Living with uterine fibroids means dealing with pain that can interrupt your workday, keep you up at night, and make simple activities feel impossible. The cramping, pressure, and aching can vary from mildly annoying to completely debilitating. You deserve relief that works right now, not weeks from now.
Uterine fibroid pain responds well to multiple at-home strategies including heat application, over-the-counter medications, gentle movement, and dietary adjustments. Most women find relief through a combination of these methods rather than relying on a single approach. Understanding your specific symptoms helps you choose the most effective techniques for your situation.
Understanding Why Fibroids Cause Pain
Fibroids are non-cancerous growths in your uterus that range from pea-sized to larger than a grapefruit. They cause pain through several mechanisms.
Large fibroids press against nearby organs. Your bladder, bowel, or pelvic nerves can all feel the squeeze. This creates a constant dull ache or sharp pressure.
Fibroids also disrupt your normal menstrual cycle. They increase the surface area of your uterine lining, leading to heavier bleeding and more intense cramping. Your uterus works harder to shed this extra tissue.
Some fibroids outgrow their blood supply. When this happens, the tissue starts to break down, causing sudden, severe pain called degeneration. This type of pain feels different from regular cramping.
The location matters as much as the size. A small fibroid pressing on a nerve can hurt more than a large one sitting in a neutral spot.
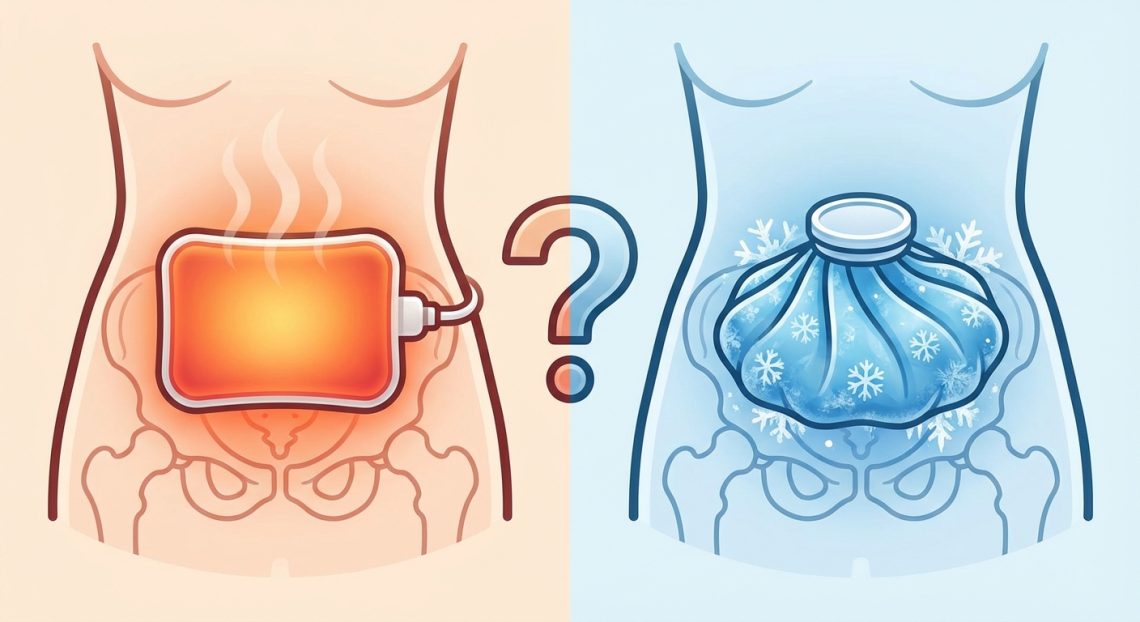
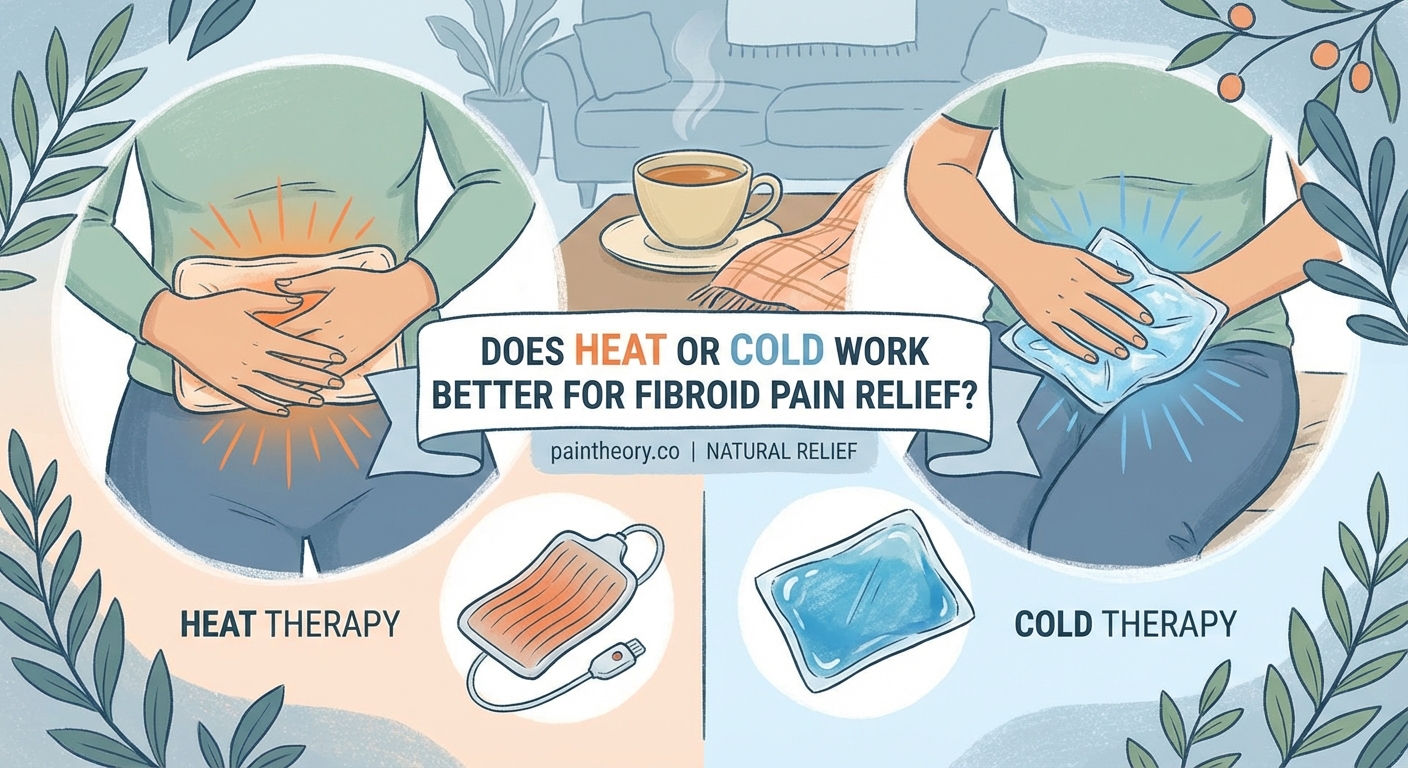
Heat Therapy for Immediate Comfort

Heat remains one of the most reliable tools for fibroid pain relief. It works by relaxing the uterine muscles and improving blood flow to the area.
A heating pad on your lower abdomen or back provides direct comfort. Set it to a moderate temperature and use it for 15 to 20 minutes at a time. You can repeat this throughout the day as needed.
Hot water bottles offer a portable alternative. Fill one before bed and place it where you feel the most discomfort. The sustained warmth helps you sleep better despite the pain.
Warm baths serve double duty. The heat eases your physical symptoms while the quiet time reduces stress. Add Epsom salts for additional muscle relaxation.
Heat patches designed for menstrual cramps work well during your workday. They stick discreetly under your clothing and provide hours of consistent warmth.
“Heat therapy doesn’t shrink fibroids, but it significantly reduces pain perception by interrupting pain signals and relaxing smooth muscle tissue. Many of my patients find it as effective as medication for managing daily symptoms.”
Over-the-Counter Medications That Help
The right pain medication can make a substantial difference in your comfort level.
Ibuprofen addresses both pain and inflammation. Take 400 to 600 mg every six to eight hours with food. This medication works particularly well for menstrual cramping associated with fibroids.
Naproxen lasts longer than ibuprofen. A single dose provides relief for eight to twelve hours. This makes it convenient for overnight coverage.
Acetaminophen helps with pain but doesn’t reduce inflammation. Use it if you can’t tolerate NSAIDs or have stomach sensitivities.
Start taking pain medication at the first sign of discomfort. Waiting until pain becomes severe makes it harder to control.
Never exceed the recommended dosage. If you need pain relief more than a few days per month, talk to your doctor about prescription options.
Movement Strategies That Reduce Discomfort
Physical activity might seem counterintuitive when you hurt, but gentle movement often provides relief.
Walking increases circulation and releases natural pain-relieving endorphins. Even ten minutes around your neighborhood can help. Start slow and listen to your body.
Yoga poses that open the hips reduce pelvic tension. Child’s pose, pigeon pose, and reclining bound angle pose all work well. Hold each position for several breaths.
Swimming takes pressure off your pelvis while keeping you active. The water supports your body weight and allows pain-free movement.
Pelvic tilts strengthen your core and improve posture. Lie on your back with knees bent, then gently rock your pelvis forward and back. This simple exercise reduces lower back pain from fibroids.
Avoid high-impact activities during symptom flares. Running, jumping, and intense workouts can increase pelvic pressure and worsen pain.
Dietary Changes for Symptom Management
What you eat affects inflammation levels and hormone balance, both of which influence fibroid symptoms.
Anti-inflammatory foods should fill most of your plate. Think leafy greens, berries, fatty fish, nuts, and olive oil. These foods help calm the inflammatory response that contributes to pain.
Fiber keeps your digestive system moving. Constipation puts extra pressure on your uterus and worsens pain. Aim for 25 to 30 grams of fiber daily from vegetables, fruits, and whole grains.
Reducing red meat and dairy may help some women. These foods contain compounds that can promote inflammation and affect estrogen levels.
Limit caffeine and alcohol during painful periods. Both can increase inflammation and interfere with sleep, making pain harder to manage.
Stay hydrated. Dehydration intensifies cramping and makes you feel worse overall. Drink at least eight glasses of water daily.
Managing Heavy Bleeding and Related Pain
Heavy menstrual bleeding often accompanies fibroid pain. Addressing the bleeding helps reduce overall discomfort.
Iron supplementation prevents anemia from blood loss. Low iron levels cause fatigue that makes pain feel more overwhelming. Take iron with vitamin C for better absorption.
Tranexamic acid reduces menstrual bleeding by helping blood clot. Your doctor can prescribe this medication to use during your period.
Menstrual cups or period underwear handle heavy flow better than tampons or pads. Less frequent changing means less disruption to your day.
Track your bleeding patterns. Note how many pads or tampons you use, the size of clots, and how many days you bleed heavily. This information helps your doctor assess whether you need additional treatment.
Stress Reduction Techniques
Stress amplifies pain perception. Your nervous system becomes more sensitive when you’re anxious or overwhelmed.
Deep breathing activates your parasympathetic nervous system. Try breathing in for four counts, holding for four, and exhaling for six. Repeat for five minutes.
Progressive muscle relaxation reduces physical tension. Start at your toes and work up, tensing and releasing each muscle group.
Meditation apps provide guided sessions specifically for pain management. Even five minutes daily can change how you experience discomfort.
Adequate sleep is non-negotiable. Pain disrupts sleep, and poor sleep worsens pain. Create a dark, cool bedroom and stick to consistent sleep times.
When Home Remedies Aren’t Enough
Recognizing when you need medical intervention is part of effective fibroid pain relief.
Seek care if your pain interferes with work, relationships, or daily activities. You shouldn’t have to arrange your life around fibroid symptoms.
New or suddenly worsening pain needs evaluation. This could signal fibroid degeneration or another condition requiring treatment.
Heavy bleeding that soaks through a pad or tampon every hour for several hours requires immediate attention. This level of blood loss can be dangerous.
Comparing Relief Methods
| Method | Best For | How Long It Works | Cost |
|---|---|---|---|
| Heating pad | Cramping and muscle tension | 15-20 minutes per session | Low |
| Ibuprofen | Inflammation and moderate pain | 6-8 hours | Low |
| Gentle yoga | Chronic pelvic tension | Cumulative with regular practice | Free to low |
| Dietary changes | Long-term symptom reduction | Weeks to months | Variable |
| Stress management | Pain amplified by anxiety | Immediate and cumulative | Free to moderate |
Creating Your Personal Relief Plan
Effective fibroid pain relief usually requires multiple strategies working together.
- Start with heat therapy as your foundation. Keep a heating pad accessible at home and heat patches in your bag.
- Add appropriate pain medication based on your symptom pattern. Take it proactively rather than waiting for severe pain.
- Incorporate daily movement that feels good. This might be a morning walk, evening yoga, or lunchtime stretching.
- Make one dietary change at a time. Add more vegetables this week, reduce caffeine next week.
- Practice stress reduction daily, even when you feel fine. This builds resilience for difficult days.
Document what works for you. Keep notes about which combinations provide the best relief. Your pattern might differ from someone else’s.
Common Mistakes to Avoid
- Waiting too long to take pain medication
- Using heat for too long and risking burns
- Pushing through severe pain instead of resting
- Trying every remedy at once and not knowing what helps
- Skipping meals, which can worsen inflammation
- Ignoring worsening symptoms that need medical attention
Medical Treatments Worth Discussing
If home strategies provide only partial relief, several medical options can help.
Hormonal birth control often reduces fibroid-related pain and bleeding. Pills, patches, or IUDs can all work depending on your situation.
Uterine fibroid embolization blocks blood flow to fibroids, causing them to shrink. This minimally invasive procedure preserves your uterus.
Focused ultrasound uses sound waves to destroy fibroid tissue without surgery. Recovery time is minimal compared to traditional procedures.
Myomectomy surgically removes fibroids while leaving your uterus intact. This option makes sense if you want to maintain fertility.
Hysterectomy provides permanent relief by removing your uterus. Consider this if you’ve completed your family and other treatments haven’t worked.
Building Your Support System
Managing chronic pain is easier with help.
Talk to your partner or close friends about your symptoms. They can’t read your mind, but they can offer support when they understand what you’re experiencing.
Join online communities for women with fibroids. Hearing how others manage their symptoms provides practical ideas and emotional validation.
Work with your healthcare provider to create a comprehensive plan. Regular check-ins help you adjust strategies as your symptoms change.
Consider working with a pelvic floor physical therapist. These specialists understand how fibroids affect your body and can teach targeted exercises.
Tracking Symptoms for Better Management
Monitoring your symptoms reveals patterns that help you plan ahead.
Note pain intensity on a scale of one to ten. Record the location, quality, and what makes it better or worse.
Track your menstrual cycle. Many women notice their fibroid pain peaks at specific times during their cycle.
Document which relief strategies you try and how well they work. This creates a personalized reference guide.
Share your symptom log with your doctor. Concrete data leads to better treatment recommendations than vague descriptions.
Finding What Works for Your Body
No single approach works for everyone with fibroids. Your symptoms, lifestyle, and preferences all shape what provides the best fibroid pain relief.
Start with the simplest, lowest-risk options. Heat therapy, over-the-counter pain medication, and gentle movement cost little and help most women at least somewhat.
Give each strategy a fair trial. Some methods like dietary changes take weeks to show results.
Be willing to adjust your approach as your symptoms change. Fibroids can grow or shrink over time, and what worked last year might need modification now.
Remember that managing fibroid pain is not about perfection. Some days will be harder than others. Having multiple tools in your relief toolkit means you always have options, even when your go-to method isn’t quite enough.