Standing in the pharmacy aisle, staring at dozens of pain relievers, you’re not alone in feeling overwhelmed. Each bottle promises relief, but which one actually works for your specific pain? The truth is that not all pain medications treat all types of pain equally well. Some excel at reducing inflammation while others simply mask discomfort. Understanding these differences can mean the difference between genuine relief and wasted money on products that won’t help your particular condition.
Pain medications work through different mechanisms, making certain types more effective for specific conditions. NSAIDs like ibuprofen reduce inflammation and work best for arthritis and muscle injuries. Acetaminophen blocks pain signals without reducing swelling, making it ideal for headaches and fever. Opioids affect brain receptors and are reserved for severe pain. Matching your medication to your pain type ensures better relief with fewer side effects.
Understanding the main categories of pain relievers
Pain medications fall into three primary categories, each working through distinct biological pathways.
NSAIDs (nonsteroidal anti-inflammatory drugs) include ibuprofen, naproxen, and aspirin. These medications block enzymes called COX-1 and COX-2 that produce prostaglandins, the chemicals responsible for inflammation and pain signals.
Acetaminophen works differently. It reduces pain and fever by affecting areas of the brain that regulate temperature and pain perception, but it doesn’t reduce inflammation at injury sites.
Opioids like codeine, oxycodone, and morphine bind to receptors in your brain and spinal cord, changing how your nervous system perceives pain signals. These are controlled substances due to their addiction potential.
Topical analgesics deliver medication directly through your skin to affected areas. These include lidocaine patches, capsaicin creams, and diclofenac gels.
Matching medications to your pain type
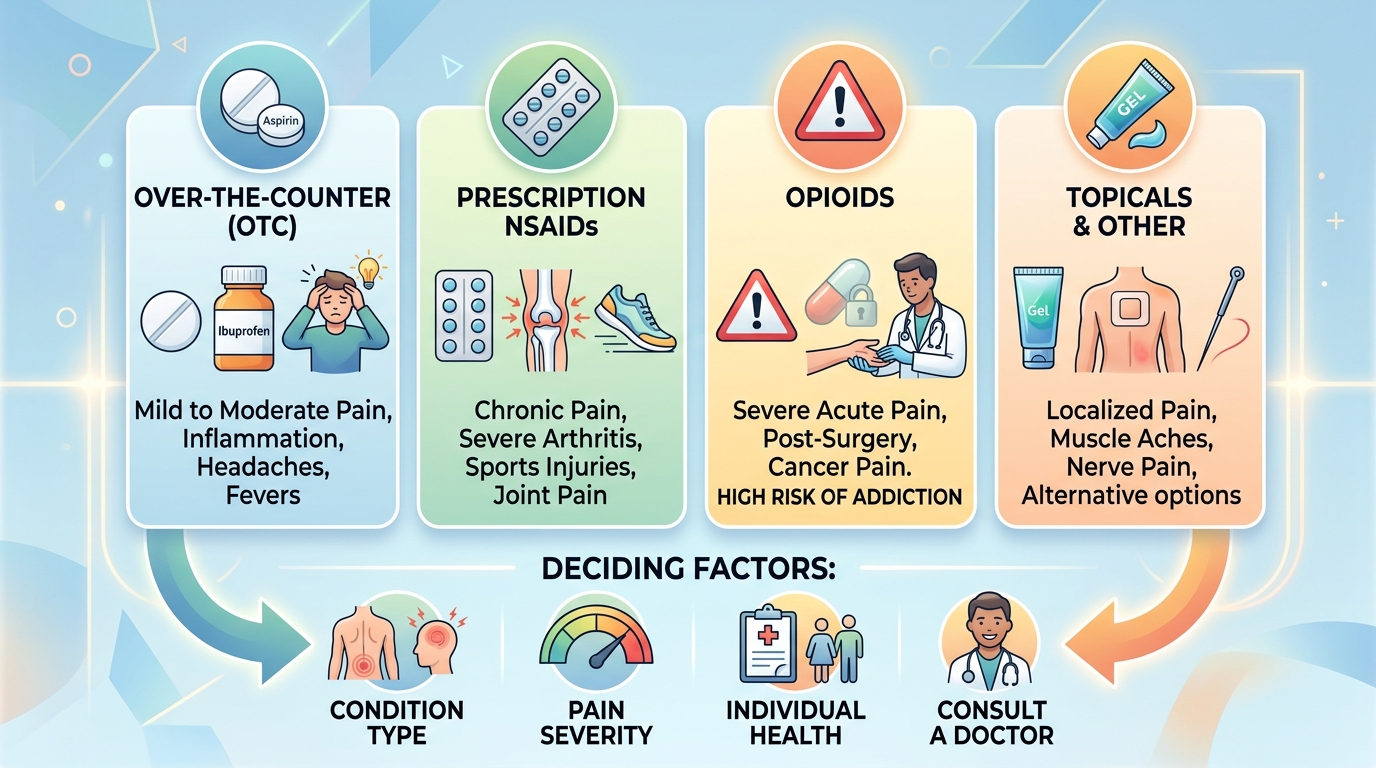
Different pain conditions respond better to specific medication classes.
Inflammatory pain conditions
Arthritis, tendonitis, bursitis, and most sports injuries involve inflammation. NSAIDs work best here because they address the root cause of pain rather than just masking symptoms.
Ibuprofen typically starts working within 30 minutes and lasts four to six hours. Naproxen takes longer to start but provides relief for eight to twelve hours, making it better for conditions requiring consistent coverage.
For chronic inflammatory conditions, your doctor might recommend prescription NSAIDs like celecoxib, which specifically targets COX-2 enzymes and causes fewer stomach issues than traditional options.
Non-inflammatory pain
Headaches, fever, and general aches without swelling respond well to acetaminophen. It’s also the preferred choice if you have stomach sensitivity or bleeding disorders that make NSAIDs risky.
Many people find acetaminophen less effective than NSAIDs for musculoskeletal pain. That’s because it doesn’t reduce inflammation at the injury site.
Nerve pain
Conditions like diabetic neuropathy, shingles pain, and sciatica often don’t respond well to traditional pain relievers. These typically require medications originally developed for other purposes.
Gabapentin and pregabalin, originally anti-seizure medications, calm overactive nerve signals. Certain antidepressants like duloxetine also treat nerve pain by affecting neurotransmitters.
Severe acute or chronic pain
When other medications fail to control pain, doctors may prescribe opioids. These are appropriate after major surgery, for cancer pain, or for severe injuries.
However, the risks of dependence, tolerance, and side effects mean they should be a last resort after other options have failed.
| Pain Type | First Choice | Why It Works | Alternative |
|---|---|---|---|
| Arthritis | Ibuprofen or naproxen | Reduces joint inflammation | Topical diclofenac gel |
| Headache | Acetaminophen | Blocks brain pain signals | Aspirin or caffeine combination |
| Muscle strain | Ibuprofen | Reduces tissue inflammation | Ice plus acetaminophen |
| Nerve pain | Gabapentin | Calms nerve activity | Duloxetine or topical lidocaine |
| Post-surgical | Opioid (short-term) | Changes pain perception | Combination therapy with NSAIDs |
How to choose the right medication for your situation
Follow this process when selecting pain relief:
- Identify whether inflammation is present by checking for swelling, redness, or warmth at the pain site.
- Consider your medical history, including stomach problems, kidney disease, liver conditions, or bleeding disorders.
- Review medications you’re already taking to avoid dangerous interactions.
- Start with the lowest effective dose and increase only if needed.
- Give the medication adequate time to work before switching (at least three to five days for chronic conditions).
- Track your response in a simple journal noting pain levels before and after medication.
Safety considerations you can’t ignore

Every pain medication carries risks that increase with improper use.
NSAIDs can cause stomach ulcers, bleeding, kidney damage, and increased blood pressure. Taking them with food reduces stomach irritation. Never exceed recommended doses, even if pain persists.
Acetaminophen seems gentle but causes liver damage when you take too much. Many cold and flu medications already contain acetaminophen, so check labels carefully to avoid accidental overdose. The maximum safe dose is 3,000 mg daily for most adults, though some experts recommend staying below 2,000 mg.
“People often assume that over-the-counter means completely safe, but acetaminophen overdose remains one of the leading causes of acute liver failure in the United States. Always read labels and account for all sources of the medication you’re taking.” (Dr. Sarah Chen, Pain Management Specialist)
Opioids cause constipation, drowsiness, confusion, and respiratory depression. They also create physical dependence within days to weeks of regular use. Never share prescription opioids or take them longer than prescribed.
Combination strategies that enhance effectiveness
Sometimes using multiple approaches together provides better relief than any single medication.
Acetaminophen and ibuprofen work through different mechanisms, so alternating them every three hours can provide more consistent pain control than either alone. This approach works particularly well for dental pain or injuries.
Adding topical treatments to oral medications targets pain from two directions. A lidocaine patch on your lower back pain that worsens at night combined with an oral NSAID often works better than doubling the oral dose.
Non-medication strategies amplify pharmaceutical relief. Ice reduces inflammation in the first 48 hours after injury. Heat relaxes muscles and improves blood flow to healing tissues. Physical therapy addresses mechanical problems causing pain.
For those wondering about how sleep quality affects pain, improving rest often reduces the amount of medication needed for adequate relief.
When over-the-counter options aren’t enough
Several warning signs indicate you need professional evaluation rather than continued self-treatment:
- Pain lasting longer than two weeks despite appropriate medication
- Increasing pain intensity over time
- Pain that wakes you from sleep consistently
- New symptoms like numbness, weakness, or bowel/bladder changes
- Fever accompanying your pain
- Pain after a significant injury or fall
Understanding why pain becomes chronic helps you recognize when your nervous system needs specialized treatment beyond simple pain relievers.
Your doctor has access to prescription-strength NSAIDs, muscle relaxants, nerve pain medications, and targeted injection therapies. They can also order imaging or tests to identify treatable underlying causes.
In some cases, surgical intervention becomes appropriate when medications only mask symptoms of a structural problem.
Special considerations for specific conditions
Certain health conditions require modified approaches to pain medication.
Pregnancy and breastfeeding
Acetaminophen is generally considered safe throughout pregnancy. Most NSAIDs should be avoided, especially in the third trimester when they can affect fetal heart development.
Always consult your obstetrician before taking any medication while pregnant or nursing.
Kidney disease
NSAIDs can worsen kidney function and should be used cautiously or avoided entirely in people with chronic kidney disease. Acetaminophen is usually safer for this population.
Liver disease
Acetaminophen doses must be reduced significantly in people with liver problems. NSAIDs become the preferred option if stomach and kidney function are adequate.
Heart disease
NSAIDs can increase blood pressure and fluid retention, potentially worsening heart failure. They may also increase heart attack and stroke risk, especially with prolonged use.
Aspirin in low doses protects against heart attacks but doesn’t provide much pain relief at those doses.
Bleeding disorders
People taking blood thinners or with clotting disorders should avoid most NSAIDs and aspirin, which interfere with platelet function. Acetaminophen is usually the safer choice.
Common mistakes that reduce effectiveness
Avoid these errors that prevent medications from working optimally:
- Taking medication only when pain becomes severe rather than maintaining consistent levels
- Mixing multiple products containing the same active ingredient
- Taking NSAIDs on an empty stomach
- Expecting immediate results from medications that need several days to reach full effect
- Stopping medication too soon when treating inflammatory conditions
- Ignoring maximum daily dose limits
- Drinking alcohol while taking acetaminophen or NSAIDs
- Crushing or breaking extended-release formulations
Reading labels like a professional
Understanding medication labels prevents dangerous mistakes.
The active ingredient section tells you what’s actually treating your pain. Generic names like “ibuprofen” or “acetaminophen” matter more than brand names.
The “Drug Facts” panel lists the purpose, uses, warnings, directions, and inactive ingredients. Pay special attention to warnings about interactions with other medications or health conditions.
Check the expiration date. Medications lose potency over time, and some become dangerous when expired.
Note whether the product is immediate-release or extended-release. Extended-release formulations should never be crushed, chewed, or broken, as this dumps the entire dose at once.
Cost-effective choices that don’t sacrifice quality
Brand-name medications and generics contain identical active ingredients at the same strengths. The FDA requires generics to meet the same quality standards as brand names.
Buying larger quantities typically costs less per dose. A bottle of 500 tablets costs much less per pill than a bottle of 50.
Store brands from reputable pharmacies offer the same formulations as national brands at 30-50% lower prices.
Prescription NSAIDs sometimes cost more than over-the-counter options at higher doses. Ask your doctor if taking multiple over-the-counter tablets would work as well and cost less.
Finding the right fit for your lifestyle
Your daily routine should influence medication choice.
If you need consistent coverage throughout the workday, longer-acting naproxen taken twice daily beats ibuprofen requiring doses every four to six hours.
People who forget to take medications benefit from once-daily options or extended-release formulations.
Athletes and active individuals should time NSAID doses around activity. Taking ibuprofen 30 minutes before exercise prevents inflammation from building up during workouts.
For conditions with cyclical pain patterns, timing medication to start before pain typically worsens provides better control than waiting for symptoms to appear.
Making informed decisions about your pain relief
Choosing the best pain medication for your condition requires understanding how different drugs work, matching them to your specific type of pain, and considering your individual health factors.
Start with the safest, most appropriate option for your pain type. Give it adequate time to work at the recommended dose. Track your results honestly. Adjust your approach based on response, not assumptions.
Remember that medication is just one tool in pain management. Combining pharmaceutical options with physical therapy, lifestyle modifications, and addressing underlying causes provides the most complete and lasting relief.
Your pain deserves treatment that actually works for your body and your condition. Armed with this comparison guide, you can make choices that provide real relief while minimizing risks and side effects.