Might Miss the PCOS Pain Connection
Most physicians receive limited training on PCOS beyond fertility concerns. They know it affects ovulation and pregnancy chances. The widespread pain component often gets overlooked.
You might hear phrases like “that’s just part of being a woman” or “try losing some weight.” These responses dismiss real, measurable physiological processes causing your discomfort.
The problem compounds when pain appears in locations seemingly unrelated to reproductive health. A rheumatologist treats your joint pain without checking hormone levels. A neurologist addresses your migraines without considering your irregular cycles. Each specialist sees one piece of a larger puzzle.
You need to become your own advocate. Connecting the dots between your PCOS diagnosis and various pain complaints helps you guide your care team toward comprehensive treatment.
Evidence-Based Approaches to Reducing PCOS Pain
Managing PCOS pain requires addressing root causes, not just masking symptoms with pain relievers. Here’s what actually works based on current research:
Metabolic Interventions
Improving insulin sensitivity directly reduces inflammation and pain. This doesn’t mean you need to achieve a specific body weight. It means making your cells more responsive to insulin at whatever size you are.
Strategies include:
- Eating balanced meals with protein, fat, and fiber to stabilize blood sugar
- Engaging in regular movement, particularly resistance training
- Getting adequate sleep to support metabolic hormone regulation
- Managing stress through proven techniques that lower cortisol
The anti-inflammatory diet for back pain offers specific guidance on foods that calm systemic inflammation.
Hormone Regulation
Balancing your reproductive hormones reduces pain fluctuations tied to your cycle. Options include:
- Combined oral contraceptives to create predictable hormone patterns
- Progesterone therapy to oppose estrogen dominance
- Anti-androgen medications to reduce excess male hormones
- Supplements like inositol that improve ovarian function
Work with an endocrinologist or reproductive specialist familiar with PCOS pain management, not just fertility treatment.
Direct Pain Management
While addressing root causes, you still need relief from current symptoms. Effective approaches include:
- Heat therapy for muscle and joint pain
- Gentle stretching and mobility work
- Cognitive behavioral therapy to rewire pain processing
- Targeted medications for specific pain types
The 15-minute daily stretching routine for chronic pain management provides a practical starting point for movement-based relief.
Lifestyle Modifications
Small daily changes accumulate into significant pain reduction over time:
- Maintaining consistent sleep and wake times to support circadian hormone rhythms
- Identifying and avoiding personal food triggers that spike inflammation
- Building stress resilience through meditation, journaling, or therapy
- Creating an ergonomic workspace if you have a desk job
The working woman’s guide to managing chronic pain at your desk job addresses specific challenges for women managing PCOS pain while working.
When PCOS Pain Signals a Complication
Sometimes pain indicates a condition requiring immediate attention. Recognize these warning signs:
- Sudden, severe abdominal pain that doubles you over
- Pain accompanied by fever, nausea, or vomiting
- Chest pain or difficulty breathing
- Severe headache with vision changes or neurological symptoms
- Pain that progressively worsens despite treatment attempts
These symptoms might indicate ovarian torsion, a ruptured cyst, or another acute complication. Don’t wait. Seek emergency care.
Five back pain red flags that mean you should see a doctor immediately covers additional warning signs that apply beyond PCOS-specific concerns.
The Mind-Body Component of Chronic PCOS Pain
Living with chronic pain changes your nervous system. Your brain becomes more efficient at creating pain signals and less effective at filtering them out.
This isn’t psychological weakness. It’s neuroplasticity working against you. Your pain pathways strengthen through repeated activation, making you more sensitive over time.
The good news? You can actually rewire your pain response through targeted interventions. Mindfulness practices, graded exposure to movement, and pain reprocessing therapy all help retrain your nervous system.
“Women with PCOS often develop central sensitization, where their nervous systems amplify pain signals beyond what the original tissue damage warrants. Addressing this neurological component is just as important as treating the metabolic dysfunction.” — Dr. Sarah Mitchell, Pain Medicine Specialist
Understanding why pain becomes chronic helps you recognize when you need interventions targeting your nervous system, not just your ovaries.
Sleep Disruption and PCOS Pain: Breaking the Cycle
Poor sleep intensifies pain. Pain disrupts sleep. This vicious cycle is particularly problematic for women with PCOS, who already face higher rates of sleep apnea and insomnia.
Sleep deprivation increases inflammatory markers and lowers pain thresholds. After even one night of poor sleep, your body produces more pain-promoting chemicals and fewer pain-relieving ones.
PCOS compounds sleep issues through multiple mechanisms:
- Elevated androgens contribute to sleep apnea
- Insulin resistance disrupts normal sleep architecture
- Anxiety about symptoms prevents mental relaxation
- Physical discomfort makes finding comfortable positions difficult
How to sleep better when chronic pain keeps you awake provides specific strategies for breaking this cycle and improving both sleep quality and pain levels.
Comparing PCOS Pain to Other Gynecological Conditions
PCOS pain overlaps with other reproductive conditions, making diagnosis tricky. Understanding the distinctions helps ensure you receive appropriate treatment.
Fibroid pain vs. endometriosis explores how these conditions differ from PCOS, though you can have multiple conditions simultaneously.
Women with PCOS and fibroids face compounded challenges. Both conditions involve hormonal imbalances and can cause similar symptoms. If you’re experiencing unexplained weight changes alongside pain, understanding whether fibroids can cause weight gain helps you identify which condition might be driving which symptoms.
Medication Options That Target PCOS Pain Mechanisms
Different medications address different aspects of PCOS pain. Understanding your options helps you have informed conversations with your healthcare provider.
Comparing pain medications for various pain types can guide your choices, but PCOS-specific considerations include:
- Metformin to improve insulin sensitivity and reduce inflammation
- NSAIDs for acute pain flares, used cautiously to avoid gut inflammation
- Low-dose naltrexone to modulate immune function and pain processing
- Gabapentin or pregabalin for nerve-related pain
- Hormonal contraceptives to stabilize reproductive hormone fluctuations
Some women benefit from nerve blocks and injections for specific pain locations that don’t respond to systemic treatments.
Stress Management as Pain Treatment
Stress doesn’t just make pain feel worse emotionally. It creates measurable physiological changes that amplify pain signals.
Cortisol, your primary stress hormone, increases inflammation when chronically elevated. It also interferes with insulin function, worsening the metabolic dysfunction at the heart of PCOS.
Five stress management techniques that actually reduce physical pain offers evidence-based approaches specifically validated for chronic pain conditions.
The mind-body connection in PCOS pain is bidirectional. Physical symptoms create emotional distress. Emotional distress amplifies physical symptoms. Breaking this cycle requires addressing both components simultaneously.
Building Your PCOS Pain Management Team
Comprehensive PCOS pain management often requires multiple specialists working together. Your ideal team might include:
- A gynecologist or endocrinologist who understands PCOS beyond fertility
- A pain management specialist familiar with chronic pain mechanisms
- A registered dietitian experienced in insulin resistance and anti-inflammatory eating
- A physical therapist who can address musculoskeletal components
- A mental health professional trained in chronic illness and pain psychology
Coordinating care between specialists can be exhausting when you already feel terrible. Consider asking one provider to serve as your primary coordinator, ensuring all team members communicate about your treatment plan.
Tracking Your Pain Patterns for Better Treatment
Identifying your personal pain triggers and patterns provides valuable information for your care team. Keep a simple log noting:
- Pain locations and intensity (scale of 1 to 10)
- Timing relative to your menstrual cycle
- Foods eaten in the previous 24 hours
- Sleep quality and duration
- Stress levels and major events
- Physical activity type and intensity
- Any medications or supplements taken
Patterns emerge over weeks and months. You might notice pain spikes after eating certain foods, during specific cycle phases, or following poor sleep nights. This data helps you and your providers make targeted interventions.
Moving Forward With PCOS Pain
PCOS pain is real, measurable, and treatable. You’re not overreacting. You’re not weak. You’re dealing with a complex endocrine condition that affects your entire body.
The path forward involves patience and persistence. Metabolic improvements take time. Hormonal balance doesn’t happen overnight. Pain reprocessing requires consistent practice.
But small changes compound. Better blood sugar control reduces inflammation. Lower inflammation decreases pain sensitivity. Less pain improves sleep. Better sleep supports metabolic health. The positive cycle builds on itself, just as the negative one did.
Start with one intervention. Maybe it’s adjusting your eating patterns to stabilize insulin. Maybe it’s finally scheduling that appointment with a PCOS-informed endocrinologist. Maybe it’s beginning a gentle stretching routine.
Your pain deserves attention, investigation, and comprehensive treatment. You deserve providers who listen, believe you, and work with you to address the root causes creating your discomfort. Keep advocating for yourself until you find that support.